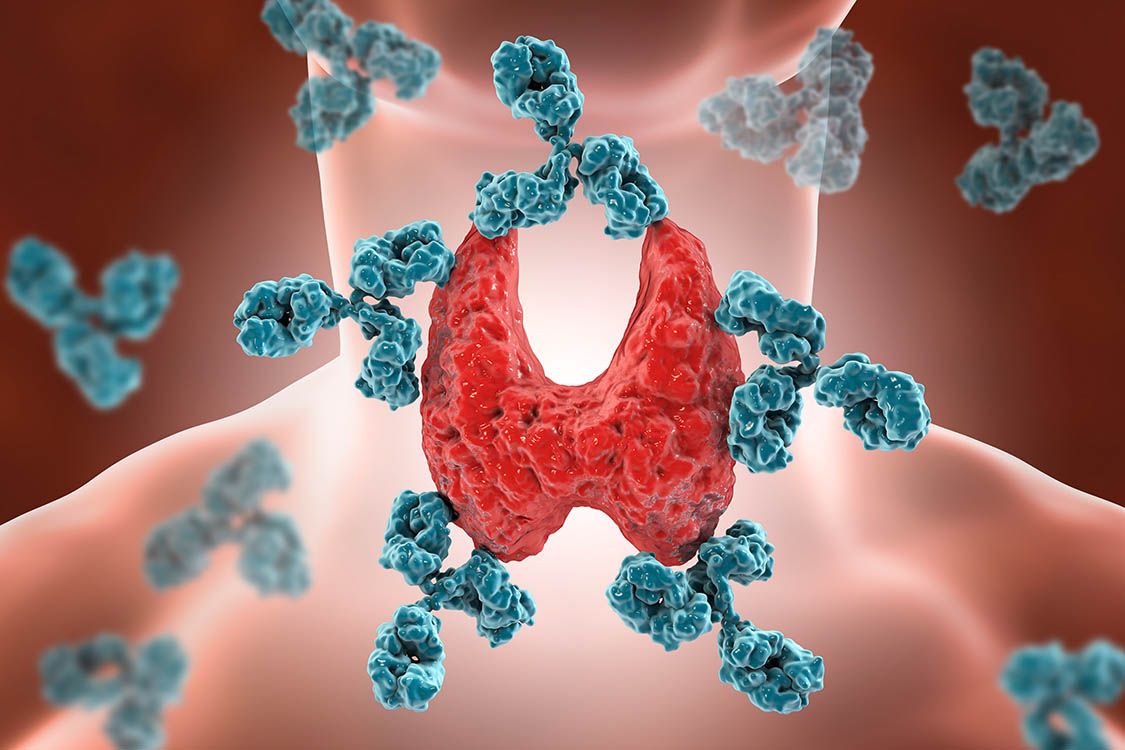
What is Hashimoto's thyroiditis?
This is an inflammatory reaction of the thyroid gland. The disease is also known as autoimmune thyroiditis or colloquially as Hashimoto’s and is named after the Japanese physician Hakaru Hashimoto, who first described it as an independent disease.
The body’s own defense system mistakenly targets thyroid cells. It is therefore an autoimmune disease in which the immune system attacks the body’s own tissue.
This persistent autoimmune reaction leads to the destruction of thyroid tissue over a period of years. The chronic inflammation therefore reduces the size of the thyroid gland over time, the organ works less and less and hypothyroidism develops.
This can have a whole range of negative consequences for the entire metabolism. Incidentally, the most common cause of hypothyroidism is autoimmune thyroiditis or Hashimoto’s thyroiditis.
Hashimoto’s frequency and risk groups
Hashimoto’s thyroiditis is the most common chronic disease of the thyroid gland and is estimated to affect up to 10% of the population in Central Europe. It is also one of the most common causes of hypothyroidism in Switzerland.
The disease often only occurs in adulthood, usually from the age of 30 and up to 50. Women are often affected; their risk of developing this form of thyroiditis is around 5:1 compared to men. The reasons for this are thought to include hormonal influences and gender-specific differences in the immune system.
