In principle, a distinction is made between localized and metastasized, advanced disease. Various treatment methods are available for prostate cancer, such as the pure monitoring strategy, radiotherapy, radical surgery, gentle focal therapies (such as HIFU) through to system therapies such as hormone or chemotherapy treatment.
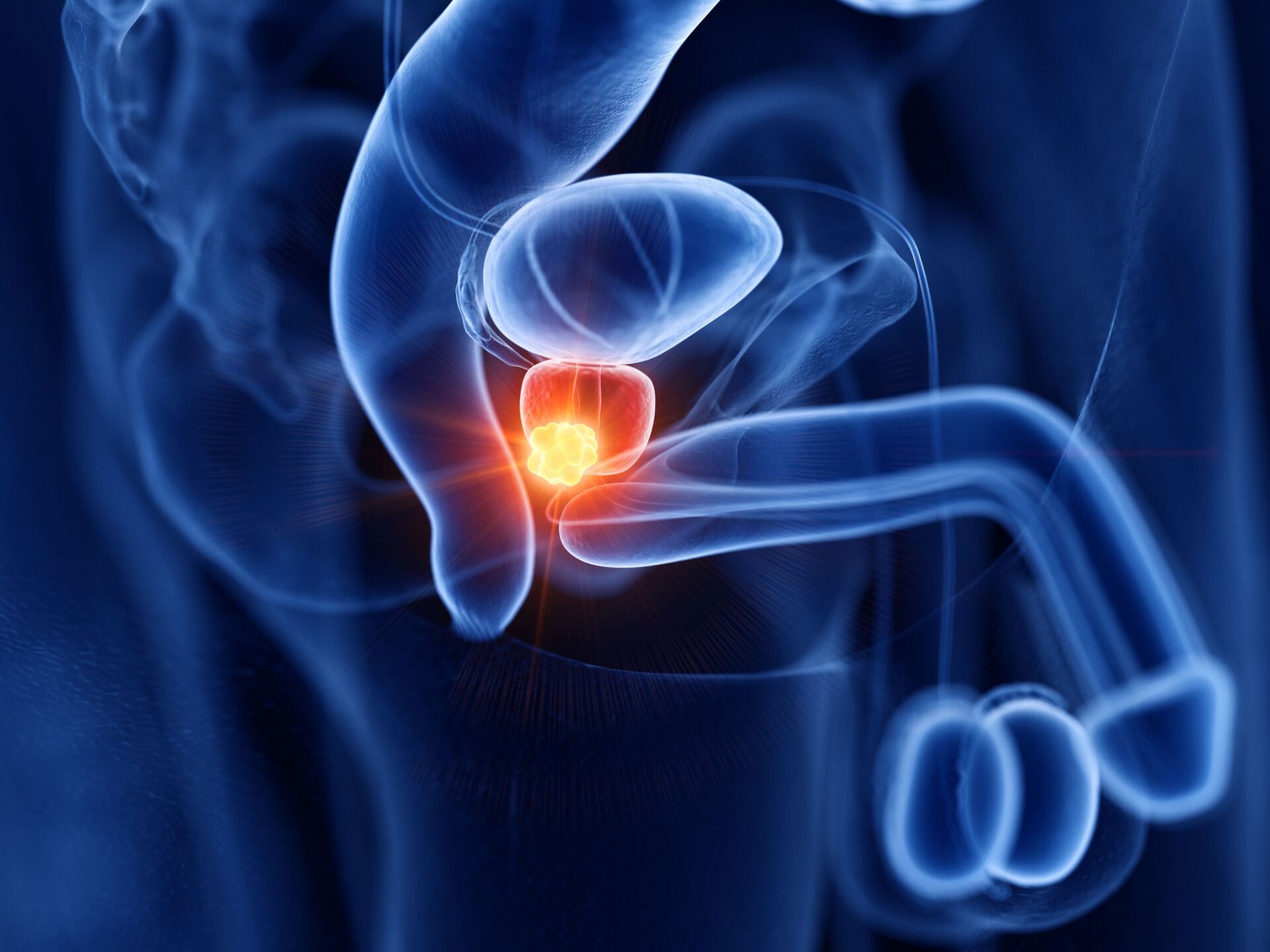
What is a prostate tumor?
