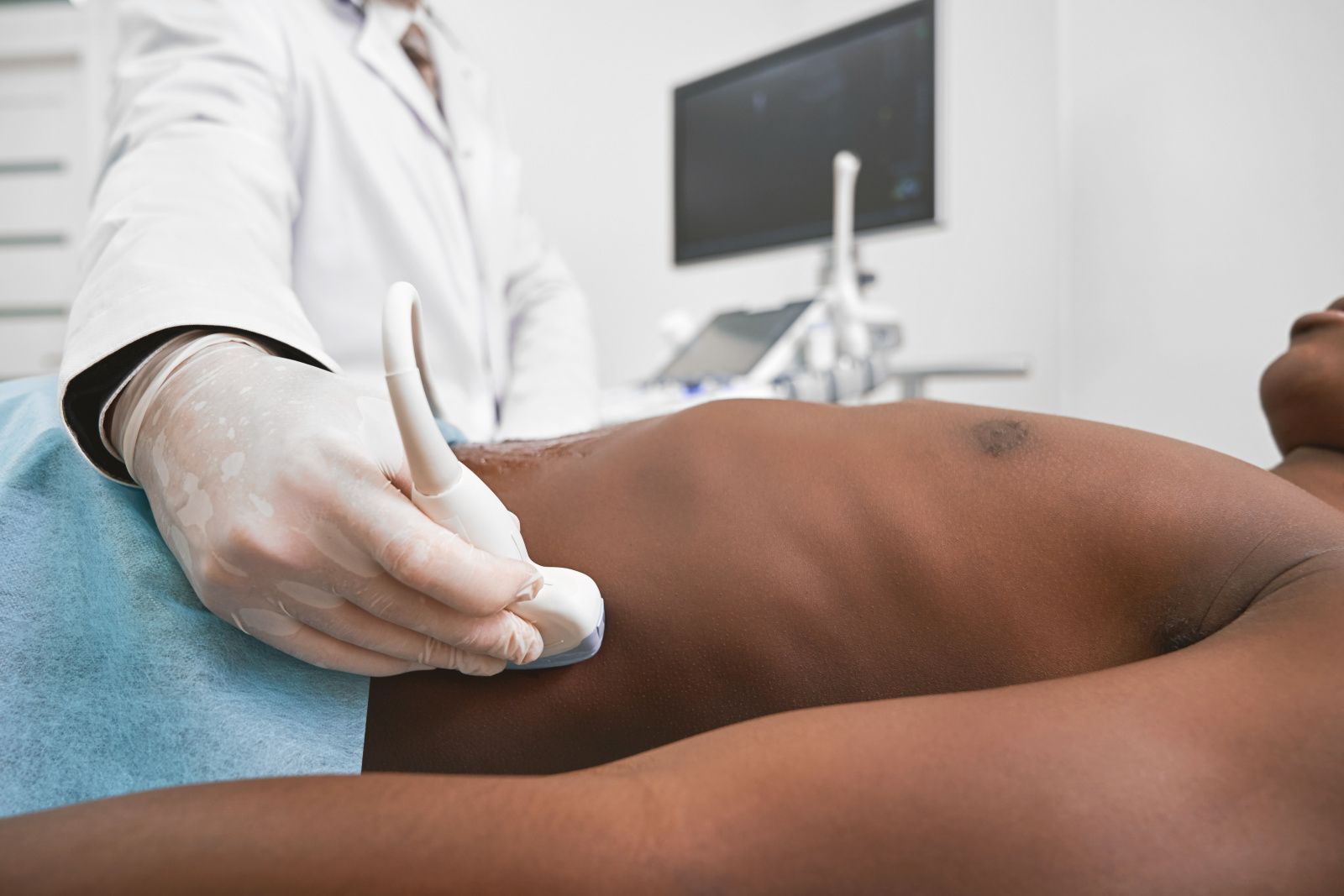
Ultrasound instead of endoscopy - patients with chronic inflammatory bowel diseases in particular benefit from the quick and simple examination. Gerhard Rogler, Director of the Clinic for Gastroenterology and Hepatology, on the advantages for patients and doctors.
Prof. Rogler, you often use ultrasound instead of endoscopy for examinations. Which patients do you use ultrasound for?
We use ultrasound instead of endoscopy for patients with chronic inflammatory bowel diseases and, for example, for patients with diverticulitis, both for acute symptoms and for long-term monitoring of the course of the disease and therapy. In certain cases, we also use ultrasound instead of computer tomography (CT).
Ultrasound has been around for a long time. Why is it only being used now?
It’s true that the technology has been around for a long time, but only the latest generation of devices provide images with a resolution high enough to replace endoscopy.
What are the advantages of ultrasound examinations for these patients compared to endoscopy or CT?
The list of benefits for these patients is long! In short, the examination is quick, simple and free of side effects. And also much cheaper.
Can you explain the advantages for patients?
Patients with chronic bowel disease often suffer several episodes of the disease per year and also frequently have diffuse abdominal pain. However, endoscopies require preparation for the examination, and patients sometimes have to wait longer for an appointment. However, it is very helpful to find out the cause of the symptoms quickly in order to clarify and provide rapid and targeted treatment. We can also use ultrasound to monitor the course of the disease and the effectiveness of a therapy very well. This also includes indications as to whether therapy should be continued or whether the patient can discontinue it. Or whether symptoms indicate a recurrence of an inflammation or have a completely different, harmless cause.
What side effects can be avoided?
A CT scan is always associated with a certain radiation exposure. For young patients in particular, it is important to keep this load low. Obtaining the same information with completely radiation-free ultrasound as with a repeated CT is of course an enormous improvement.
So there are numerous advantages for patients. And for the quality of the diagnosis?
Ultrasound has the same sensitivity and specificity as a CT or MRI in this diagnostic application. However, ultrasound also allows us to see the deeper layers of the intestine and whether they are increasingly supplied with blood – an indication of inflammation that we would not be able to detect in an endoscopy. This means that only the surface of the intestinal mucosa is visible. However, we know from studies that this heals faster than the deeper layers and that superficial appearances can therefore be deceptive.
Where do you see positive aspects for the attending physician?
We receive any number of images from the examination, which we can use for diagnosis and comparisons over a longer period of time. The devices are also mobile today. The exchange with the patients during the examination is extremely positive. This is very helpful for them and for the doctor. During a colonoscopy, the patient is usually sedated and is not aware of the examination; during a CT scan, the patient lies in the machine and the results of the examination are communicated in the written report.
During the ultrasound, patients can see what is going on in their abdomen and can also ask questions straight away. And if I see a suspicious area, I can do a palpation right away and the patient can tell me immediately if and where it hurts.
An endoscopy is still recommended for colorectal cancer screening. Why is ultrasound not used there?
In the ultrasound, the intestinal gas reflects the entire ultrasound, so that only 180° of the intestinal tube can be seen. During a colonoscopy – unlike an ultrasound – the side of the intestine facing away from the abdominal wall is also visible. Even small polyps cannot be seen with ultrasound. However, these polyps can develop into bowel cancer. Endoscopy or colonoscopy therefore offers a decisive advantage for colorectal cancer screening: the small polyps can be removed in one go during the endoscopy. Although colonoscopy is still more unpleasant than an ultrasound, it is the best option for the prevention and early detection of bowel cancer and is currently irreplaceable.