In addition, many of those affected show a familial clustering, which indicates a genetic predisposition. People with Hashimoto’s thyroiditis also have an increased risk of developing other autoimmune diseases.
Causes and risk factors of Hashimoto's
Autoimmune thyroiditis or Hashimoto’s thyroiditis is an autoimmune disease that is directed against the thyroid gland.
Defense cells such as T lymphocytes attack the thyroid gland as if it did not belong to the body but to foreign tissue. Due to the involvement of T lymphocytes, this autoimmune disease is also known as chronic lymphocytic thyroiditis.
The exact causes of Hashimoto’s thyroiditis have not yet been conclusively clarified. Experts assume that a genetic predisposition interacts with additional triggering factors.
The triggers that misdirect our immune system and cause it to produce antibodies against thyroid tissue are still unknown. But there are assumptions:
- Familial predisposition: Genes could play a role, as autoimmune thyroiditis or Hashimoto’s thyroiditis occurs more frequently in some families. Some of those affected also have other autoimmune diseases, which confirms the theory of a family history. These include type 1 diabetes and celiac disease, but also rarer autoimmune diseases such as Addison’s disease (adrenal hypofunction), vitamin B12 deficiency anemia or pernicious anemia, but white spot disease (vitiligo) can also be present in parallel with autoimmune thyroiditis or Hashimoto’s thyroiditis. If at least two organs that are part of the hormone balance or two different glands are restricted in their function or no longer work, we speak of a polyglandular autoimmune syndrome, for example in type 1 diabetes and thyroiditis. The term polyglandular is made up of the Greek words “poly” for many and “glandula” for gland.
- Iodine-rich diet: In the case of a family history, a very high iodine intake could also be a risk factor for the development or worsening of an autoimmune thyroid disease. This applies in particular to high-dose iodine preparations or iodine-containing medication. The usual supply of iodine via the diet or iodized table salt, on the other hand, is not considered problematic.
- Infections: An infection with certain bacteria or viruses could trigger the familial predisposition to develop an autoimmune thyroid disease, so to speak. Such infections are not considered to be the sole cause, but are discussed as possible triggers if there is a genetic predisposition.
The significantly higher incidence of Hashimoto’s thyroiditis in women also suggests that hormonal influences could play a role in the development of the disease.
A genetic predisposition plus an infection could therefore be the cause of this autoimmune thyroid disease, it is assumed, but this has not been proven.
Initially sometimes like hyperthyroidism, later typical of hypothyroidism
Autoimmune thyroiditis or Hashimoto’s thyroiditis often remains undetected for a long time because there are virtually no early symptoms. The chronic disease progresses slowly. Mild hyperthyroidism can sometimes occur in the early stages as a response to the inflammation. The following symptoms then appear, which are typical of hyperthyroidism:
- You sweat more than before.
- Although you are not eating less than usual, you are losing weight.
- You are nervous.
- You are constantly suffering from palpitations.
This phase is usually temporary and is often not clearly attributed to thyroid disease by those affected.
As autoimmune thyroiditis progresses, thyroid tissue is destroyed and the production of thyroid hormones decreases. This results in the specific symptoms of an underactive thyroid (hypothyroidism), such as
- The drive is missing.
- They gain weight and tend to become constipated.
- This leads to concentration problems.
- You are constantly tired, even though you sleep more than you used to.
- They shiver quickly and are particularly sensitive to the cold.
- The skin becomes dry.
- The hair also changes and becomes brittle.
In addition, hypothyroidism can lead to psychological and cognitive symptoms, such as depressive mood, irritability, inner tension or memory and word-finding disorders (“brain fog”). The severity of the symptoms varies greatly from person to person and not all symptoms occur at the same time in every affected person. In women, cycle changes or an unfulfilled desire to have children can also be the first signs of thyroid dysfunction.
