Malignant diseases
The majority of our patients suffer from tumor diseases. A malignant tumor disease is also called “cancer”. Malignant tumors are characterized by aggressive growth and the possibility of metastasis. The growth of tumors can be stopped by radiotherapy and in many tumors all diseased cells can be killed by radiation.
In principle, radiation affects healthy and diseased tissue in equal measure: The cells are damaged. However, healthy cells are better able to repair the damage than diseased cells. Tumor cells are therefore more severely affected.
By concentrating the radiation in the diseased area, this is particularly damaged and the surrounding healthy tissue is spared as much as possible.
Benign diseases
Benign tumours are characterized by slow, displacing growth and are usually treated surgically. But here too, radiotherapy can play a decisive role due to its lower burden on the patient and achieve results that are often on a par with surgery. Radiation oncologists and surgeons decide together which therapy is the best choice for the individual patient.
Benign functional diseases
Functional clinical pictures are usually understood to be persistent, inflammatory processes. The most common include inflammation of the tendons or their attachments, tendon thickening, inflammation of the joints due to underlying osteoarthritis and others. Good results have been achieved with heel spurs or tennis elbow, for example: in the majority of patients, pain relief or even complete freedom from pain can be achieved.
Procedure
As a specialist field, radio-oncology deals with the therapeutic use of X-rays. In most cases, treatment is carried out with curative intent in the case of cancer. Radiation can be carried out alone or in combination with other therapies.
Radiotherapy before surgery can shrink tumors and make them easier to remove. After surgical interventions, any remaining tumor cells can be destroyed, thus preventing recurrence.
Radiation treatment can also be combined with chemotherapy to further damage the tumor cells.
Procedure for radio-oncological treatment
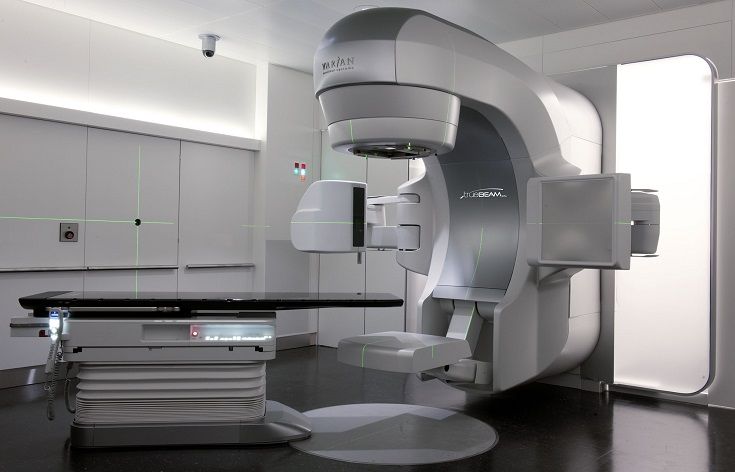
TrueBeam linear accelerator in the Department of Radio-Oncology, University Hospital Zurich
Even if a cure is no longer possible, symptom-relieving (=palliative) radiotherapy can bring great relief. Radiation is one of the most effective treatments for tumor-related pain. If tumors press on nerves or organs, pain or paralysis are frequent consequences. If tumors or their metastases grow in the brain, this can lead to seizures, headaches or mental deficits. Radiation is used to shrink or completely kill the tumors so that the pain and other symptoms disappear or are at least alleviated. Tumor bleeding can also be stopped by radiation.
Side effects of radiotherapy
Side effects of radiotherapy occur when healthy cells are also damaged by the radiation or when diseased cells die and are broken down by the body. In order to minimize the undesirable effects as much as possible, we plan the targeted irradiation of the diseased area with the best possible protection of the surrounding healthy tissue.
You will be seen and examined regularly by your treating doctor throughout your therapy. Close monitoring allows us to get an idea of the success and side effects of the therapy in order to optimize it. Please do not hesitate to let us know if you have any complaints or questions.
There are different side effects depending on where you are irradiated.
General side effects
Your illness, but also the radiotherapy, is exhausting for your body. Many patients report increased tiredness and fatigue during therapy. This generally improves within a few weeks of completing therapy.
A healthy and balanced diet and physical activity, even during radiation treatment, help to minimize these side effects. General symptoms such as nausea may also occur. Irradiation in the abdominal cavity or in the brain shows an increased risk of this.
Nutrition & digestion
Radiation treatments can cause certain digestive problems such as diarrhea, constipation and difficulty swallowing. Symptoms such as nausea and vomiting can also occur in connection with inflammation of the gastrointestinal tract or as a result of irritation of the vomiting center in the brain. The symptoms are usually temporary and subside after the treatment is completed. Some of these symptoms can be completely eliminated or at least alleviated by medication, others by adjusting or changing the diet.