Prostate cancer is the most common cancer in men in Switzerland and worldwide. It usually occurs after the age of 65.
Many prostate tumors grow very slowly and do not cause any problems for those affected and are often only discovered by chance, e.g. during autopsies of deceased patients (so-called latent carcinomas). However, prostate tumors can also be associated with symptoms or grow rapidly and subsequently require treatment.
If you have prostate cancer, the earlier the prostate tumor is detected, the greater your chances of recovery. As its symptoms usually only show up late, a medical screening examination from the age of 50 helps to detect the tumor in good time (so-called risk screening).
Prostate cancer – frequency and age
Around 7,100 men are diagnosed with a prostate tumor in Switzerland every year; this accounts for around 29 percent of all cancer cases in men and makes the tumor the most common type of cancer in the male population in Switzerland.
Around 19 percent die of prostate cancer, or around 1,400 men every year. This makes prostate cancer the second most common cause of death among all types of cancer in men in Switzerland.
Almost half of those affected are older than 70 when they are diagnosed with prostate cancer. Only a few patients are younger than 50. For a 35-year-old, the risk of developing a prostate tumor in the next ten years is around 0.1 percent. For a 75-year-old, on the other hand, the risk is around five percent.
Frequency and age at risk of prostate cancer
The greatest risk factor for the occurrence of prostate cancer is age. Carcinomas of the prostate gland only form very rarely at a young age.
Another risk factor is familial clustering. If you have a father or brother who has prostate cancer, your own risk of also developing a prostate tumor is doubled. If both (father and brother) have prostate cancer, your risk increases at least fivefold. The hereditary predisposition also increases the risk of developing prostate cancer at a younger age. Such genetic factors play a role in every fifth to tenth man who develops a prostate tumor.
Whether a certain lifestyle increases the risk of developing prostate cancer has not been proven beyond doubt. However, it is assumed that, for example, a lack of exercise or an unhealthy diet (e.g. food that is too sweet and high in fat) promotes cancer.
However, according to the current state of scientific knowledge, a benign enlargement of the prostate (benign prostatic hyperplasia) is very unlikely to develop into a prostate tumor.
Prostate cancer symptoms
A tumor often does not cause any specific symptoms at an early stage. However, the risk of developing symptoms increases with the size of a tumor:
- Difficulty urinating. If your prostate increases in size due to a tumor, the urethra becomes narrower. Your urine stream will become weaker, you may need to go to the toilet more often and you may need longer to urinate than usual. However, these signs can also indicate benign prostate enlargement, but should always be clarified by a doctor to rule out malignant disease.
- Blood in urine. The cause could be prostate cancer, but it could also be a disease of the bladder or kidneys, for example. Immediate clarification is necessary.
- Blood in the seminal fluid. The cause of so-called hemospermia could be a prostate carcinoma, but also an infection of the urethra or epididymis, for example. Immediate clarification is necessary.
- Pain when ejaculating. Painful ejaculation that causes discomfort in the pelvis or back, for example, can indicate prostate cancer, but also inflammation of the prostate. This inflammation, called prostatitis, is caused by bacteria, for example. Immediate clarification is necessary.
- Potency disorders. They can also occur as a side effect of prostate cancer. However, there are many possible causes of erectile dysfunction, for example vascular calcification, high blood pressure, diabetes or psychological reasons. Immediate clarification is necessary.
You should always consult your family doctor or urologist.
Prostate Cancer Center
At the USZ, numerous specialist departments have joined forces to form a prostate cancer center. The center is certified according to the guidelines of the German Cancer Society (DKG). A team of experts specializing in the medical treatment of prostate cancer works closely together here for the benefit of our patients and discusses each case on an interdisciplinary basis at a tumour board. At DKG-certified centers, patients are treated according to strict quality criteria and, according to current studies, have a better chance of survival on average.
Preventing prostate cancer and early detection
So far, no specific behaviors such as certain environmental toxins or the frequent consumption of certain foods have been directly linked to prostate cancer. In general, a healthy lifestyle with a varied diet and physical activity helps to maintain health and speed up recovery in the event of illness.
