Brain surgery on an awake person places special demands on the team and the patients.
The idea is strange at first: an operation on the brain while the patient is wide awake, answering questions, reading something out loud or even singing. Luca Regli, Director of the Department of Neurosurgery, understands this. He and his team operate on a patient almost every week in a so-called awake operation. But why not let people sleep through the procedure under deep anesthesia? “We can also perform the procedures that we do on awake patients under anesthesia,” explains Luca Regli. “If someone is awake, however, we receive information from them directly during the operation, which we can use to work even more precisely and safely. This improves the outcome of the operation.” The surgical method is primarily used where precision and safety are required to the highest degree: for tumor removal in the brain and for functional interventions such as deep brain stimulation in Parkinson’s patients.
Operating as gently as possible
In principle, the procedure is always the same: during the operation, the area of the brain being operated on is stimulated with electrical impulses. Based on the patient’s reaction to these impulses, doctors can localize exactly where they can make incisions without causing damage to brain function, or whether they have precisely targeted an area to be stimulated. In the case of Parkinson’s patients, it can be determined during the operation whether the electrodes for deep brain stimulation have been optimally placed and whether the tremors typical of this disease have been successfully stopped. “When removing a tumor, the aim is to remove the tumor tissue as completely as possible while causing as little damage as possible to the surrounding brain tissue,” explains Luca Regli. “These tumors are often located near the speech center. This is a delicate location, because even tiny distances can determine whether or not the patient loses their ability to speak as a result of the operation. If the person is awake during the operation, we can determine the boundaries at the transition from tumor tissue to healthy tissue much more precisely based on their reaction.” In simple terms, this means that before the surgeons make an incision, the corresponding area of the brain is stimulated via a probe and the patient is asked to speak or read. Changes in his or her ability to express himself or herself allow the doctors to see whether the next incision will already damage the speech center or whether they can still safely remove tissue.
If patients are under anesthesia during such an operation, the result of the operation can only be determined once they are awake again. A new intervention would be necessary to correct the position of an electrode, for example, and damage to the speech center would be irreversible. And unfortunately, in many cases brain tumors only become noticeable when they are already well advanced. Some tumor patients have only recently learned of their serious illness, and sometimes their remaining life expectancy has suddenly shrunk to just a few weeks. Against this background, maintaining the ability to speak is of immense importance.
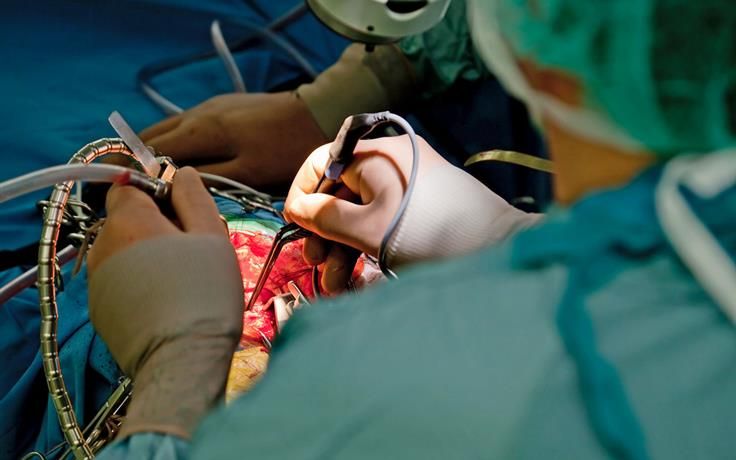
Highly specialized teamwork
In terms of surgical technique, awake operations are no different from operations in which patients are asleep. “The fact that people are awake places completely different, very high demands on the whole team,” says Luca Regli. “The patients are in a very special situation. They see everything and are even actively involved in the operation. They are tense and uncertain, even though we naturally explain exactly how the procedure will work and discuss the opportunities and risks before they decide to have the operation. Our aim is therefore for our patients to trust that we will do everything we can to achieve the best result for them and make them feel as comfortable as possible. This includes, for example, working extremely quietly so that interaction with the patient is not disturbed. And always keeping calm in critical situations. The patients should go into the operation without fear of pain and know that we won’t leave them alone.”