In the course of the disease, structural changes to the thyroid gland can also occur. This can cause the organ to shrink (atrophy of the thyroid gland), but sometimes it can also enlarge. The enlargement of the thyroid gland is often perceived by those affected as an additional symptom, as a so-called globus sensation in the throat. They describe it as if a lump is pressing in the throat and narrowing the pharynx a little.
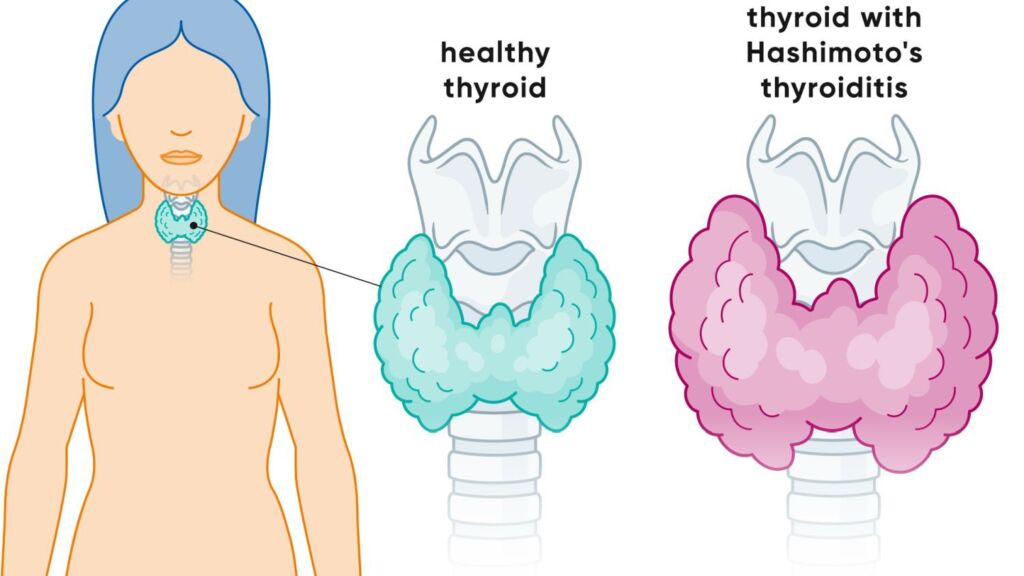
Hashimoto's thyroiditis diagnosis
Because the symptoms only become clearer gradually, most sufferers do not seek medical advice until it is too late. Thyroid inflammation is therefore often only diagnosed when the organ is already noticeably damaged and its function is restricted.
Various methods are used to detect thyroid inflammation or Hashimoto’s thyroiditis:
- Palpation examination: During the palpation examination, we check whether the thyroid gland is enlarged or reduced in size and whether it is sensitive to pressure. Palpation can therefore already provide initial clues.
- Blood test: The blood test is more informative if autoimmune thyroiditis or Hashimoto’s thyroiditis is suspected. These include various blood values that are associated with the thyroid gland. On the one hand, this involves a targeted search for specific antibodies that occur in autoimmune thyroiditis. They indicate whether this disease is present, but not whether thyroid function is also affected. This is why thyroid levels are also checked, as they show whether and to what extent the chronic inflammation is already affecting thyroid function. Together, these values provide information on whether Hashimoto’s thyroiditis is present and to what extent it results in a thyroid dysfunction that requires treatment. A typical example of the detection of Hashimoto’s disease and the associated hypothyroidism: TSH and TPO-AK values are elevated, T4 values are too low.
- Ultrasound examination: Finally, the ultrasound examination provides additional information on whether the thyroid gland is altered by inflammation. In addition, further examinations can be carried out, such as fine needle biopsy for tissue sampling and thyroid scintigraphy as an imaging diagnostic option.
- Scintigraphy: A thyroid scintigraphy can also be used to obtain information about the function of the thyroid gland.
As a rule, the diagnosis is based on a combination of clinical findings, blood values and imaging examinations. Blood values play a central role in the diagnosis and in the further course of the disease. They allow conclusions to be drawn about both thyroid function and the presence of an autoimmune reaction.
