Definition of dementia
The term “dementia” comes from the Latin de mens and means “without mind” or “out of one’s mind”. It is a generic term for various diseases that lead to a permanent decline in higher brain functions. Today, “dementia” is referred to as a “major neurocognitive disorder”.
The diagnosis of major neurocognitive disorder requires evidence of a significant decline in cognitive performance relative to the previous level of performance in one or more cognitive domains, which must be objectified by standardized neuropsychological testing or other qualified clinical assessment, and there is no evidence of an alternative cause.
The relevant cognitive areas include:
- Learning and memory
- Speech disorders (aphasia)
- Perception and motor functions
- Executive functions
- Complex attention functions
- Social cognition
Dementia or a major neurocognitive disorder develops over at least six months and progresses chronically. Consciousness and sensory perception usually remain intact, but the ability to lead an independent life increasingly declines.
Frequency of dementia
There are currently around 161,000 people living with dementia in Switzerland.
- Around 34,800 new cases occur every year.
- Women are significantly more frequently affected due to their higher life expectancy (approx. 70% of all cases).
- At around 60%, Alzheimer’s disease is the most common form.
- Only rarely do younger people develop dementia.
Due to demographic trends, the number of people affected will continue to increase in the coming decades.
Forms of dementia
The cause of dementia is a brain disease, i.e. a neurological disorder in which nerve cells die (neurodegeneration) or blood flow to the brain is impaired.
- Alzheimer’s disease: At 60 percent, Alzheimer’s disease is the most common form of dementia. Alzheimer’s is a neurodegenerative disease that progresses gradually and is usually characterized by memory impairment. The incidence of Alzheimer’s disease increases with age.
- Vascular dementia: Vascular dementia is the second most common type of dementia. It is caused by a chronic circulatory disorder of the brain (arteriosclerosis), a stroke or a combination of these two factors. The most important risk factors are high blood pressure, diabetes, high cholesterol levels, obesity and smoking.
- Mixed forms: There are also mixed forms between Alzheimer’s disease or the other forms of dementia mentioned below and vascular dementia.
- Frontotemporal dementia: Another neurodegenerative disease that can lead to dementia is frontotemporal dementia (FTD), formerly known as Pick’s disease. The focus here is less on memory disorders and more on behavioral and speech disorders. The age of onset is usually younger than that of Alzheimer’s dementia.
- Parkinson’s dementia: Over time, people with Parkinson’s disease can also develop signs of dementia, known as Parkinson’s dementia.
- Lewy body dementia / Lewy body dementia: As in Parkinson’s disease, pathological synuclein proteins are deposited in the brain in Lewy body dementia, but not primarily in the motor centers, but diffusely distributed. Patients with Lewy body dementia usually have milder Parkinson’s symptoms and often fluctuating cognitive performance in addition to limitations in higher brain functions.
- Prion diseases: In Creutzfeld-Jakob disease, incorrectly folded proteins are deposited in the brain nerve cells, often leading to rapidly progressing dementia.
The exact differentiation of the form of dementia is crucial in order to plan the best possible treatment and support, as the course, symptoms and therapeutic approaches can vary significantly depending on the cause.
Causes and risk factors of dementia
The development of dementia is the result of various pathological changes in the brain. Depending on the form of dementia, these processes can vary, but ultimately lead to nerve cells and their connections being damaged or destroyed.
Medically, the following main mechanisms can be distinguished:
- Neurodegeneration: Progressive breakdown of nerve cells and nerve cell connections, as in Alzheimer’s dementia, frontotemporal dementia or Lewy body dementia.
- Vascular damage: Chronic or acute circulatory disorders in the brain, as occur in vascular dementia.
- Combination of several causes: Mixed forms in which there are both neurodegenerative and vascular changes.
- Special disease processes: Protein deposits in prion diseases or inflammatory and metabolic diseases that can cause secondary dementia.
Important risk factors
Certain factors increase the risk of developing dementia or influence the course of the disease:
Many of these risk factors are easy to influence. A healthy lifestyle with a balanced diet, regular exercise and mental activity can reduce the risk of dementia and have a positive influence on the course of the disease.
