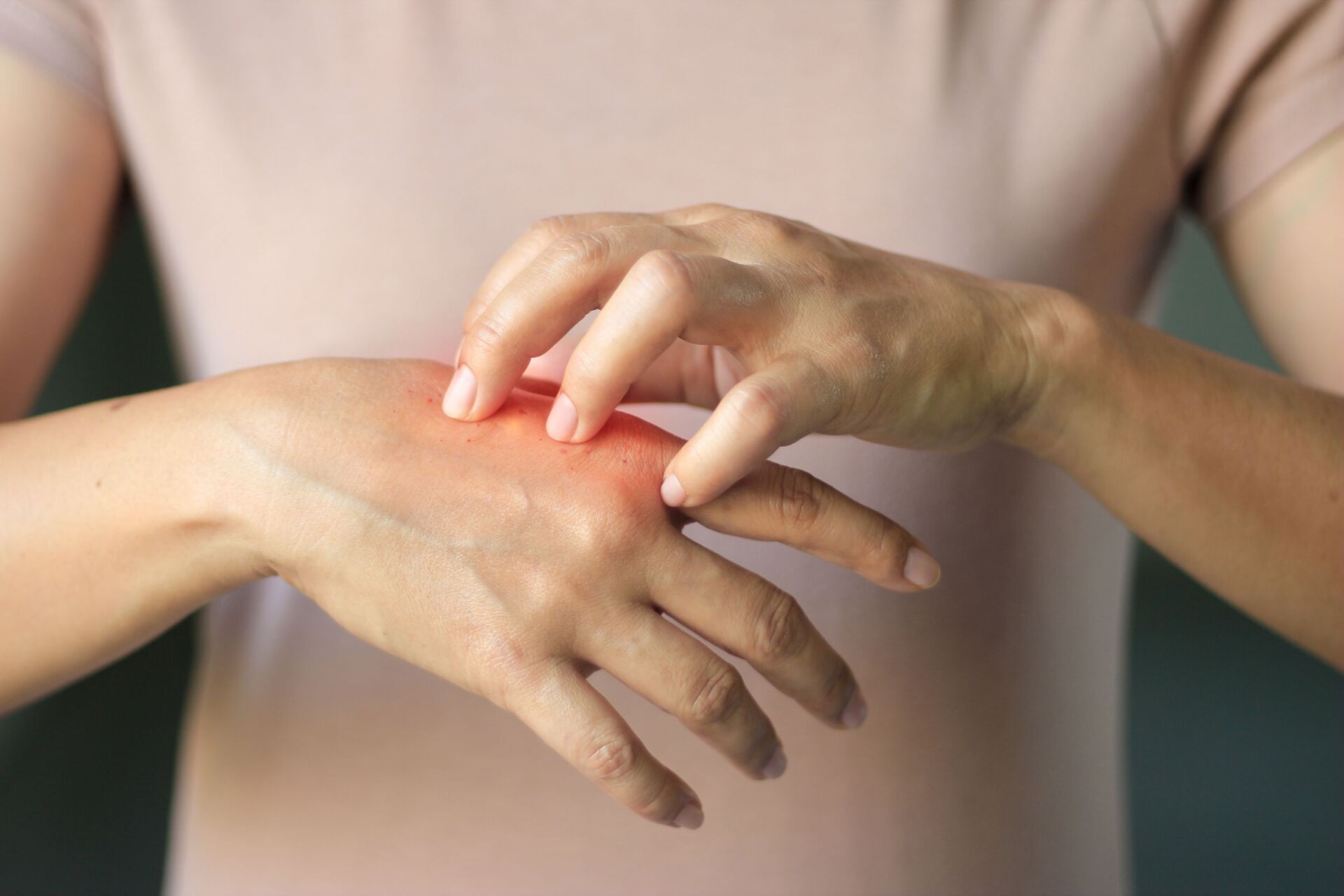
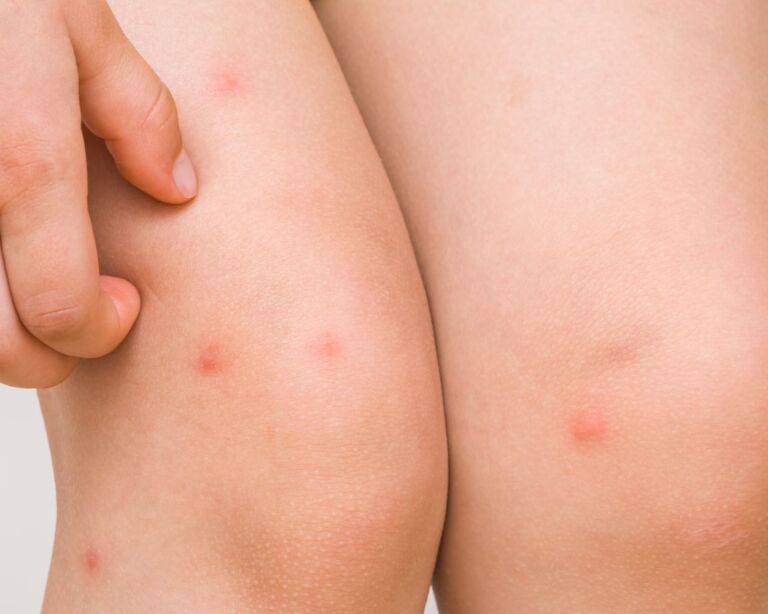
What is eczema?