A healthy, balanced diet provides the body with vital nutrients and strengthens the organism, which has been stressed by the illness and radiation. Tasty, appetizing meals increase the desire to eat. To relieve the gastrointestinal tract as much as possible, you should eat small meals more often (every two to three hours), chew your food thoroughly and drink as much as possible.
It is sensible to reduce alcohol and especially nicotine consumption as much as possible or to give it up completely. Alcohol irritates the mucous membranes and can increase side effects; nicotine damages the mucous membranes and reduces the chances of recovery. Medication can also irritate the stomach lining. They should always be taken with sufficient liquid and – unless otherwise prescribed – not on an empty stomach. Sometimes there are changes in taste sensation, loss of appetite and weight loss. In rare cases, indirect consequences of radiation can also include hunger attacks and weight gain. If you have lost a lot of weight, it may be useful to supplement your diet with additional carbohydrates, vitamins and proteins. Your dietician can recommend concentrated ready-to-drink products that contain all the important nutrients as a drinking solution and are available in different flavors.
If normal nutrition is not sufficient or is not possible by oral means (through the mouth), artificial nutrition can provide relief. Gastric or intestinal tubes (enteral feeding) are less uncomfortable today than they used to be and can also be used at home. We advise against so-called cancer diets. Not only are they ineffective, one-sided and monotonous, they also weaken the body. The effects of the treatment continue after the radiotherapy has been completed. You should therefore stick to the dietary recommendations for another two to three weeks and only then slowly return to your usual diet. If you have any questions or problems relating to nutrition, please contact your doctor or the nutritionist at your hospital. They will answer your questions and create a nutrition plan tailored to your personal needs and preferences. You can find more tips and suggestions in the Cancer League brochure “Nutritional problems in cancer”.
Skin & Hair
Nowadays, skin and hair are better protected from radiation than in the past. Nevertheless, localized, mild, sunburn-like skin reactions may occur in the radiation field. These can be mitigated by observing the following points in the irradiated areas:
Avoid any additional skin irritation (intense sun, hot water bottles, ice packs, tight-fitting clothing, cosmetics, etc.)
- Leave the skin uncovered as often as possible (but protect it from direct and intense sunlight)
- Do not scratch if itching
- Wash with clear water without soap, do not wash off the markings
- Prefer a lukewarm shower to a full bath
- Dry the skin with a soft cloth or cold hairdryer, preferably dabbing instead of towel drying
- Electric shaving irritates the skin less than wet shaving
- Cotton/silk garments are more skin-friendly than those made from synthetic fabrics
If there is hair loss in the irradiated area, it usually starts to grow again 2-3 weeks after the end of treatment. Hair loss can be concealed with head scarves, hats or wigs.
Tumor induction
Radiation also damages the genetic material of healthy cells. These can usually repair themselves or die off. In very rare cases, radiation therapy can cause a tumor to develop in the radiation field at the earliest 10 – 20 years after radiation. The frequency of such tumor induction strongly depends on the patient’s age at the time of irradiation and the irradiated region. Your doctor will inform you about your individual risk. With all radiation treatments, however, the possible success of the treatment is to be considered more important than the usually rare side effect of tumor induction.
Abdomen
If the abdomen is irradiated, temporary irritation of the urinary tract and pain when urinating may occur. Irritation of the rectum, large intestine and (more rarely) small intestine is also possible. Because radiotherapy and chemotherapy are often used together for cancer in the pelvic area, bloating, cramps and diarrhea can occur. Please consult your doctor as soon as you notice the first symptoms.
Radiation used for certain types of cancer can lead to the absence of menstruation. Radiation can also affect sexuality. Inflamed mucous membranes cause pain during sexual intercourse. Feelings of discomfort during radiotherapy are also not unusual for women and men. Whether and to what extent they occur varies greatly from person to person and cannot be predicted. Take your time – it’s quite normal not to feel like it. It is important to know: Cancer is not a contagious disease that can be transmitted during sexual intercourse. However, it can lead to physical limitations and psychological disorders. The understanding and sensitivity of your partner and talking to them are now particularly important. If you have not yet completed your family planning, you should definitely discuss this with your doctor before starting radiotherapy.
Technology & types of radiation in radio-oncology
There are different types of radiation that are used in radio-oncology. The radiation can be produced by the decay of radioactive elements. For medical purposes, however, it is generated using particle accelerators.
Photons
The most commonly used radiation is high-energy electromagnetic radiation. It can occur during the decay of radioactive elements or be generated using an electron accelerator. It is then also referred to as ultra-hard X-ray bremsstrahlung.
Electrons (beta radiation)
Electron radiation, which does not penetrate far into the tissue, can therefore be used particularly well for superficial tumors.
The choice of the type of radiation, the energy of the radiation and the technique used depends on the type, location and extent of the tumor. In addition to different types of rays, there are different techniques for using them. A distinction can be made between percutaneous radiotherapy (from the outside, through the skin) and brachytherapy (Greek brachys = short).