A highly specialized and experienced interprofessional team therefore performs the procedures at the Department of Neurosurgery. In addition to surgeons, anesthetists and nurses, electrophysiologists, speech therapists and neuropsychologists, physiotherapists and occupational therapists are also involved. Monika Grimm, head of department in the operating theater, has been involved in awake operations for years. “We feel differently than when someone is asleep and relaxed. For patients, an operation like this is incredibly physically and emotionally demanding and stressful. Many have never been in an operating theater before, and then they have to undergo several hours of brain surgery while being awake and worrying and hoping that everything will go well. The noises are strange, the horror when your own voice sounds strange during a stimulation test or your articulation temporarily fails completely.” However, Monika Grimm also remembers a singer who even sang during the operation. When the trembling of Parkinson’s patients’ hands caused by the disease suddenly stops as a result of the intervention, it is a gratifying moment: “We know that it massively improves their quality of life. So it’s only understandable that patients sometimes burst into tears from exhaustion after all the effort.” And Monika Grimm can only agree with Luca Regli that these interventions demand a lot from everyone. “The concentration and long periods of standing are exhausting for us too. But we carry our patients and each other through these hours as a team.”
Pain-free brain surgery
Christian Möhrlen is part of the team as an anesthesiologist. His aim is also to provide patients with as much relief as possible. “The brain matter is insensitive to pain. That’s why such operations are feasible at all. But the scalp and part of the meninges are sensitive, and opening the skullcap is very unpleasant, the drilling hums like at the dentist, but much louder.” The necessary straining of the head and lying down for long periods can also be painful. In addition to a regional anesthetic to relieve the pain of the incision in the scalp, Christian Möhrlen therefore puts the patients into a half-sleep at the beginning and end, from which he then wakes them up again for the decisive steps of the operation. It is extremely rare for cramps or bleeding to occur during surgery. The anaesthetist is therefore always ready to stabilize the patient in the event of complications and, if necessary, to induce a general anaesthetic so that the operation can still be completed. Speech therapists and neuropsychologists play an important role in awake operations. They accompany patients during the assessment, during the operation and during follow-up examinations. Nicole Schmid, Head of Neuropsychology at the USZ, is one of them. “The surgeons have a lot of experience and a good sense of which patients they can even suggest awake surgery to. However, if a patient decides in principle in favor of this, we also carefully clarify whether he or she can withstand the psychological stress of such an operation.”
Reference tests before the operation
Once the decision has been made, speech therapists and neuropsychologists carry out detailed tests with the patients and have long discussions with them. They serve the neuropsychologists as a reference for the operation. This is because in order to correctly assess the changes in speech, word finding problems or changes in breathing triggered by the stimulation, they need to know how the person articulates, reads, speaks or breathes before the operation. “The location of the tumor also provides information about the changes we have to expect when stimulating the brain areas in order to provide surgeons with the right information.” If the tumor is on the right side, patients usually have more difficulty with speech, articulation, voice or breathing. If the tumor is in the left hemisphere of the brain, the patient is more likely to be unable to read or write, to understand what he or she has read, or to miss words. During surgery on tumors located in critical proximity to speech-relevant brain areas, the neuropsychologists and speech therapists are the faces that the fixed patients see. Because they have to notice not only changes in spontaneous speech and speech comprehension, but also the smallest changes in the patient’s facial motor skills that could indicate complications, they spend these hours very close to the patients. Some patients are helped by the fact that they can actively contribute to the operation, while others still feel very exposed. “During the long operation, people also experience phases of fatigue or suffer psychological crises. This is another reason why it is essential that they can always see someone. The pre-operative clarifications give us a relationship of trust with the patients. We also try to help them get through these moments psychologically so that we can carry out the operation with the patient’s full cooperation.”