We recommend that all men over the age of 50 attend regular prostate cancer screenings with their family doctor or urologist. You should take advantage of this option from the age of 45 if your close male relatives (father, brother, grandfather, uncle) have been diagnosed with prostate cancer.
The screening examination at our clinic usually consists of a detailed consultation with your urologist and a PSA blood test (see Diagnosis). Palpation (digital rectal examination (DRU)) is now only rarely used. At the USZ, we also use a new generation of prostate cancer screening, namely a blood test that examines other genetic biomarkers in addition to the protein marker PSA. This new test is called the Stockholm3 test.
Medical checkup – more information
Prostate cancer diagnosis
As with the screening examination, your urologist will first take a careful history of your symptoms, including questions about prostate cancer in the family. The next step for your doctor will be a physical prostate examination. We usually use the following examinations and tests:
- Palpation examination: During this examination, the doctor inserts an index finger into your rectum. This allows him to feel the prostate through the bowel wall and recognize its circumference. This method is also known as a “digital rectal examination” (DRU). It is only rarely used at the USZ, as we now have more precise examination methods at our disposal.
- PSA blood test: This blood-based laboratory test determines how much PSA is present in your blood. PSA (prostate-specific antigen) is a protein that is only produced by the prostate. If your PSA value is above 4 nanograms per milliliter, this may be an indication of a possible prostate tumor; if the value is above 10 nanograms per milliliter or higher, the risk of a malignant tumor increases. Other reasons for an increased value include inflammation of the prostate (prostatitis), benign prostate enlargement or activities that stimulate the prostate such as sexual intercourse and cycling that were performed shortly beforehand.
- Stockholm3 test: In addition to the PSA protein, this test determines other proteins and over 100 different genetic biokmakers in the blood. Together with clinical information on age, family risk and medication intake, the blood analysis is used to calculate a prostate cancer risk assessment. Due to the large number of factors involved, the calculated risk value is more accurate than the PSA test alone.
- Prostate-specific magnetic resonance imaging (MRI): With the help of this imaging procedure, the doctor can see in which area your prostate has enlarged. There are also indications as to whether a benign enlargement of the prostate, an inflammation or an actual tumor is present. Magnetic resonance imaging (MRI), also known as magnetic resonance imaging, does not generate X-rays.
- Tissue sample (biopsy): If previous examinations have confirmed your suspicion of prostate cancer, a biopsy can provide the desired clarity. Using imaging techniques such as MRI and ultrasound, suspicious areas of the prostate can be sampled in a more targeted manner (fusion-supported template biopsy). A pathologist uses a microscope to determine whether cancer cells are present in the tissue removed from your prostate.
PSA value prostate
PSA (prostate-specific antigen) is a protein that is produced by cells in the prostate, a gland of the male reproductive system, and serves to liquefy the ejaculate. Since cancer cells produce considerably more PSA than healthy prostate cells, this value is well suited as a tumor marker and helps to detect prostate carcinoma and monitor the disease. However, the size of the prostate can also influence the PSA value – the larger the prostate, the higher the value. An elevated PSA value can therefore not only indicate prostate cancer, but also other diseases such as prostatitis (inflammation of the prostate) or benign prostatic hyperplasia (BPH, benign enlargement of the prostate). Prostate stimulating activities such as cycling, horse riding or sex also influence the PSA value. These activities should be avoided at least two days before a PSA analysis.
If the PSA value is slightly elevated (3-10 ng/ml), the test is repeated after a few weeks (important: in the same laboratory). In consultation with the doctor, further investigations such as an MRI and tissue sampling (biopsy) are carried out in the event of elevated PSA values. PSA values are always considered in the context of age, health status and other clinical findings.
How can the PSA value be lowered?
There are drugs and treatments that can lower PSA levels. For example, certain drugs used to treat an enlarged prostate, such as finasteride or dutasteride, can lead to a reduction. Surgical removal of the prostate in the case of benign enlargement of the prostate as well as radiotherapy and hormone therapy also have a lowering effect on the value.
Lowering the PSA level is not a treatment for prostate cancer. The PSA value is merely a biomarker that indicates changes in the prostate, but is not the cause.
