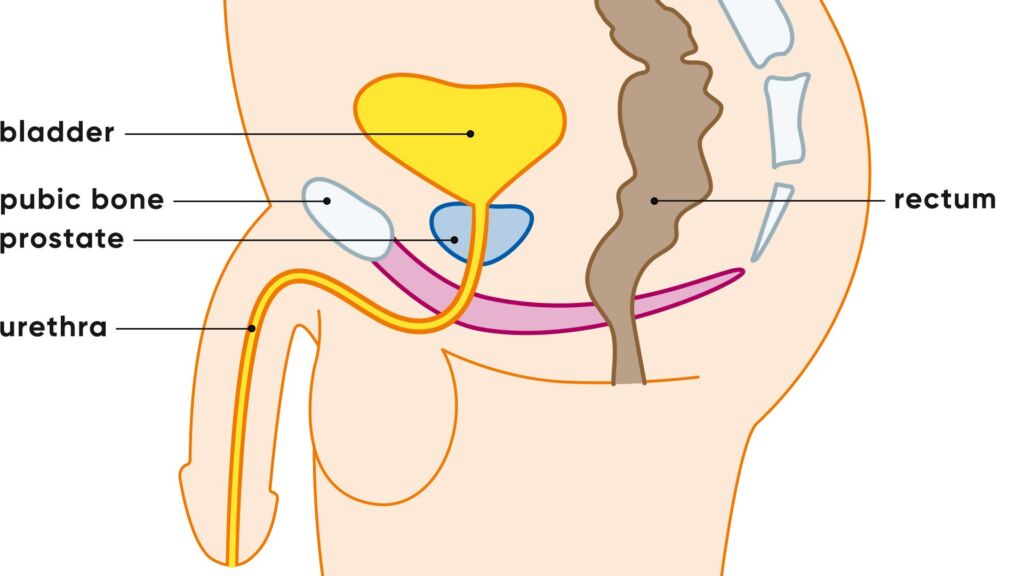
Task and function of the prostate and prostate secretion
The prostate is a small but very important organ in the male body. Their main function is to produce part of the seminal fluid. This is not a simple “side dish”. The prostate secretion protects and supplies the sperm with important nutrients and enzymes that increase their motility and ability to survive. This increases the probability that the sperm will be successful in reproduction.
During ejaculation, the muscle fibers in the prostate contract and push the fluid produced into the urethra. There it mixes with the sperm from the testicles and the fluid from the seminal vesicles. This mixture forms the ejaculate.
In addition to its crucial role in reproduction, the prostate also has an important function in the urinary tract. It surrounds the upper part of the urethra, through which urine passes from the bladder to the outside. As long as the prostate is healthy, it has hardly any influence on urination. However, if it becomes enlarged or inflamed, it can restrict the flow of urine. This can lead to symptoms such as a frequent urge to urinate or a weak urine stream.
The prostate is also involved in hormonal processes, as it reacts to male sex hormones (androgens) and increases their effect. These hormones influence both the growth of the prostate and its function.
PSA – the prostate-specific antigen: Function in the prostate
PSA is a special enzyme that is produced by the cells of the prostate. It is part of the seminal fluid and has an important task: it helps to make the ejaculate more fluid after ejaculation. This allows the sperm to move better and gives them a better chance of reaching an egg. This means that PSA ensures that the semen is not too viscous and that the sperm can swim freely.
Small amounts of PSA can be detected in the blood. An elevated PSA level may indicate changes or diseases of the prostate, such as inflammation, benign enlargement, or prostate cancer. This is why PSA is often used as an important value in prostate screening.
The role of the prostate in hormone metabolism (DHT)
The prostate is a hormone-dependent organ, which means that it reacts in particular to male sex hormones, the so-called androgens. The most important androgen is testosterone, which is mainly produced in the testicles.
In the prostate, testosterone is converted into a stronger form, dihydrotestosterone (DHT), by an enzyme. This hormone is crucial for the growth, development and function of the prostate. It ensures that the glandular cells remain active and that prostate secretions are produced.
The prostate is heavily dependent on male hormone metabolism. The balance of androgens regulates their growth and function, which is why changes in the hormone balance can affect the health of the prostate.
How does the prostate support ejaculation?
The prostate plays a central role in ejaculation. It produces a special, milky secretion that contains important components such as enzymes (e.g. PSA), zinc and citric acid. In the urethra, this secretion mixes with the sperm from the testicles and the secretion from the seminal vesicles. Together they form the ejaculate.
During orgasm, the smooth muscles of the prostate contract rhythmically and actively push the prostate secretions into the urethra. At the same time, a closing mechanism ensures that no urine gets into the ejaculate and that the ejaculate does not flow back into the bladder. The prostate makes a decisive contribution to the reproductive function by releasing the ejaculate completely and in a targeted manner.