What is coeliac disease?
Celiac disease is an autoimmune disease of the small intestine and not a food allergy. It is caused by an intolerance to gluten in the small intestine. Gluten is a gluten protein that is mainly found in cereal products made from wheat, rye, oats, barley and spelt. Ancient grains such as einkorn, kamut and emmer also contain gluten and are not gluten-free.
Gluten is harmless for healthy people, but it is problematic for people with coeliac disease, as their bodies react to this gluten protein with inflammation. If they consume gluten despite this intolerance, it triggers an overreaction of the immune system. The body produces antibodies as in a viral or bacterial infection. These antibodies attack the intestinal villi in the small intestine and destroy them.
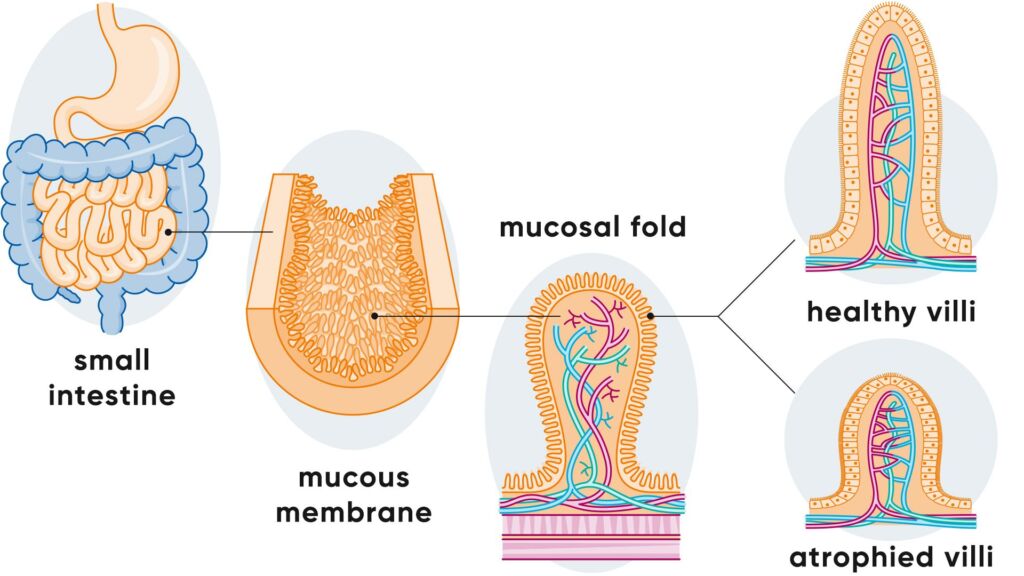
In coeliac disease, the consumption of gluten triggers inflammation of the mucous membrane of the small intestine. This causes the villi of the small intestine to die off over time.
Consequences of coeliac disease
Coeliac disease leads to chronic inflammation of the intestinal mucosa, which in turn leads to a reduction in the surface area of the small intestine, known as villous atrophy. This has far-reaching consequences, as the small intestine is the most important organ for digestion and nutrient absorption. Here the food components are broken down with the help of digestive enzymes so that they can be absorbed into the blood via the finger-shaped villi of the small intestine. If these villi atrophy due to inflammation, the intestine can no longer adequately absorb nutrients from food.
Untreated coeliac disease can lead to deficiency symptoms, including iron, folic acid, calcium and zinc deficiency as well as a deficiency of the fat-soluble vitamins A, D, E and K. The damaged intestinal mucosa often leads to lactose intolerance (lactose intolerance) in coeliac disease.
Coeliac disease can occur at any age, but mostly in children and young adults between the ages of 25 and 40. Women are affected about three times more often than men. If the disease remains untreated, it can damage the body in the long term. Why some people develop coeliac disease and others do not is not yet fully understood.
Forms of coeliac disease
There are various forms of coeliac disease, which differ in their symptoms and course:
- Classic coeliac disease: The most common form, with typical symptoms such as diarrhea, weight loss, abdominal pain and flatulence. This form is often diagnosed in young children.
- Atypical coeliac disease: This form has less obvious symptoms, such as abdominal discomfort or digestive problems. Instead, symptoms such as tiredness, skin problems or joint pain may be in the foreground.
- Silent coeliac disease (silent): No obvious symptoms are recognizable here, but there is damage to the mucous membrane of the small intestine. This form is often only discovered through blood tests or an intestinal biopsy.
- Latent coeliac disease: People with this form of gluten intolerance have no current symptoms or intestinal damage, but are genetically predisposed. The disease can become active later, especially with a gluten-containing diet.
- Refractory coeliac disease: A rare and severe form in which the symptoms persist despite a strict gluten-free diet and the intestine does not heal. This form can cause serious complications and requires specialized treatment.
