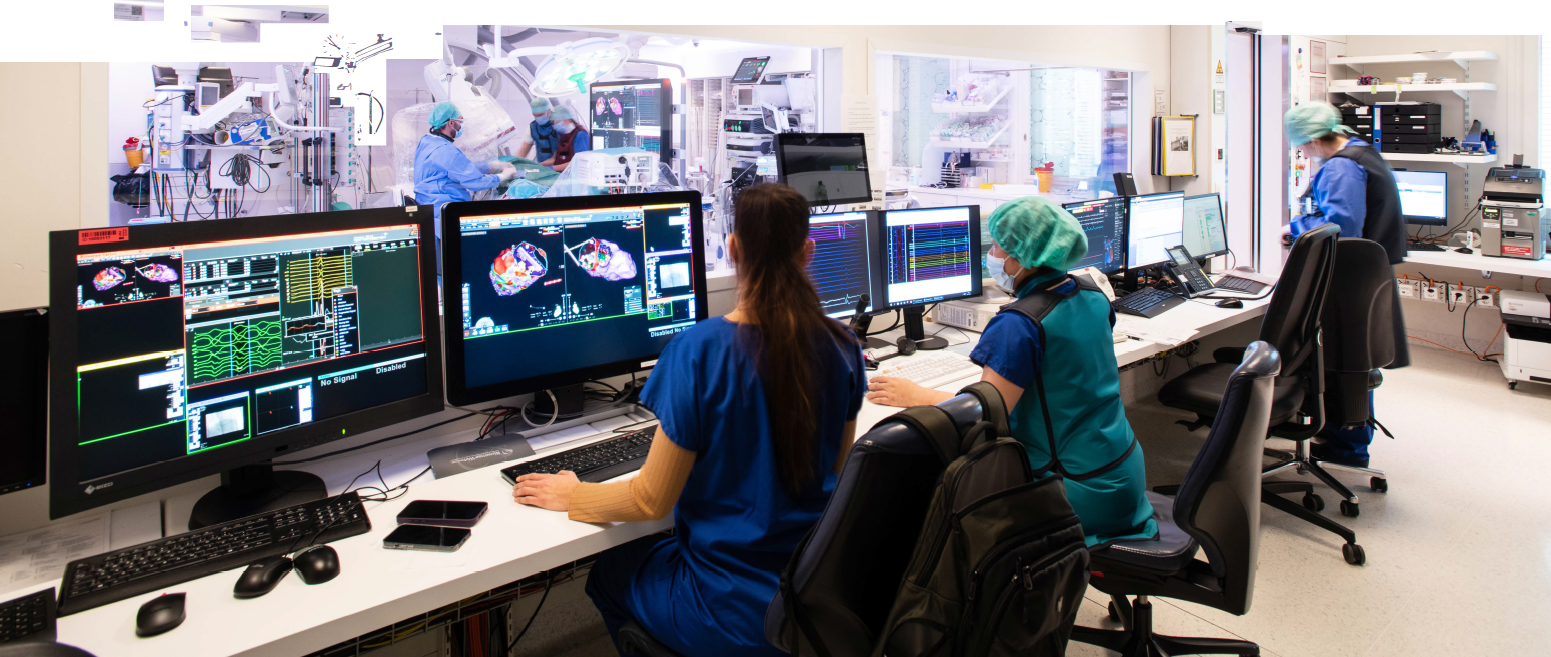
During an electrophysiological examination (EPS), catheters are placed at various points in the heart. This allows the electrical properties of the heart to be determined. Cardiac arrhythmias can be triggered, terminated and localized. The aim of an EPS is to identify and localize the patient’s arrhythmia so that it can be treated in the next step. In addition to medication, treatment options include ablation, i.e. obliteration of the respective arrhythmia using heat (radio frequency) or cold energy (cryoablation).
Latest technology
Pulsed Field Ablation (PFA) is a new technology for the treatment of cardiac arrhythmias, especially atrial fibrillation. This form of energy is very specific to the heart muscle tissue and can therefore spare surrounding structures during ablation. Paralysis of the phrenic nerve is the most common complication of cryoenergy-based ablation of atrial fibrillation (cryoballoon). This complication practically does not occur with PFA due to its more selective effect on the myocardium. Atrioesophageal fistula is a dreaded, fortunately very rare complication of radiofrequency energy-based ablation of atrial fibrillation, and is often fatal. This complication can also be practically eliminated by using PFA, as the heart muscle is selectively ablated and the esophagus is spared. Other complications such as severe narrowing of the pulmonary veins have also not been described with PFA. Several international studies have shown that pulmonary vein isolation with PFA is at least as effective as previously used technologies (cryoballoon and radiofrequency). At the University Hospital, we will be one of the first centers worldwide to use this new effective and safe technology for the treatment of cardiac arrhythmias, especially atrial fibrillation, and hope to be able to treat our patients with arrhythmias even more safely and effectively.