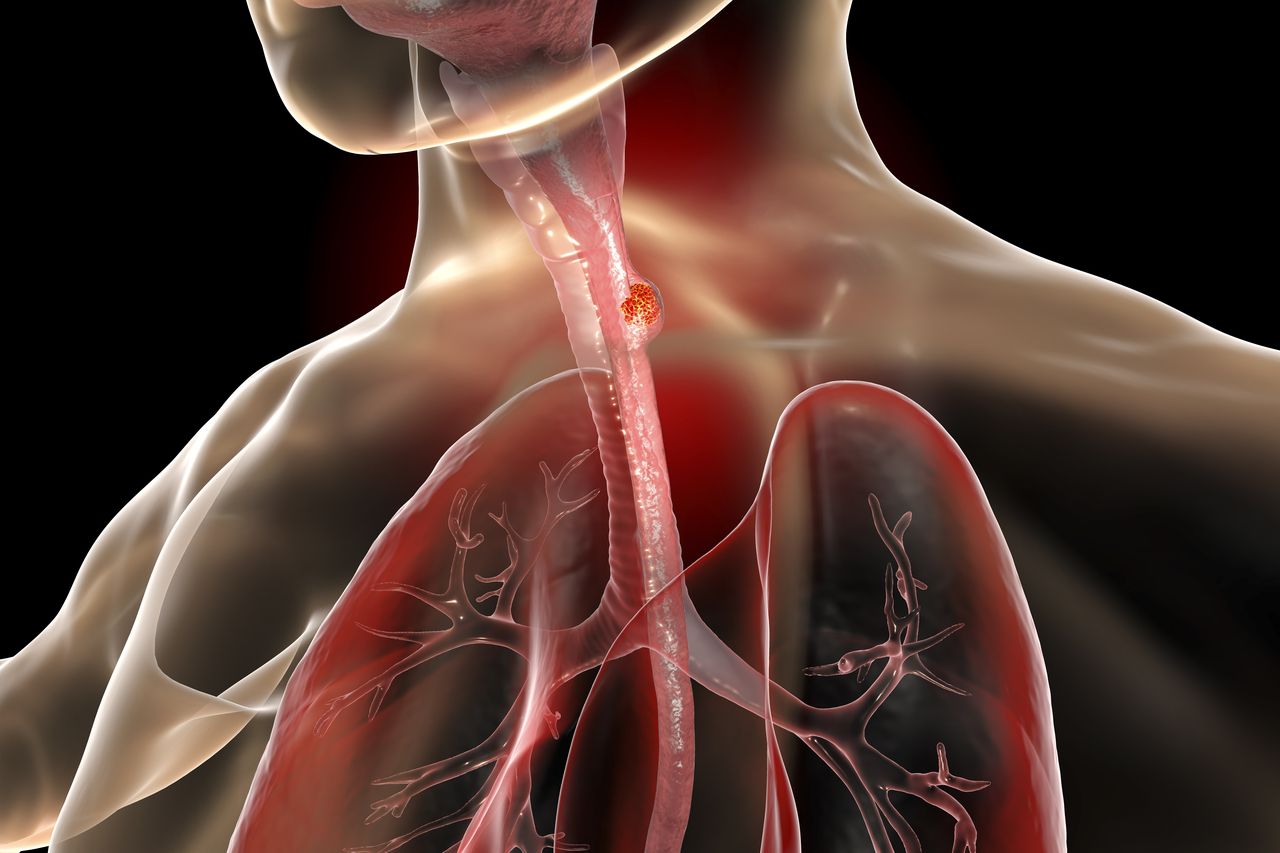
Esophagectomy can lead to life-threatening complications. A new procedure minimizes the risk, as a new accompanying clinical study at the USZ shows.
Every year, around 600 people in Switzerland are diagnosed with esophageal cancer. It is a particularly insidious cancer because it is usually only discovered late: Symptoms such as difficulty swallowing often only occur at an advanced stage. However, the later the diagnosis, the worse the chances of survival.
The most common treatment is surgical removal of the esophagus. If only parts of the esophagus are removed, this is referred to as an esophagectomy or resection. The stomach is then reshaped into a tubular replacement esophagus and connected to the remaining esophageal stump. The procedure is complicated because the esophagus behind the lungs is difficult to access. Thanks to minimally invasive techniques, morbidity has been massively reduced in recent years. Nevertheless, serious complications still occur relatively often after the procedure.
One of the most common reasons why an esophagectomy ends fatally is so-called anastomotic insufficiency. It occurs when the newly created connection between the residual esophagus and the stomach is leaky. If this is the case, endoluminal vacuum therapy has proven itself as a treatment. In this procedure, a sponge made of special plastic is inserted using endoscopy, after which the wound is effectively cleaned with the help of a vacuum pump.
However, this treatment can also be carried out prophylactically. “We have had very good experience with using vacuum therapy as a preventative measure,” says Professor Christian A. Gutschow, Head Physician at the Clinic for Visceral and Transplant Surgery at the USZ. This means that the sponge is placed in the area of the anastomosis during the operation and supplied with negative pressure. “This means that any undetected or emerging microleakages can be treated before they become clinically relevant,” says Gutschow.
An accompanying scientific study carried out at the USZ proves the success of the measure: instead of around 15 percent, insufficiency only occurred in around 5 to 7 percent of cases – which also reduced overall morbidity. According to Gutschow, the procedure is in principle suitable for every patient with esophageal cancer, but especially for high-risk patients. The USZ performs around 40 such procedures per year.
Progress also in aftercare
The USZ is also breaking new ground in the aftercare of esophageal cancer. “Many of the people treated suffer from the after-effects of the operation, which severely impairs their quality of life,” says Gutschow. However, non-oncological syndromes have so far been neglected. In their accompanying clinical research, Gutschow and his team have compiled the most common complaints of patients following esophageal surgery. These include difficulty swallowing, reflux, digestive problems, weight loss and diarrhea. “Only when we know what impairs quality of life can we target aftercare to the syndromes,” says Gutschow. This requires close cooperation between oncologists, radiologists, gastroenterologists and specialized nursing staff, as is the case at the USZ.