In leukemia, cells from which white blood cells develop multiply uncontrollably. Acute forms can quickly become fatal if left untreated. In recent years, research has discovered more and more about the causes of blood cancer. This makes more precise treatments possible.
Text: Helga Kessler
An inflammation in the mouth that does not heal. The nose that keeps bleeding. Wounds that do not close. The feeling of being tired and listless all the time. “If such symptoms occur over a longer period of time, this could be an indication of leukemia,” says Antonia Müller, senior physician at the Clinic for Medical Oncology and Haematology: “People often don’t think about it.” A simple blood count usually provides the first important indication of the diagnosis.
As with any cancer, blood cancer cells multiply uncontrollably – in this case, these are early developmental stages of blood cells in the bone marrow. This results in many immature, non-functional white blood cells. Two types of cells can be affected: myeloid or lymphoid. In healthy people, phagocytes of the immune system develop from the myeloid cells, while the specific and long-lived T and B lymphocytes, which are important for immune defense, develop from the lymphoid cells.
If the blood cells “degenerate” at a very early and immature stage of their development and the cancer cells divide correspondingly quickly, this is referred to as acute leukemia – in contrast to slowly progressing senile leukemia. Healthy blood formation is often suppressed, which, if left untreated, leads to the death of the patient within a few weeks or months. In the past, only chemotherapy was available for treatment. The more aggressive the cancer, the higher the dosage. However, cytostatic drugs not only kill cancer cells, they also cause a lot of damage to healthy tissue. “A brutal method,” says Antonia Müller.
Chemotherapy as first choice
Chemotherapy is still the first choice today, even after a relapse. However, targeted therapies are now also possible. This is due to the fact that basic research has discovered a lot about the exact causes of leukemia in recent years. “Today, we can differentiate between many different subtypes of leukemia and thus see much better which patients we need to treat particularly intensively so that we achieve the best possible chance of recovery,” says blood cancer specialist Antonia Müller.
For an exact diagnosis, bone marrow is taken and examined using various methods: Exactly which cell types are involved, B or T cells, how mature or immature are they, are the chromosomes or genes altered, etc.? The examination results determine the future treatment plan. Chemotherapy is often combined with immunotherapy or another targeted therapy. “We can cure a good proportion of leukemias in this way today,” says Antonia Müller.
The prognosis is particularly favorable for children, whose chances of recovery from acute lymphoblastic leukemia are over 80 percent, compared to 40 to 50 percent for adults with the same type of leukemia. One reason for this is that children tolerate much higher doses of chemotherapy drugs than older adults, who often have previous illnesses. “But the biology of the disease is probably also different,” says Antonia Müller. Whether a targeted therapy or an immunotherapy can be used and which one exactly is chosen depends on certain properties on the surfaces of the cancer cells. If the target structure is known, antibodies or targeted small molecules can be produced that either attack the cancer cell directly or by activating the immune system.
Targeted with antibodies
The antibody Rituximab selectively binds to the CD20 antigen, a surface structure that is found on healthy B lymphocytes, but also on many degenerated B lymphocytes. Rituximab was one of the first monoclonal antibodies and was used from the late 1990s for the treatment of lymphoma and chronic lymphocytic leukemia. In the meantime, further antibody-based immunotherapeutics have been developed for the treatment of B cell tumors that are directed not only against CD20, but also against other surface features.
The latest developments are so-called chimeric antigen receptor or CAR-T cells, which boost the immune response and are used in lymphomas, but also in children and young adults with acute lymphoblastic leukemia (see box). “In the case of myeloid leukemias, which mainly affect older people, there are only a few highly potent immunotherapeutic agents that we can use to attack the cancer cells,” says Antonia Müller.