Percutaneous irradiation
Percutaneous radiotherapy is the most common radiotherapy technique. The tumor located in the body is precisely targeted from the outside using radiation. The radiation is artificially generated by a linear accelerator. The linear accelerator has no radioactive source. This means that it does not emit any radiation when it is not switched on. The radiation is generated by accelerating electrons in an acceleration tube to the desired energy.
When irradiated with photons, the electrons are directed onto a metal plate (target), where photons are generated in a physical reaction. The radiation (photons or electrons) is then directed at the patient’s tumor and applied.
Our linear accelerators generate photons with energies of 6 and 18 MV and electrons with energies of 6, 9, 12, 16 and 20 MeV. Photons and electrons have different beam characteristics and are used depending on the location of the tumor. Irradiation is subject to the highest safety requirements, which is why our linear accelerators are tested daily. In addition, a whole series of safety thresholds (interlocks) ensure that the patient is irradiated correctly. To ensure the safety of patients and staff, downtime for servicing, repairs and major checks must be accepted.
IMRT & VMAT
IMRT stands for “Intensity Modulated Radiotherapy”. In normal percutaneous therapy, the beam fields are limited by the diaphragms, the Multi Leaf Collimators (MLC). The radiation is homogeneous within these limits. However, the human body is not homogeneous. It consists of body parts of different densities (e.g. bones and lungs) that absorb more or less dose. Furthermore, the entrance surface of the radiation is not always flat, so that the penetration depth for the radiation can vary within an irradiation field. This means that you want to deliver more or less radiation to defined parts of a field in order to obtain a homogeneous dose distribution in the target volume. This is exactly what is possible with IMRT. Put simply, the radiation field is divided into small segments. The planning system calculates how many monitor units must be delivered in each segment in order to obtain the prescribed dose in the target volume.
Traditionally, radiation fields were applied from 5-7 different directions. Nowadays it is possible to irradiate from all directions to varying degrees while moving the irradiation device. This standard technique called VMAT (Volume Intensity Modulated Arc Therapy) or Rapid Arc shortens the treatment time and enables a better dose distribution.
Stereotaxy
With the Stereotactic Center, we can build on a wealth of expertise and experience in this field. Stereotactic radiotherapy is the extremely precise irradiation of small volumes with high doses in one (radiosurgery) or only a few sessions (fractionated stereotactic radiotherapy).
Precise patient positioning is a prerequisite for small-volume irradiation with a small safety distance around the target volume. This enables the most precise delivery of the dose in the target volume while at the same time protecting the surrounding tissue as much as possible.
Proton therapy
Treatment with fast proton particles is even more gentle on the tissue around the tumor in certain tumor types than state-of-the-art photon therapy. For some, but not all patients, proton therapy can therefore be an advantage compared to conventional radiation with high-energy X-rays. Predestined for this are childhood brain tumors, eye tumors and rare tumors of the base of the skull or the spine. We work closely with the Paul Scherrer Institute (PSI) to enable our patients to undergo such state-of-the-art therapy.
PSI has been a world leader in the technical and clinical research and application of proton therapy for many years.
Thanks to the close links between the Department of Radiation Oncology at the USZ and the PSI, our patients have fast and direct access to this modern form of radiotherapy.
Whole body irradiation
This is an irradiation method prior to a bone marrow transplant. As the name suggests, the whole body is irradiated during whole-body irradiation.
This form of radiation is used in particular for malignant diseases of the blood and lymph glands, always in combination with intensive chemotherapy.
Brachytherapy
In brachytherapy, a radioactive source is placed directly in or near a tumor. Due to the close proximity to the tumor, the law of distance squared and/or the short range of the radiation can be exploited. The underlying healthy tissue is largely spared. For the treatment we use gamma rays coming from an Iridium-192 source.
The most common form of brachytherapy is intracavitary and interstitial therapy. Here, the radiation source is placed in naturally existing body orifices or via hollow needles in soft tissue in order to irradiate the tumors located there. We use a high dose rate afterloading device in which the radioactive source is stored in a shielded container. Once the application has been placed, the positioning accuracy ensured, the irradiation planned and the dwell time of the radioactive source calculated, the radioactive source is brought into the irradiation position under computer control. The afterloading technique enables the greatest possible protection of the patient and staff. You can find more information on brachytherapy here.
Radiotherapy 4D-CT
To ensure that the radiation treatment is as precise as possible, we use special positioning systems as well as the latest technologies for treatment planning, such as 4D CT. A 4D CT not only shows the position of the bones and internal organs, but also their movement. In addition to the three-dimensional spatial resolution (3D), it also includes a temporal component. In this way, consideration can also be given to unavoidable movements during irradiation, such as breathing. The 4D CT shown below is an example of the movement of a tumor in the lung.
Equipment and technology