Hashimoto’s thyroiditis values
The blood values not only help with the diagnosis, but are also crucial for monitoring the course of the disease and planning treatment. It is important to understand that it is not a single value that is assessed, but always the interaction of several parameters.
The TSH value serves as a central orientation value and indicates how strongly the thyroid gland is controlled by the superordinate hormone system. In addition, the thyroid hormones free T4 (fT4) and free T3 (fT3) provide information about the actual hormone production of the thyroid gland.
Antibodies against thyroid tissue, especially TPO antibodies, are typical for the detection of autoimmune diseases. Elevated antibody levels confirm an autoimmune reaction, but do not allow a direct statement about the severity of the disease or the current need for treatment.
Blood values are therefore always assessed in conjunction with the symptoms and other findings. Symptoms may be present even if the values are normal, while conversely, elevated antibodies do not necessarily require immediate treatment.
Differential diagnoses for Hashimoto’s
The symptoms of Hashimoto’s thyroiditis are sometimes non-specific and can also occur with other diseases. It is therefore important to specifically rule out other possible causes.
These include in particular other thyroid diseases, such as hyperthyroidism of a different cause, subacute thyroiditis or nodular changes in the thyroid gland.
Deficiencies such as iron, vitamin B12 or vitamin D deficiency and mental illnesses, such as depressive disorders or fatigue syndrome, can also cause similar symptoms.
A careful medical assessment helps to correctly classify the symptoms and initiate targeted treatment.
Everyday life with Hashimoto's thyroiditis
After diagnosis, many sufferers are faced with the question of what Hashimoto’s thyroiditis means for their everyday life in the long term. The disease is usually chronic and accompanies those affected for many years.
However, with individually adapted treatment and regular medical check-ups, thyroid function can usually be well balanced. In most cases, therefore, no significant reduction in quality of life is to be expected in everyday life.
In addition to drug therapy, lifestyle and diet also play a role in personal well-being and stable thyroid function. A good understanding of the disease can help those affected to recognize changes at an early stage and actively support treatment.
Diet and lifestyle for Hashimoto’s
A special diet for the treatment of Hashimoto’s thyroiditis is not necessary. In principle, the same recommendations apply as for a healthy general population: a balanced, varied diet, regular exercise and sufficient rest.
However, individual nutrients play a role in thyroid function. These include iodine, selenium, iron, vitamin B12 and vitamin D in particular. While a normal intake of iodine through the diet is generally unproblematic, high-dose iodine supplements should be avoided without consulting a doctor.
Dietary supplements are not routinely necessary for Hashimoto’s thyroiditis and should only be used if a deficiency is proven. There is also no general recommendation for special diets, such as gluten-free or anti-inflammatory diets.
A healthy lifestyle with regular exercise, sufficient sleep and stress reduction can help to improve general well-being and better manage symptoms. The decisive factor is an individually tailored therapy and good medical support.
Special phases of life: Desire to have children and pregnancy
Thyroid function is particularly important if you want to have children and during pregnancy. Thyroid hormones are important for the development of the unborn child, especially in the first weeks of pregnancy.
Women with Hashimoto’s thyroiditis should therefore have their thyroid levels checked as soon as they wish to have children. Regular checks are necessary during pregnancy, as the need for thyroid hormones can change and medication often needs to be adjusted.
If the thyroid function is well adjusted, pregnancy is usually uncomplicated. Close cooperation between the attending physician and the pregnant woman helps to minimize risks for mother and child.
Follow-up checks are also useful after the birth, as thyroid function can change again in the postpartum phase.
Hashimoto's disease: prevention, early detection, prognosis
Targeted prevention of Hashimoto’s thyroiditis is not possible. Because the causes of this chronic thyroid disease are not known, there are no reasonable starting points in this context.
Therefore, do not fail to recognize the disease at least as early as possible. Always have the symptoms listed checked by a doctor. The simple blood test checks the most important thyroid parameters safely and quickly.