Symptoms and signs of dementia
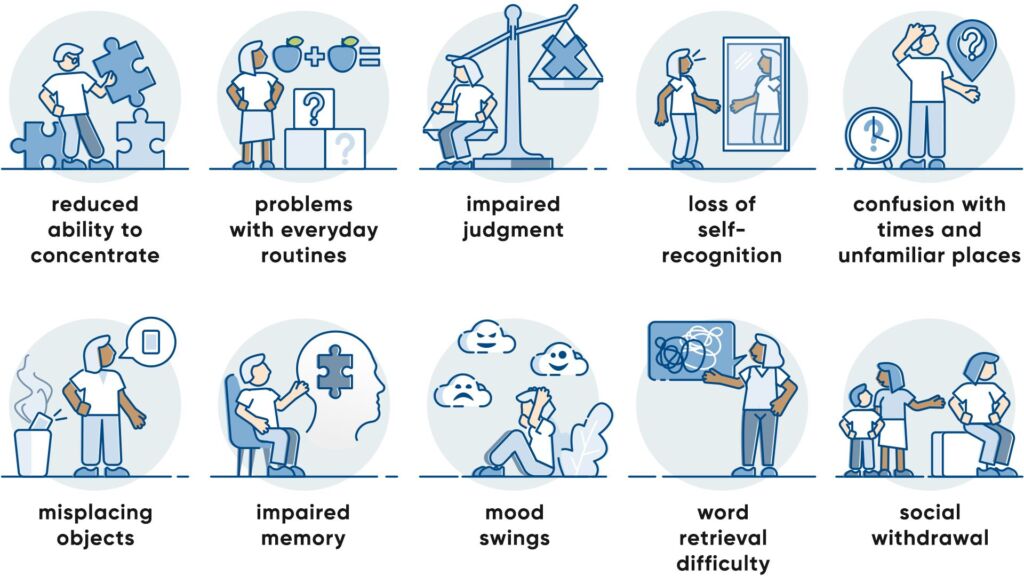
The first signs of dementia usually develop gradually and can vary depending on the form of dementia. Common symptoms include memory problems, especially for recent experiences, difficulties with orientation in time and space, language problems (e.g. word-finding difficulties) and difficulties with everyday activities. Changes in personality or social behavior, a decline in the ability to judge and make decisions and attention disorders can also occur. As the disease progresses, the cognitive impairments increase and can ultimately make it impossible to lead an independent life.
Dementia diagnosis
The diagnosis of dementia requires a comprehensive medical and neuropsychological assessment to determine the type of dementia and rule out other, treatable causes. First, the symptoms, their onset and progression are recorded, supplemented by a survey of relatives.
Important diagnostic steps are
- Neuropsychological examination with assessment of memory, language, orientation, attention and other cognitive functions by means of a detailed neuropsychological examination.
- Neurological examination to record motor, sensory and coordinative functions.
- Imaging procedures such as magnetic resonance imaging (MRI) or computer tomography (CT) to detect structural changes, circulatory disorders or tumors.
- Laboratory tests to identify treatable causes (e.g. vitamin deficiency, thyroid disease, infections).
- If necessary, special examination procedures such as cerebrospinal fluid tests or nuclear medicine imaging (PET, SPECT) to differentiate the form of dementia more precisely.
An early and precise diagnosis is crucial in order to initiate the appropriate therapy and supportive measures and to provide the best possible advice to those affected and their relatives.
Differential diagnosis: Other causes of dementia-like symptoms
Not every impairment of higher brain functions automatically means dementia. There are various diseases or conditions that can cause similar symptoms such as memory loss, speech problems or disorientation – without the presence of a primary, incurable dementia. Some of these causes are treatable, which is why it is particularly important to recognize them during the investigation:
- Alcohol abuse: Long-term excessive alcohol consumption can damage the frontal and temporal lobes of the brain in particular. This can lead to severe memory impairment, known as Korsakov’s syndrome.
- Infectious brain diseases: Chronic inflammation of the brain, e.g. in HIV infection (AIDS dementia) or syphilis (progressive paralysis), can cause cognitive impairment.
- Space-occupying processes in the brain: Brain tumors or excess pressure in the cerebrospinal fluid system (hydrocephalus) can affect the brain mechanically and thus cause symptoms similar to those of dementia.
- Metabolic and deficiency conditions: Diseases such as hypothyroidism, diabetes mellitus or a severe vitamin deficiency (especially vitamin B12 deficiency) can significantly reduce mental performance.
- Mental illness: Depression can cause symptoms that sometimes resemble dementia. Existing dementia can also be exacerbated by depression.
Treatment details
In most cases, dementia cannot be cured, but drug and non-drug measures can often slow down the progression and improve quality of life. Treatment depends on the underlying form of dementia and – depending on the situation – includes medication, cognitive training, physiotherapy and psychosocial support for those affected and their relatives.
The prognosis varies greatly depending on the form of dementia, general condition and accompanying illnesses. On average, life expectancy after diagnosis is between six and ten years, and even longer in very slowly progressing forms. Starting treatment early and providing holistic care can help to maintain independence for as long as possible and avoid complications.