Second opinion for prostate cancer
When a cancer diagnosis is made, a second medical opinion is an important decision-making tool. The Comprehensive Cancer Center Zurich supports you with a professional expert opinion. They receive a thorough analysis of the situation as well as personal advice and quick answers to their questions.
Prostate cancer life expectancy and progression
As long as a prostate tumor is limited to the prostate gland itself (local disease), the chances of recovery are very good. In this case, more than 90 percent of all treated patients with prostate cancer survive.
In the case of metastatic disease (metastases form in other organs), the aim of treatment is to stabilize the disease for as long as possible. The bones (e.g. spine, ribs, pelvis) and the lymph node regions in the body are most frequently affected by metastases. However, metastases can also develop in the liver and lungs.
Effective treatment for prostate cancer
Various therapy methods are available for the treatment of prostate tumors. Which of these types of treatment your doctor will recommend depends on various factors. For example, the histological tissue differentiation, the size of the tumor, the PSA value and its doubling time, whether the disease is localized or already metastasized, as well as the patient’s concomitant diseases and age. All prostate cancer cases treated by us are discussed in an interdisciplinary tumor board of the Prostate Cancer Center in order to be able to give the patient well-founded therapy recommendations.
In addition to clinical prostate cancer studies, the University Hospital Zurich is also actively involved in researching and developing new therapies and diagnostic approaches for prostate cancer in order to continuously improve treatment options and enhance patients’ quality of life.
Details on prostate cancer treatments
Frequently asked questions about prostate cancer
Prostate surgery can be considered as a treatment option if benign enlargements block the flow of urine and medication does not bring any improvement, or in the case of prostate cancer if it is confined to the prostate.
Prostate problems can include various conditions, including benign prostatic hyperplasia (BPH, benign enlargement of the prostate), prostatitis and prostate cancer. These conditions can lead to symptoms such as an increased urge to urinate, pain in the pelvic area and problems urinating. It is important to consult a doctor if symptoms occur in order to obtain an accurate diagnosis and appropriate treatment. Problems with the prostate can be treated. Do not accept this as part of the ageing process. Get active!
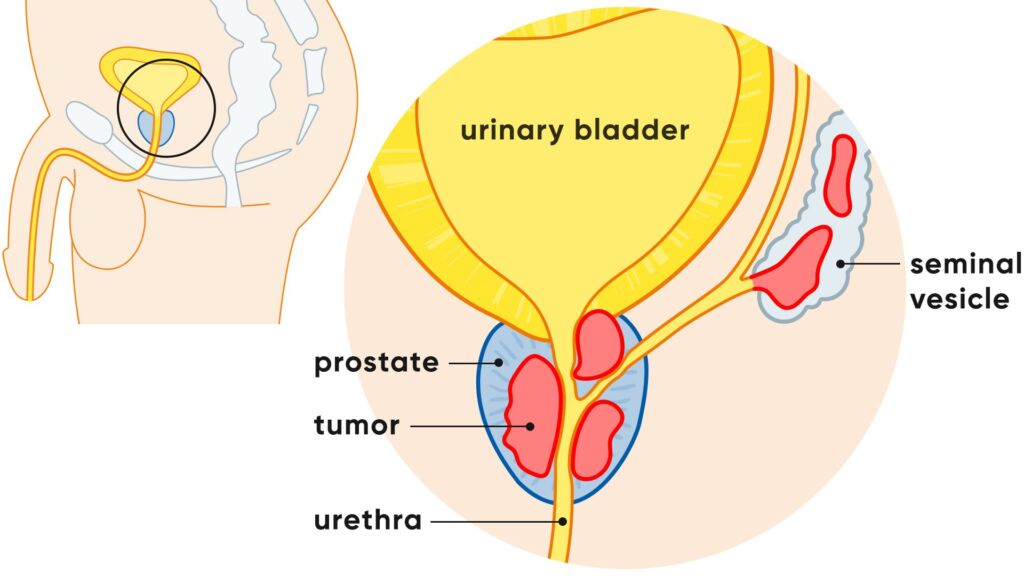
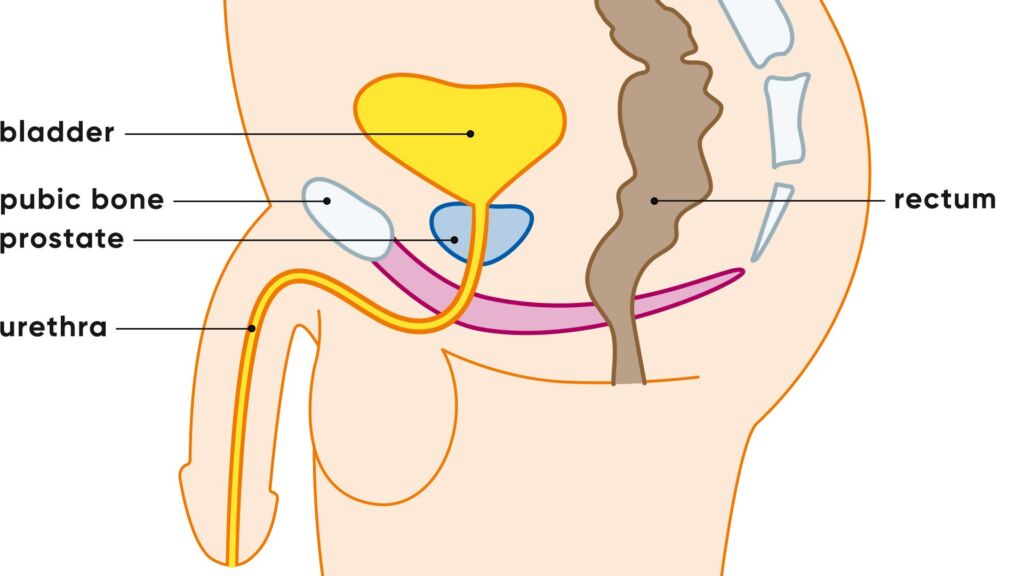