Eczema is an inflammatory reaction of the uppermost layers of the skin that can be triggered by various external and internal factors. The skin reacts with an inflammatory reaction, which manifests itself in characteristic symptoms.
Eczema is not contagious, but can have a significant impact on quality of life. The main symptom is usually severe itching, accompanied by reddening of the skin, scaling and in some cases weeping skin changes.
Eczema types
Eczema can be acute or chronic and can occur almost anywhere on the body. A distinction is made between different types of eczema depending on the cause and appearance:
By pathogenesis (mechanism of development)
Endogenous eczema: caused by internal, usually genetic or immunological factors.
- Atopic eczema (neurodermatitis) – genetic predisposition, impaired skin barrier, tendency to skin inflammation
- Seborrheic eczema – excessive sebum production, reaction to skin yeasts(Malassezia furfur)
- Nummular (microbial) eczema – unclear cause, often associated with dry skin
- Dyshidrotic eczema (pompholyx) – multifactorial (stress, sweat, contact substances)
Exogenous eczema: triggered by external stimuli (chemical, physical, microbial)
- Allergic contact dermatitis – late allergic reaction (type IV) to contact allergens (e.g. nickel, fragrances)
- Irritant-toxic contact dermatitis – direct damage caused by irritants (e.g. detergents, acids)
- Photoallergic / phototoxic eczema – combination of light and photosensitizing substances
- Stasis dermatitis – the result of chronic venous insufficiency, usually on the lower legs
Mixed / multifactorial eczema: combination of internal and external influences
- Microbial eczema – occurs secondary to bacterially infected wounds or fungal infections
According to morphology (clinical appearance)
- Acute eczema: redness, edema, blisters (vesicles), oozing, crusts. B. acute contact dermatitis, acute atopic flare-up
- Subacute eczema: transitional form; scaling, crusts, moderate oozing
- Chronic eczema: thickened skin (lichenification), cracks, hyperkeratosis, often hyperpigmentation. B. chronic neurodermatitis, lichen simplex chronicus
- Nummular eczema: coin-shaped, scaly, weeping plaques
- Dyshidrotic eczema: itchy, deep blisters on the palms of the hands or soles of the feet
- Seborrheic eczema: greasy, yellowish scales on a reddened background
By localization
- Face / scalp: Seborrheic eczema, atopic eczema (especially in infants), contact eczema (e.g. cosmetics, eyeglass metal)
- Hands / forearms: Irritant-toxic eczema, Allergic contact dermatitis, Dyshidrotic eczema
- Bends (elbows, back of the knee): Atopic eczema (flexural eczema)
- Lower leg: stasis dermatitis (venous), microbial eczema
- Trunk / extensor sides: Nummular eczema, atopic eczema (in adults)
- Sun-exposed areas: photoallergic or phototoxic eczema
- Genital / perianal area: contact eczema (e.g. due to hygiene products, moisture), atopic eczema
The most common types of eczema
Atopic eczema (neurodermatitis): is a chronic skin disease that is genetically determined. It frequently occurs in childhood and is often associated with other atopic diseases such as asthma or hay fever.
Contact eczemaContact dermatitis : caused by direct contact with irritating or allergenic substances. They can be either allergic or irritant and are usually limited to the area of skin that has come into contact with the triggering substance.
Seborrheic eczema: mainly affects areas of skin rich in sebaceous glands. It often occurs on the scalp, face and upper body and is associated with excessive sebum production.
Dyshidrotic eczema: occurs mainly on the hands and feet. It is characterized by small, very itchy blisters, which are often accompanied by increased sweating.
Nummular eczema: manifested by coin-shaped, round skin lesions. It usually occurs on the arms and legs and is more common in men.
Eczema: causes and risk factors
The development of eczema is complex and can have various causes. There is often a disturbed skin barrier which, together with immunological reactions, leads to inflammation. Frequent triggers are:
Genetic factors
- Inherited predisposition to skin diseases
- Familial clustering of allergies
- Impaired skin barrier function
Environmental factors
- Contact with irritants (soaps, cleaning agents, chemicals)
- Allergens (nickel, fragrances, preservatives)
- Climatic conditions (dry air, extreme temperatures)
Psychological factors
- Stress and emotional strain
- Lack of sleep
- Mental illnesses
Other factors
Symptoms: Recognizing eczema
Eczema manifests itself through characteristic skin changes that can vary depending on the stage and type. The main symptom of most eczema is itching.