Transplantation of stem cells
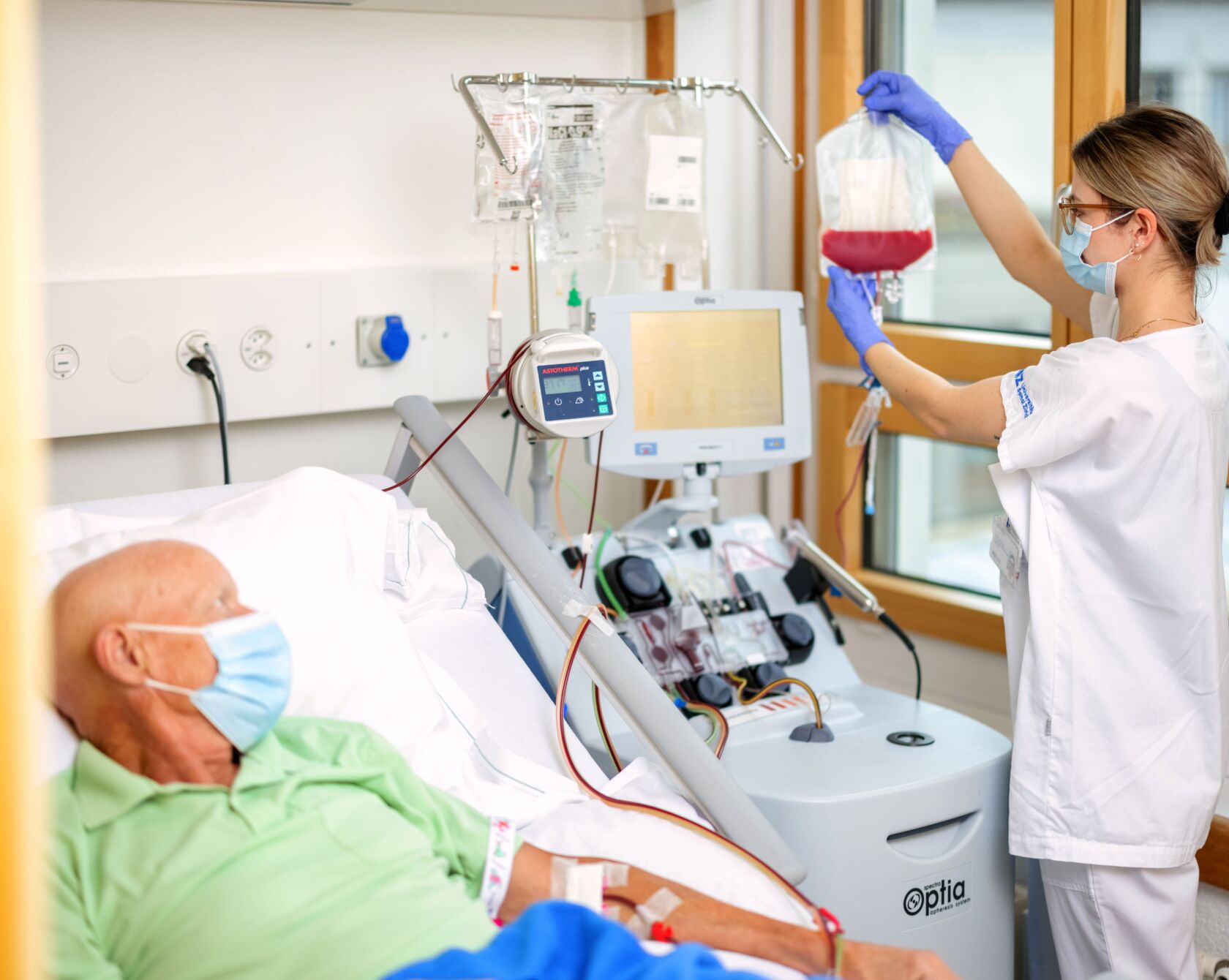
Depending on the prognosis of the disease, chemotherapy and immunotherapy can be supplemented by an “allogeneic stem cell transplant”. Before the transfer of healthy donor cells, the patient’s entire hematopoiesis and immune barrier is destroyed with high-dose chemotherapy. Transplantation with donor cells is also basically an immunotherapy because the transplanted cells not only contain blood stem cells, which are responsible for future blood formation in the recipient, but also immune cells from the donor. This donor immune system can grow firmly in the body, remain there for years and eliminate recurring cancer cells.
There is no strict age limit for stem cell transplants, says Müller, even 70-year-olds can benefit from them. However, it is important to clarify which concomitant illnesses are present and the patient’s general state of health: “It always depends on the individual case.”