The prostate is a sex gland in the male reproductive system that lies directly under the bladder and surrounds the initial part of the urethra. It is roughly the size and shape of a chestnut. The prostate produces a secretion that forms an essential component of semen.
The prostate produces a secretion that helps to nourish and protect the sperm in the ejaculate. This fluid makes up a significant part of the ejaculate and helps to make it thin and protect the sperm in the acidic environment of the vagina. In addition, the position of the prostate and the muscle-controlled internal changes in shape ensure that either only sperm or only urine comes out of the penis.
Prostate cancer is detected at an early stage using blood tests such as the PSA test (prostate-specific antigen) or the Stockholm3 test. Symptoms usually only appear at a later stage and can include difficulty urinating, frequent urination, pain when ejaculating or blood in the urine or semen. If you have these symptoms, please see your doctor immediately. We recommend that men should have regular prostate checks from the age of 50, and from the age of 45 if they have a family history of prostate cancer (father, brother with prostate cancer).
The treatment of prostate cancer depends on the stage of the cancer, the histological classification, the patient’s state of health, age and personal preferences and life situation. Prostate cancer treatment can include radical removal of the prostate, focal therapy such as HIFU (High Intensity Focal Ultrasound), radiotherapy, hormone therapy, chemotherapy or a combination of these treatments. Active surveillance may be an option if the disease progresses slowly at an early stage.
Prostate cancer is primarily treated with medical treatments such as surgical removal of the prostate, focal therapy such as HIFU (High Intensity Focal Ultrasound), radiotherapy, hormone therapy and, if necessary, chemotherapy. If the disease is not very aggressive and at an early stage, it can be monitored closely (active surveillance) rather than actively treated. Accompanying measures such as a healthy diet, sufficient exercise and psychological support can support the success of treatment.
Yes, the prostate can be surgically removed. This surgical procedure is known as a radical prostatectomy. A prostatectomy is a treatment option for cancer that is confined to the prostate (localized) and has not metastasized. The entire prostate is removed. We do this using robotic surgery with the DaVinci surgical robot.
You can live well without a prostate. Side effects such as incontinence and erectile dysfunction may occur for some time after the procedure. Continuous pelvic floor training, which begins before the operation, can provide very good support.