Details of the treatments
Support and tips for relatives of dementia patients
Relatives play a central role in the care of people with dementia. The disease often presents them with major challenges. Good preparation and sharing experiences with others can help you to cope better with everyday life and not neglect your own health.
- Information and knowledge: Understand that the behavioral changes are part of dementia and are not directed at you personally.
- Adapt communication: Speak in short, clear sentences. Show patience and use non-verbal communication such as touch or eye contact. Avoid confrontations or unnecessary discussions.
- Structured daily routine: A regular daily routine provides security. Involve the person concerned in simple activities to maintain their independence for as long as possible.
- Know your own limits: The care is exhausting. Take time out, ask friends or family members for support or make use of respite services such as day centers or short-term care.
Seek support: Sharing experiences with people who are equally affected can be very helpful. Self-help groups offer a safe space to share experiences and receive valuable advice. You can also find out about support options from specialist advice centers or the University Hospital Zurich, e.g. Alzheimer Zurich.
Self-help groups
The exchange with people who are affected by the same disease can be a great support in coping with the disease. Advice on finding a suitable self-help group is available from Selbsthilfe Zürich. Self-Help Zurich and the University Hospital Zurich are cooperation partners in the national project “Health literacy thanks to self-help-friendly hospitals”.
Frequently asked questions about dementia
Dementia is a generic term for various diseases that lead to a progressive decline in mental abilities. Alzheimer’s disease is the most common form of dementia (around 60% of cases) and is caused by specific protein deposits in the brain. In addition to Alzheimer’s disease, there are also other defined forms of dementia such as vascular dementia, Lewy body dementia or frontotemporal dementia.
Typical symptoms of Alzheimer’s disease are memory disorders – especially for recent experiences – as well as orientation problems, speech disorders and difficulties with everyday tasks. This is often accompanied by behavioral changes such as withdrawal, irritability or mood swings. Other forms of dementia can manifest themselves with other symptoms, for example behavioral abnormalities and impaired speech functions in fronto-temporal dementia or impaired movement patterns and even Parkinson’s disease in Lewy body disease.
Medically, the progression of Alzheimer’s disease is usually divided into three stages: Early stage with mild memory impairment, middle stage with significant limitations in everyday life and late stage with severe cognitive and physical impairment. Some models speak of four phases, whereby the early stage is divided into a very early (“preclinical”) phase and a mild dementia phase. This stage classification cannot always be used for other forms of dementia.
Early signs of Alzheimer’s disease can be: frequent forgetting of current events, difficulties in planning or organizing, orientation problems in familiar surroundings, word-finding difficulties, declining decision-making ability and changes in social behavior. Other forms of dementia can manifest themselves with other symptoms, for example behavioral abnormalities and impaired speech functions in fronto-temporal dementia or impaired movement patterns and even Parkinson’s disease in Lewy body disease.
In most cases, Alzheimer’s disease initially affects short-term memory – those affected forget recent events, appointments or conversations. Memories from childhood and adolescence often last longer at first.
Early warning signs of Alzheimer’s disease are memory lapses in everyday life, difficulties in expressing or understanding language, orientation problems, conspicuous errors in familiar activities, reduced attention and mood swings or withdrawal from social contacts.
In the late stages – regardless of the form of dementia – those affected are completely dependent on care. They lose the ability to speak, move independently and eat. Complications such as infections or swallowing disorders often occur, which can be life-threatening.
People with the onset of Alzheimer’s disease often appear forgetful, withdraw or react more irritably than before. They have difficulty following conversations, finding their way in unfamiliar surroundings or coping with complex tasks. Many people deliberately cover up these problems at first.
Those affected rarely die directly from dementia. The most common causes of death are late-stage complications, such as pneumonia (often due to swallowing disorders), infections or general weakness with secondary diseases.
The course of the disease varies from person to person. On average, the condition deteriorates over several years – usually slowly over six to ten years in the case of Alzheimer’s, but often more quickly in the case of other forms such as frontotemporal dementia or prion diseases.
A cure is currently not possible. Medication can slow down the progression of certain forms, and non-pharmacological measures such as memory training, physical activity and social contact can improve quality of life. Treatment is individually tailored to the form of dementia and the patient’s state of health.
Most forms of dementia are not directly hereditary. However, there are genetic risk factors that can increase the likelihood of developing the disease – especially in rare, familial early forms of Alzheimer’s or frontotemporal dementia. In most cases, however, environmental and lifestyle factors play a greater role than genetic predisposition.




