May 28 is World Blood Cancer Day. The most important answers about leukemia, its treatment and blood stem cell transplants.
Text: Danica Gröhlich, editor at “GESUNDHEITHEUTE”
Dr. Müller, every year 1100 people in Switzerland are diagnosed with leukemia. What does research know about the cause?
Basically, leukemias are malignant degenerations of blood formation in the bone marrow. This leads to an uncontrolled proliferation of cells. Little is known about the causes of leukemia. However, we know that certain toxic substances, such as gasoline or radiation exposure as in Chernobyl, can lead to an increased incidence of leukemia. In rare cases, familial clusters occur. After previous cancer therapy, for example breast cancer or lymph node cancer, there is also an increased risk of developing acute leukemia at a later stage. Diet and hormones play a role in the development of some types of cancer. In acute leukemia, however, there are no clear causes that can be avoided.
What types of leukemia are there?
Essentially, we divide the types into lymphatic leukemia, which is common in children and occurs somewhat less frequently in adults. Acute myeloid leukemia is much more common in adults. A distinction is also made between acute forms, which are very aggressive and lead to death within a short time if left untreated, and chronic forms with a slower course. Acute leukemia accounts for three percent of all cancers. Men are more frequently affected, at over 60 percent. As genetic changes accumulate over the course of a lifetime, almost half are over 70 years old at the time of diagnosis.
What signs do leukemia patients have?
Mostly relatively unspecific symptoms such as tiredness, fatigue, often long-lasting infections, also gums and nosebleeds. Immature blood cells, which normally only occur in the bone marrow, then become visible in the blood count. In addition, healthy blood cells such as red blood cells, platelets and mature immune cells can be significantly reduced. A puncture of the bone marrow in the pelvis is performed under local anesthesia to confirm the diagnosis and classify the leukemia precisely. It is often possible to see whether healthy maturation has been displaced by immature leukemia cells. This examination is also important because it allows us to divide leukemia into one of around 50 subgroups, which helps with the prognosis and certain therapy adjustments.
Is a cure possible?
The prognosis of the various subtypes of leukemia is sometimes very different. While acute leukemia in children can very often be cured, only very rare subgroups of acute myeloid leukemia, known as promyelocytic leukemia, have a cure rate of over 90 percent in adults, whereas most other types of leukemia are more difficult to cure. Stem cell transplants are usually performed for some leukemias and also for relapses, provided the patients are fit enough. However, many leukemia patients have pre-existing conditions such as a heart attack or stroke due to their advanced age, which makes treatment more difficult. We then have to decide together whether the person can still undergo intensive chemotherapy or whether the risk of death is too high.
Palliative forms of therapy that aim to prolong life with the best possible quality of life are then also considered for relief. A blood stem cell transplant from a foreign donor also corresponds to immunotherapy. This is because not only blood stem cells are transferred, but also a cell mixture containing long-lived immune cells of the donor. These have the task of attacking everything that is foreign. They also detect individual hidden leukemia cells. This makes transplantation more successful than chemotherapy alone, which has no lasting effect once it has been eliminated from the body. The transplanted cells can survive for decades. Of course, this is no guarantee. Nevertheless, an allogeneic transplant, in which the donor and recipient are different people, is more effective.
Who is eligible to donate blood stem cells?
As this is an immunotherapy, the donor and recipient must ideally match 10 to 12 characteristics of the immune system. Otherwise the immune attack, reverse rejection reaction, can be fatal. First, let’s look at the siblings who have a 25 percent chance of matching. They must be healthy, willing to donate and no more than 70 years old. If no suitable siblings are available, the register is searched with almost 40 million entries.
Incidentally, there is an age limit of 18 to 40 years for new registrations in Switzerland. If no suitable donor is found in the registry, a maneuver is used to take half-matched siblings or children or frozen cells from umbilical cord blood. Young men are our favorite donors because their stem cells are the easiest to mobilize.
How does a donation work?