Progression and prognosis for Hashimoto’s
There is no way to cure Hashimoto’s thyroiditis. The chronic inflammation progresses and gradually destroys thyroid tissue. This results in hypothyroidism. However, this can be compensated for with appropriate tablets.
Autoimmune thyroiditis only becomes dangerous if this therapy is not carried out. However, if the thyroid dysfunction is treated and specifically compensated for, those affected can live normally and are considered healthy.
Self-help groups
The exchange with people who are affected by the same disease can be a great support in coping with the disease. Advice on finding a suitable self-help group is available from Selbsthilfe Zürich. Self-Help Zurich and the University Hospital Zurich are cooperation partners in the national project “Health literacy thanks to self-help-friendly hospitals”.
Hashimoto's thyroiditis: treatment with thyroid hormones
Hashimoto’s thyroiditis does not always need to be treated. Even if antibodies are detectable in the blood, medication is not necessary as long as thyroid function is normal and there are no symptoms. In these cases, regular checks of thyroid levels are sufficient to detect changes at an early stage.
Hashimoto’s is not treated for the inflammation itself, but for its consequences. As the disease progresses, the thyroid gland can produce fewer and fewer hormones. If this leads to an underactive thyroid (hypothyroidism), treatment is usually necessary.
The therapy consists of taking thyroid hormones, usually in the form of levothyroxine (L-thyroxine). This medication replaces the missing hormone and compensates for the hypofunction. The required dose is determined individually and adjusted based on the blood values.
Regular medical check-ups are necessary to achieve a good setting. As thyroid function can continue to change over time, the dosage must be adjusted occasionally. In most cases, treatment is required on a long-term or lifelong basis. In this phase, annual checks are usually sufficient.
With well-adjusted therapy, those affected can lead a normal life without any relevant restrictions.
Frequently asked questions about Hashimoto's disease
Hashimoto’s thyroiditis often progresses gradually. Initially there are often no or only unspecific symptoms. As the condition progresses, symptoms of hypothyroidism such as tiredness, weight gain, sensitivity to cold or concentration problems usually occur.
Hashimoto’s is typically a chronic, usually painless inflammation of the thyroid gland caused by an autoimmune reaction. Elevated thyroid antibodies and a slow loss of thyroid function are characteristic.
The exact causes have not been conclusively clarified. It is assumed that there is a genetic predisposition and that additional factors such as infections or hormonal influences can trigger the disease.
Hashimoto’s specifically targets the thyroid gland. The immune system attacks thyroid cells, which leads to chronic inflammation and reduced hormone production in the long term.
Hashimoto’s is an autoimmune disease, while hypothyroidism is a functional disorder. Hashimoto’s is the most common cause of hypothyroidism, but not all hypothyroidism is caused by Hashimoto’s.
With early diagnosis and correct treatment, life expectancy is not limited. With well-controlled thyroid function, those affected can lead a normal life.
The condition varies greatly from person to person. Many sufferers feel symptom-free with a good adjustment, others report tiredness, exhaustion or concentration problems, especially if the therapy has not yet been optimally adjusted.
There are no generally prohibited foods for Hashimoto’s. High-dose iodine preparations should be avoided without consulting a doctor. A balanced diet is recommended; special diets are not usually necessary.
A so-called flare-up can become noticeable through a temporary worsening of symptoms, such as increased tiredness, restlessness or changes in thyroid levels. However, not every change in mood means a surge in disease activity.
An increasingly bulging or bloated abdomen can have various causes. An untreated hypothyroidism can contribute to a slower metabolism, which can lead to weight gain, water retention or constipation. Digestive problems or accompanying intolerances can also play a role. However, a big belly is not a specific feature of Hashimoto’s.
Hashimoto’s thyroiditis is not usually acutely dangerous. If left untreated, however, it can lead to severe hypothyroidism. With regular monitoring and treatment, complications are easily avoidable.