Acute phase:
- Severe reddening of the skin
- Bubble formation
- Intense itching
- Weeping skin areas
- Swelling of the affected areas
- Crust formation due to scratching
Chronic phase:
- Scaling
- Skin thickening (lichenification)
- Very dry, cracked skin
- Coarser, leathery skin texture
- Persistent itching
Side effects:
- Sleep disturbances due to nocturnal itching
- Secondary skin infections due to scratching
- Mental stress
- Reduction in quality of life
Medical checkup – more information
Send a photo of the affected skin area and fill out the short questionnaire. Within 24 hours on weekdays, you will receive a reliable diagnosis from our experts. Your data will be transmitted to us encrypted and treated confidentially.
Diagnosis of eczema
The diagnosis of eczema is mainly based on clinical examination and a detailed medical history. There is no specific laboratory test for most types of eczema.
Diagnostic steps:
- Detailed questioning about symptoms and triggers
- Physical examination of the skin
- Allergy tests for suspected contact dermatitis
- Exclusion of other skin diseases
- Skin biopsy if necessary in unclear cases
Eczema: prevention, early detection, prognosis
Prevention:
- Consistent skin care with moisturizing products
- Avoidance of known triggers
- Stress reduction
- Appropriate clothing (breathable, non-scratching)
- Protection against extreme temperatures
Prognosis
The prognosis of eczema varies depending on the type and severity. Many types of eczema, especially atopic eczema, often disappear or recede significantly by adulthood. With consistent treatment and avoidance of triggers, most eczema can be well controlled.
Tips for preventing eczema
Skin care
The skin should be regularly creamed with oily or moisturizing lotions to strengthen the natural barrier. It is advisable to use mild, soap-free cleansing products and to avoid hot water when showering or washing. In addition, the skin should not be washed too often in order to preserve its natural oils. After bathing or showering, the skin should be creamed immediately, especially if it is dry.
Protection from irritants
Gloves should be worn when working with cleaning agents, gardening or in contact with chemicals. People who are allergic to certain substances should avoid them, for example jewelry, cosmetics or other products. Cotton clothing is kinder to the skin than wool or synthetic materials and can reduce irritation.
Environment and lifestyle
The air in living spaces should be kept humid, especially in winter, to avoid dry skin. Excessive sweating should be avoided as it can trigger eczema flare-ups. Stress also has a negative effect on the skin, so relaxation techniques such as yoga or meditation can be helpful.
Nutrition and general health
A balanced diet supports skin health. People with known allergies should recognize them early and avoid them, especially if they have an atopic predisposition. Drinking enough fluids also helps to support the skin from the inside.
Specific prevention for risk groups
Children with a genetic tendency to atopic eczema should be regularly moisturized from an early age to prevent flare-ups. People who frequently come into contact with water or chemicals at work should use hand protection and barrier ointments. Anyone who spends a lot of time in the sun should use sun protection to prevent phototoxic eczema.
Eczema: Treatment with individual therapy
The treatment of eczema depends on the type, severity and localization of the eczema. The basis of any therapy is intensive skin care and the avoidance of triggers.
Basic treatment principles:
Skin care
- Regular use of moisturizers
- Use mild, pH-neutral cleaning products
- Applying care products to skin that is still damp
Medication
- Topical corticosteroids for acute inflammation
- Calcineurin inhibitors (tacrolimus, pimecrolimus) as an alternative
- Antihistamines for severe itching
- Antibiotics for bacterial superinfections
Systemic therapy
- Phototherapy
- In severe cases: systemic immunosuppressants
- Biologics for therapy-resistant forms
Supporting measures
- Cool, moist compresses for acute flare-ups
- Stress reduction and relaxation techniques
- Patient education and counseling
- Psychological support if required
Frequently asked questions about eczema
No, eczema is not contagious. These are inflammatory skin reactions that cannot be transmitted from person to person.
Many eczemas can be successfully treated and controlled. Chronic forms such as neurodermatitis are often not curable, but can be managed well with the right therapy.
Nutrition only plays a relevant role in eczema (especially atopic dermatitis) in a small proportion of patients. An elimination diet should only be carried out if a food allergy is confirmed and under medical supervision. Routine dietary restrictions are not recommended for eczema patients without a proven allergy.
A doctor should be consulted if the skin is severely inflamed, weeping, painful or affected by recurrent flare-ups, or if the symptoms do not improve despite care and protective measures.
Eczema is known in dermatology as an inflammatory skin disease that has a variety of causes. These include a genetic predisposition, which weakens the skin’s natural protective barrier, as well as various external factors: Allergens such as house dust mites or nickel, irritating substances such as cleaning agents or fragrances, but also heat, sweating, stress, dry air in winter and contact with certain plants or animals. All these factors can trigger eczema or aggravate existing skin changes.