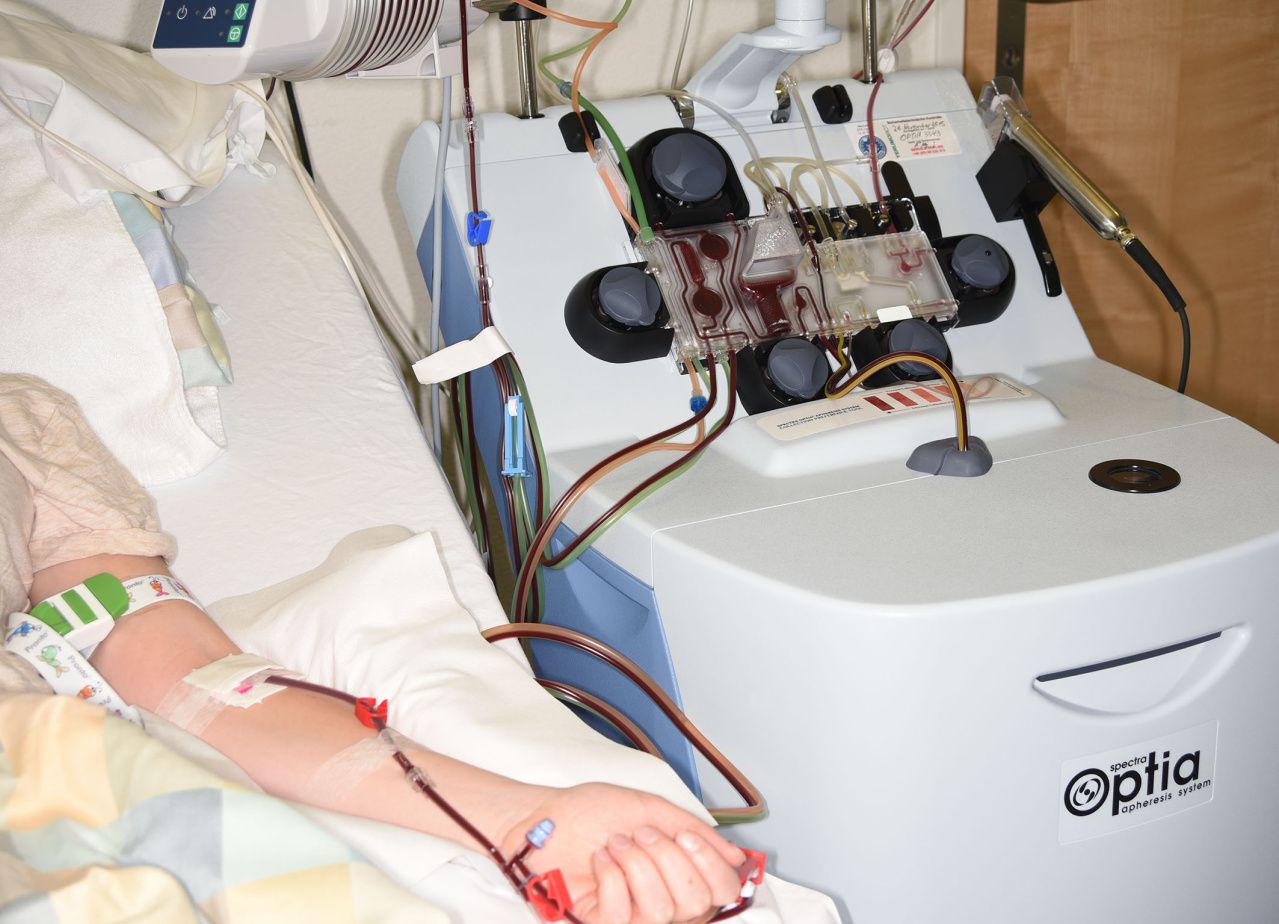
As a rule, we introduce the blood stem cells into the bloodstream using medication. To do this, the donor injects the growth factor into the fatty tissue of the leg. The stem cells multiply to such an extent that they spill over into the bloodstream. These are collected on day 5: On one arm, the blood flows into a machine with a centrifuge, which separates it into its components. The blood stem cells are aspirated and the rest is returned to the body via the other arm. This keeps blood loss to a minimum. Because blood formation is not normally noticeable, any bone pain that occurs can be treated well with paracetamol. A blood stem cell donation is therefore not such a big deal and reasonable!
How does a transplant work?
Leukemia patients remain in hospital for four to six weeks for the blood stem cell transplant. During the first seven days or so, high doses of chemotherapy and immunotherapy are administered to stop the patient’s own hematopoiesis and eliminate the immune barrier. The actual transplantation is carried out quite unspectacularly as an infusion. The stem cells find their way into the bone marrow on their own. Newly formed blood cells appear in the bloodstream between the 12th and 20th day. During this time, leukemia patients in special wards are protected from infections with air filters.
In order to prevent a reverse rejection reaction, transplant patients must take a number of medications in the first few months that suppress the immune system. A balancing act to prevent organ damage! It’s like driving a car with one foot on the gas and the other on the brake. For the first 100 days after the transplant, the person has to live as we all know it in coronavirus times: with a mask, without visitors and in complete isolation. In the best case scenario, the chances of recovery are 60 to 70 percent. But: people with leukemia only undergo this procedure with the goal of a cure in mind, which can also succeed.
Further information: