Overview
White skin cancer is still on the rise in Switzerland. The number of cases has tripled in the last 30 years – to around 30,000 per year today. Skin cancer is most commonly operated on as an outpatient procedure under local anesthesia. The main alternative is radiation. Large tumors sometimes require more complex therapy.
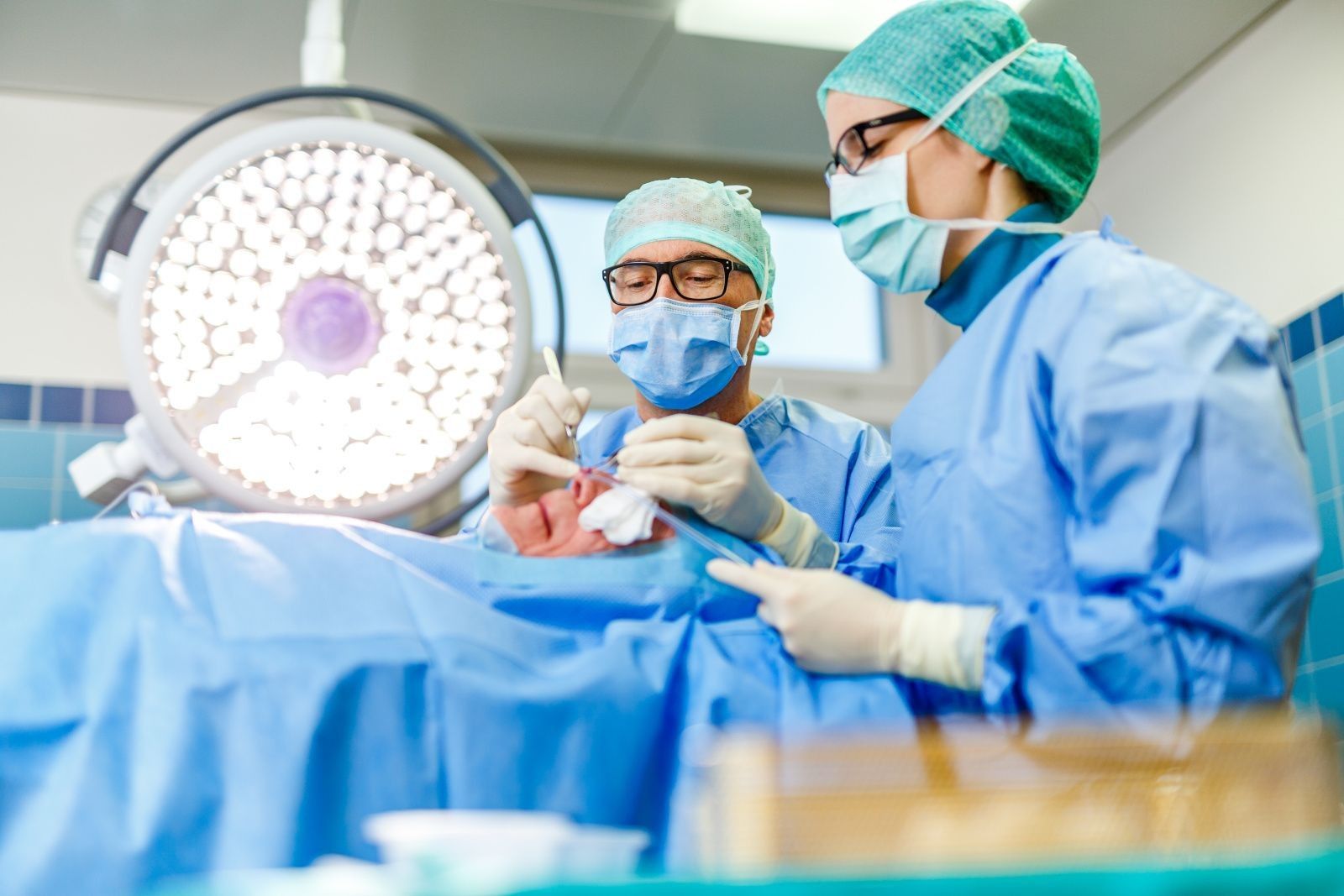
During surgery, it is extremely important to remove the entire skin cancer, as otherwise the tumor can quickly recur. However, this is not so easy because skin tumors have the property of growing with fine extensions that are not visible from the outside. To be on the safe side, the tissue is therefore often cut out with a large safety margin – which leaves traces in the form of unnecessarily large scars. As skin cancer mainly occurs in sun-exposed areas such as the face, neck or arms, many sufferers find such scars unsightly.
In such cases, Mohs surgery can be a worthwhile alternative. The tumor is cut out at a relatively close distance, after which the piece of tissue at the edges of the cut is examined microscopically. If tumor remnants are found, another operation is performed at this site. These steps are repeated until no more tumor remnants are found. This procedure has two decisive advantages: Firstly, there are far fewer relapses: instead of around 5 to 25 percent of patients (depending on the type of tumor), only 1 to 5 percent have to be operated on again later due to a relapse. Secondly, the aesthetic result is better, as only as much tissue is removed as necessary.








