Overview: What is a streptococcal infection?
Streptococcal infections are diseases caused by a specific type of bacteria known as streptococci. These bacteria occur naturally in humans in the mouth, throat, on the skin, in the intestines or in the vagina and are largely harmless.
Only when streptococci multiply strongly in the body and penetrate the tissue can they cause disease. The throat, nose, tonsils, ears, lungs, inner lining of the heart (endocardium) and the brain are frequently affected. In severe cases, a streptococcal infection can lead to sepsis (colloquially known as blood poisoning).
What diseases can be caused by streptococci?
Streptococci can cause many different diseases. Depending on the type of bacteria, different diseases can occur. Examples are:
Group A streptococci(Streptococcus pyogenes):
- Inflammation of the throat and pharynx (pharyngitis)
- Tonsillitis (tonsillitis, angina tonsillaris)
- Otitis media
- Sinusitis
- Scarlet fever
- Skin infections such as contagious lichen (impetigo contagiosa) or erysipelas (erysipelas)
- Severe infections such as blood poisoning (sepsis), toxic shock syndrome or necrotizing fasciitis
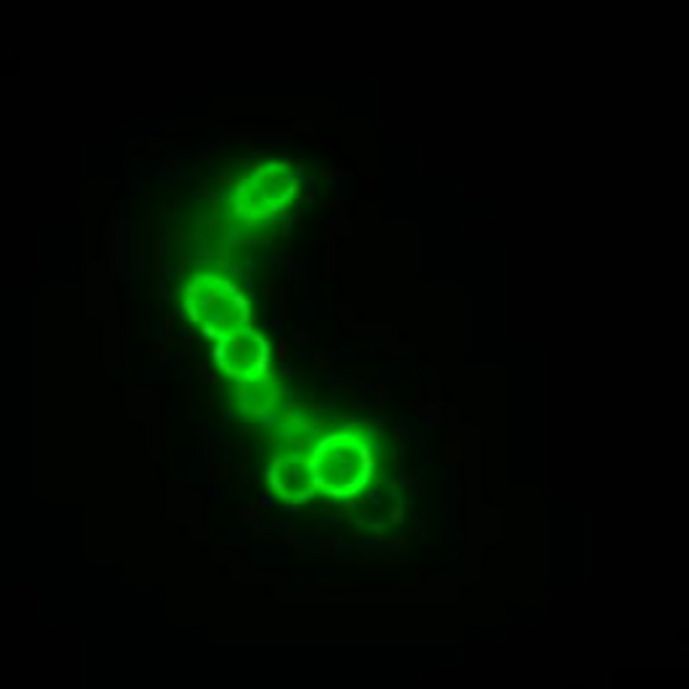
Streptococcus pyogenes (Photo: © K. Schilcher)
Group B streptococci(Streptococcus agalactiae):
Pneumococci(Streptococcus pneumoniae):
Oral streptococci(Streptococcus viridans)
Many streptococcal infections are contagious and can easily be transmitted from person to person. The risk of infection is particularly high with A streptococci.
Causes and risk factors: How is streptococcus transmitted?
Streptococci can be transmitted in various ways – either directly from one infected person to another or indirectly via the environment. Common transmission routes are:
Direct contact
- Skin-to-skin contact with infected areas (e.g. erysipelas, scarlet fever rash or infected wounds).
- Certain types of streptococci – especially Streptococcus pyogenes – can also be transmitted directly from person to person through close contact via droplets (speaking, coughing, sneezing).
Indirect contact
- Via objects that have come into contact with infectious secretions (e.g. handkerchiefs, towels, bed linen, toys).
From mother to child
- Group B streptococci in particular can be transmitted to the newborn during birth.
Certain factors increase susceptibility to infection:
- Weakened immune system due to illness, medication or stress
- Age at risk: young children and the elderly
- Close contacts, for example in families, daycare centers or schools
- Pre-existing conditions such as diabetes or lung diseases
- Skin injuries facilitate the penetration of bacteria
Streptococci during pregnancy: How can children be protected from group B streptococci (GBS)?
Certain streptococci – the so-called group B streptococci (GBS) – can be transmitted from mother to child during birth. Many women carry these bacteria in their intestines or vagina without realizing it. They are usually harmless for the mother. However, they can be dangerous for a newborn baby: If the baby comes into contact with the bacteria at birth, it can in rare cases develop a serious infection, for example blood poisoning, pneumonia or meningitis.