Coeliac disease: causes and risk factors at a glance
The causes of coeliac disease are complex and multifactorial. They include genetic, immunological and environmental factors:
Genetic predisposition to coeliac disease
The main cause of coeliac disease is a genetic predisposition. Around 95% of people with coeliac disease carry the HLA-DQ2 or HLA-DQ8 genes. These genes are associated with the development of the disease and determine how the body reacts to gluten. However, the presence of these genes does not automatically mean that a person has coeliac disease. Almost a third of the population carries these genes, but only a small proportion actually develop the disease. This indicates that other triggers are necessary in addition to genetic factors.
Immune reaction to gluten
In people with coeliac disease, the immune system reacts to gluten as if it were recognizing a threat such as a virus or bacterial infection. This misdirected immune reaction leads to the formation of antibodies that not only attack the gluten, but also damage the mucous membrane of the small intestine, especially the intestinal villi. This inflammation impairs the intestine’s ability to absorb nutrients from food.
Environmental factors increase the risk of coeliac disease
It is assumed that environmental factors play a role in whether a person with a genetic predisposition actually develops coeliac disease. These include, for example
- Early childhood diet: Studies suggest that the timing and type of introduction of gluten-containing foods into a child’s diet can influence the risk.
- Viral infections: Some viral infections (e.g. rotaviruses) can increase the risk of developing celiac disease by stimulating the immune system and triggering an autoimmune response.
- Stress and other health factors: There is evidence that physical or mental stress increases the risk of coeliac disease.
Symptoms of coeliac disease: recognizing signs and warning signals
Gluten intolerance can have both physical and systemic effects. The symptoms of coeliac disease are diverse and vary from person to person. Common symptoms are
Celiac disease symptoms in adults
- Loss of appetite
- Abdominal pain
- Bloating
- Diarrhea
- Anemia
- Iron deficiency and other vitamin deficiencies (e.g. vitamin B12, vitamin D)
- Exhaustion and tiredness due to a lack of nutrients
- Depressive moods, irritability or anxiety, often due to a lack of nutrients or an unclear burden of disease
- Dermatitis herpetiformis (itchy skin disease with blistering)
- Vomiting
- Joint and muscle pain
- Weight loss
- Bone pain and osteoporosis due to calcium and vitamin D deficiency
- Mundgeschwüre (Aphthen)
- Constipation
- Tooth damage
Celiac disease symptoms in young children
- Abdominal pain
- Diarrhea or bulky, strong-smelling stools
- Bloated belly
- Paleness
- Weight loss
- Nausea
- Delayed puberty
- Growth arrest or delay
In some cases, especially with silent coeliac disease, there are no obvious symptoms even though the small intestine is damaged. The disease therefore often goes unnoticed.
Celiac disease: diagnosis and examinations
Celiac disease is diagnosed by specific antibody detection and a biopsy of the small intestine. A reliable diagnosis is very important, especially for young children. If the disease remains undetected, it can lead to growth and development disorders. Due to the unspecific symptoms, it still takes an average of ten years, especially in older children and adults, before the “diagnosis of coeliac disease” is made.
The diagnosis of coeliac disease involves several steps and requires a combination of clinical assessment, laboratory tests and imaging procedures. First of all, the doctor will make a suspected diagnosis based on the patient’s symptoms and medical history. Particularly if coeliac disease is suspected, it is important that the person concerned continues to eat gluten before the diagnosis is made, as otherwise the tests may be unreliable.
Blood test
The first step towards diagnosis is usually a blood test, which looks for certain antibodies. The most important markers are tTG-IgA (transglutaminase antibody) and EMA (endomysium antibody). Elevated antibody levels often indicate coeliac disease, but can also occur in other diseases.
Intestinal biopsy
If the blood tests are positive, an intestinal biopsy is usually performed to confirm the diagnosis. Tissue is taken from the small intestine to look for typical changes in the intestinal mucosa, such as villous atrophy, i.e. the destruction of the finger-shaped protrusions of the mucosa that are important for the absorption of nutrients. The biopsy is the gold standard for the diagnosis of coeliac disease, as it provides direct evidence of damage to the small intestinal mucosa.
Genetic examination
In some cases, a genetic test can also be carried out to check the genetic predisposition. The presence of the HLA-DQ2 or HLA-DQ8 genes is associated with an increased risk of coeliac disease, but genetic testing is not sufficient for diagnosis, as not all carriers of these genes actually develop coeliac disease.
Coeliac disease: prevention, early detection, prognosis
Coeliac disease is a chronic autoimmune disease that is triggered by the consumption of gluten. Early diagnosis and a strict gluten-free diet are crucial for the quality of life of those affected. But are there ways to prevent coeliac disease? Can coeliac disease be detected early? And what is the prognosis for gluten intolerance? The most important answers:
Can coeliac disease be prevented?
You cannot currently prevent coeliac disease directly, as it is a genetic autoimmune disease. However, if you have an increased risk of developing coeliac disease due to carrying corresponding genes such as HLA-DQ2 or HLA-DQ8, you can try to minimize the risk of developing the disease. Early detection remains the best measure.
Coeliac disease: early detection with a blood test
Early detection of coeliac disease is mainly possible through blood tests for specific antibodies such as tTG-IgA and EMA. Elevated antibody levels can indicate coeliac disease, even if the symptoms are not yet clearly pronounced. If coeliac disease is suspected, especially in people at risk such as family members of sufferers, an early diagnosis can help to treat the disease in good time and prevent consequential damage. Confirmation is usually provided by an intestinal biopsy.
Coeliac disease: good prognosis with early diagnosis
The prognosis for coeliac disease is generally very good if the disease is detected early and treated consistently with a gluten-free diet. By avoiding gluten, the intestinal mucosa heals in most cases and the symptoms disappear. However, if left untreated, coeliac disease has serious long-term consequences for many sufferers, such as nutrient deficiencies, osteoporosis or even an increased risk of certain types of cancer. A timely and consistent gluten-free diet can prevent these complications and enable a normal life expectancy.
Treatment of coeliac disease: Why a gluten-free diet is essential
The treatment of coeliac disease essentially consists of a lifelong, strictly gluten-free diet. This means that if you are affected, you must avoid all foods containing wheat, rye, barley or other gluten-containing grains. By avoiding gluten, the intestinal mucosa usually heals and the symptoms disappear. In some cases, it may be necessary to take additional vitamins or minerals to compensate for the nutrient deficiencies caused by the damage to the small intestine.
After diagnosis, those affected receive comprehensive training and support from qualified specialists, for example from a legally recognized nutritionist.
Close medical supervision and regular check-ups are important to ensure that the diet is being followed correctly and that no further complications occur.
Details of the treatments
Frequently asked questions (FAQ)
The symptoms of coeliac disease are often non-specific and variable, ranging from diarrhea, bloating and abdominal pain to fatigue and weight loss. Iron deficiency, anemia, skin changes or depressive moods can also occur. Growth disorders are possible in children.
Coeliac disease can occur at any age, from infancy to adulthood. Certain triggers such as infections or hormonal changes can promote the onset of the disease or trigger the first symptoms.
No, people with coeliac disease are not necessarily always hungry. Some sufferers experience an increased appetite due to impaired nutrient absorption, while others tend to have a loss of appetite or an early feeling of fullness to the point of chronic nausea. The symptoms vary greatly from person to person and depend on the stage of the disease and other factors.
People with coeliac disease are not allowed to eat gluten. Gluten is found in wheat, spelt, rye, barley and foods made from them. Hidden gluten in processed products must also be consistently avoided.
Coeliac disease manifests itself through a misdirected immune reaction to gluten. This leads to inflammation and damage to the mucous membrane of the small intestine. The symptoms and their severity vary greatly from person to person.
Coeliac disease is caused by a genetic predisposition in combination with the intake of gluten and other unknown factors. Only in a small proportion of people with a genetic predisposition does gluten trigger an immune reaction in the intestinal mucosa. The immune system then reacts to gluten components with inflammation. Environmental factors such as infections can influence the development of the disease.
With a consistent gluten-free diet, people with coeliac disease have a normal life expectancy. The intestinal mucosa can fully recover and secondary diseases can be avoided. However, if left untreated, coeliac disease can lead to long-term health problems.
Antibodies against tissue transglutaminase (tTG-IgA) and endomysium (EMA-IgA) are typically elevated. Iron, vitamin B12 or folic acid deficiencies can occur as a result of inflammation of the small intestinal mucosa. For a reliable diagnosis, gluten must still be eaten before the blood test.
With untreated coeliac disease, the stool can be light, greasy and foul-smelling. The cause is impaired fat absorption in the small intestine. Some sufferers also see undigested food in their stools. With a gluten-free diet, bowel movements usually normalize.
In untreated coeliac disease, the specific IgA antibodies against tissue transglutaminase are usually significantly elevated. However, this value can also be falsely high in individual cases without coeliac disease. Therefore, a tissue sample from the mucous membrane of the small intestine (at least in adults), which is obtained with a gastrointestinal endoscopy, is part of a reliable diagnosis. The total IgA value may be normal, but should also be determined. In the case of IgA deficiency, alternative IgG-based tests are used.
It makes sense to repeat thegastroscopy regularly to monitor the course of the disease and the healing of the small intestine. However, this depends on the response to the gluten-free diet and whether there are signs of renewed intestinal damage. The frequency and necessity of repetition can vary from individual to individual. Typically, after the diagnosis and the first gastroscopy, a follow-up examination is recommended after about 1-2 years. In some cases, later monitoring may also be useful if there are complaints or doubts about complete healing.
With coeliac disease, even a very small amount of gluten that is accidentally ingested can trigger a reaction in the body. Even if the symptoms are not always immediate or clearly noticeable, small dietary errors can be harmful in the long term. On the other hand, there are reports that rare dietary errors (e.g. accidental gluten ingestion during a meal in a restaurant) have no consequences for many sufferers. Constant fear of making dietary mistakes is therefore just as pointless as a lack of consistency in the diet.