Streptococcus test during pregnancy
To reduce the risk of severe infection, systematic screening for GBS has been recommended in Switzerland since 2019. For this purpose, a swab is taken from the vagina and rectum between the 35th and 37th week of pregnancy. If the streptococcus test is positive, the mother is given an antibiotic in her vein as a precaution during the birth. This largely prevents transmission to the child and significantly reduces the number of serious newborn infections.
Symptoms of streptococcal infection: How do I recognize a disease?
The symptoms depend on which part of the body is affected and which type of streptococcus has caused the infection. Common signs are
- Throat and pharynx: Sore throat, difficulty swallowing, reddened tonsils, sometimes white coating
- Fever and general feeling of illness: tiredness, headache, aching limbs
- Skin: reddish rashes, blisters or inflamed wounds
- Ears and paranasal sinuses: Pain, feeling of pressure, blocked nose
- Lungs: cough, breathing difficulties, fever (with pneumonia)
- Rare, severe infections: Blood poisoning, inflammation of the inner lining of the heart or muscles, toxic shock syndrome
Some infections, such as mild skin infections or tooth decay, go almost unnoticed, while others, such as scarlet fever or tonsillitis, show clear symptoms.
Diagnosis and examination of streptococcal infection: when should I see a doctor?
You should consult a doctor if you experience typical symptoms such as severe sore throat, high fever, pronounced skin rashes or rapidly worsening symptoms.
For diagnosis, the doctor usually checks
- Physical examination: Throat, skin, ears or other affected areas are checked.
- Swab or blood test: A throat swab, skin swab or blood test can detect streptococci.
Early medical clarification is particularly important for small children, older people or people with a weakened immune system, as streptococcal infections can be severe without treatment.
Treatment of streptococcal infection: usually antibiotics
Severe streptococcal infections are treated with antibiotics that specifically combat the bacteria. Early treatment helps to cure the infection more quickly and avoid complications such as severe inflammation or blood poisoning.
Minor infections, such as mild skin inflammation or tooth decay, can sometimes be treated locally without the need for antibiotics.
Streptococcal infection prognosis
Most streptococcal infections are easily treatable. With early diagnosis and treatment, infections such as sore throats, tonsillitis or skin infections usually heal completely within a few days to weeks.
However, if left untreated, some infections can cause complications, e.g. blood poisoning, inflammation of the inner lining of the heart or kidney problems. Timely medical treatment is therefore particularly important, especially for young children, the elderly or people with a weakened immune system.
Streptococcal infection: complications and late effects
If a streptococcal infection is not recognized or treated in time, serious complications can develop. Anyone with severe symptoms such as high fever, severe sore throat, skin rashes or a sudden deterioration in health should seek medical help quickly.
Streptococcal infection: prevention, early detection
Streptococci are widespread, but you can still prevent acute infections:
How to protect yourself from streptococcal infections
The best precaution is to follow simple hygiene rules:
- Wash hands regularly: Especially after contact with other people, public surfaces or pets. This significantly reduces the number of germs on the skin.
- Observe coughing and sneezing etiquette: Cough or sneeze into a handkerchief or the crook of your arm to prevent droplets that may contain bacteria from spreading into the environment. Dispose of tissues immediately and wash your hands afterwards.
- Avoid contact with infected persons: Close physical contact, kissing or sharing utensils with sick people increases the risk of infection. Caution is advised, especially in schools, daycare centers and care facilities.
- Do not share personal items: Cutlery, glasses, towels or toothbrushes should only be used by one person at a time. This will prevent bacteria from being transferred from one person to another.
- For newborns: Pregnant women can be tested for B streptococci. If a positive result is found, they are given an antibiotic during the birth to protect their child.
Good prognosis with early medical clarification
At the first signs of an infection – such as a sore throat, skin rash or fever – it is advisable to seek medical advice as soon as possible. This allows infections to be treated more quickly and complications to be avoided.
Is there a vaccination against streptococcus?
There is currently no vaccination against most streptococci that cause sore throats, tonsillitis or skin infections. The only exception is pneumococci. These bacteria can cause pneumonia, meningitis or blood poisoning. The pneumococcal vaccination is particularly recommended for children, the elderly and people at increased risk in order to prevent serious illness.
