Overview: What are burns?
Burns are thermal injuries that damage the tissue through excessive direct exposure to heat. Heat damage caused by hot liquids or hot steam is referred to as scalding.
Burns – frequency and age
According to the Swiss Council for Accident Prevention (bfu), around 7,800 people in Switzerland require medical treatment for burns every year. Up to 370 of these suffer serious injuries and require treatment in a specialist burns center.
Burns: Causes and risk factors
There are several possible causes of a burn or scald. These include, for example
- open fire and flames (candle, burning clothing, other fires)
- hot water, steam, oil and other hot liquids
- Explosions caused by gas or explosives
- hot metals (e.g. irons, ovens, machines)
- Electricity (e.g. on high-voltage lines, live vehicles or machines).
- UV radiation (sunburn)
Cells can be damaged at temperatures as low as 45 degrees Celsius when heat is applied to the skin or tissue. Whether and to what extent the skin or the tissue is damaged depends on the respective temperature, but also on how long one was exposed to it.
Degree of burns & symptoms of burns
The signs of a burn or scald do not always show up immediately. Some symptoms do not become apparent until several hours after the injury. The nature and extent of symptoms depend primarily on the severity of the burn or scald.
Important to know: The severity can increase within several days of the injury if the burn or scald continues to progress in the tissue. In this case, one also speaks of “afterburning”.
- First-degree burn: In a first-degree burn, the top layer of skin (epidermis) is damaged. A painful reddening of the skin develops. In addition, the skin in the affected area may swell. It is also typical that the redness temporarily disappears when we gently press down the affected skin area with a sterile glass spatula.
- Second-degree burns: Characterized by a whitish surface, slightly rough wound edges and redness that hardly fades when pressure is applied. The wound surface is less shiny and the pain intensity is lower. Grade 2b burns usually leave scars.
Depending on the duration and intensity of heat exposure, experts distinguish between grade 2a and 2b burns in 2nd degree burns:
- Burn grade 2a: Here, closed burn blisters often appear. If these tear, an oozing wound bed becomes visible, which is reddened and sensitive to pain. The wound surface is moist and shiny. Grade 2a burns usually heal without scars.
- Burn grade 2b: In this case, the burn blisters are ruptured. Characteristic features are a whitish background, slightly rough wound edges and a redness that hardly fades on pressure. The wound surface is less shiny and the pain intensity is lower. Grade 2b burns usually leave scars.
- Third-degree burn: In a third-degree burn, the epidermis and dermis are completely destroyed. As a result, the skin is dry, thickened like leather and may be whitish to brownish in color. The pain sensors in the skin are also destroyed, which means that touch is not perceived as painful.
- 4th degree burn: At the highest level of severity, not only the deep layers of the skin are damaged, but also underlying muscles, tendons, bones and joints. The tissue is usually charred and discolored black. People with fourth-degree burns usually feel no pain locally, as the nerve fibers in the skin are damaged.
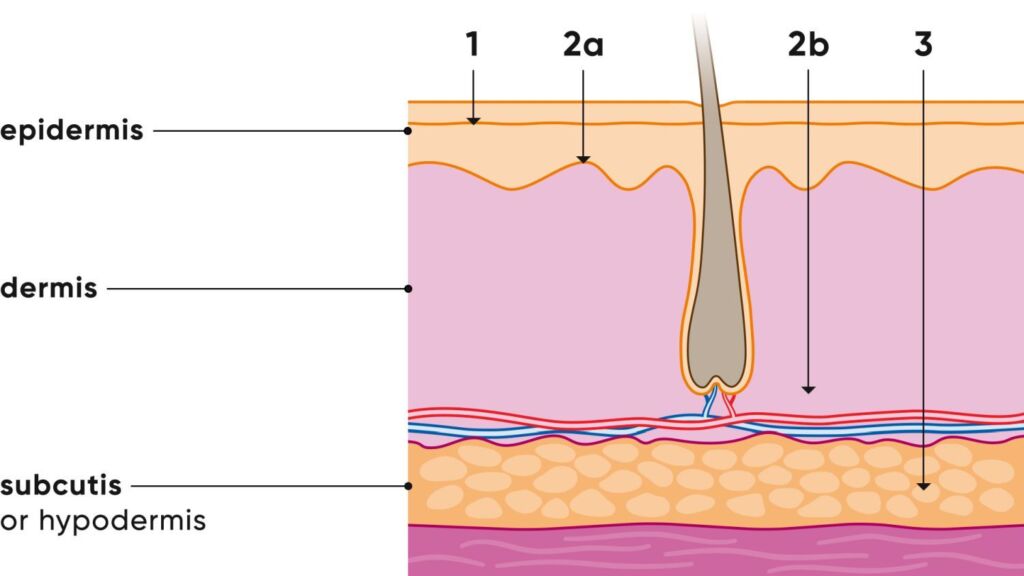
First, second and third degree burns
First aid for burns
Quick and correct first aid can have a positive effect on the course of a burn or scald and help to prevent consequential damage. The aim of the initial measures is to stop further exposure to heat, to cool the affected skin locally in the case of small-area injuries and to protect the wound from infection at all times.
End exposure to heat
The heat source should be removed first. Those affected should leave the danger zone. Hot clothing, jewelry or other objects should be removed carefully as long as they are not stuck to the skin. Firmly adhering materials must not be removed by force, as this can lead to additional tissue damage.
Cooling a burn
If there is only a small area of injury, the affected skin area can be cooled as quickly as possible with lukewarm tap water (approx. 15 to 20 °C) for about 10 to 20 minutes. Cooling can help to relieve pain and limit the progression of tissue damage.
Care should be taken not to use cold water or ice, as this can cause additional damage to the skin. In addition, only the affected part of the body should be cooled in order to avoid hypothermia. This is especially true for children.
Cover the wound
After cooling, the burn should be covered with a sterile, non-adherent dressing or a clean cloth. This protects the wound from external influences and infections.
Burn blisters should not be opened by yourself, but professionally under sterile conditions so as not to increase the risk of infection.
Important: Home remedies such as oils, ointments, flour or toothpaste should not be applied to the wound as they can further damage the skin and increase the risk of infection.
When immediate medical assistance is required
In certain cases, rapid medical treatment is required. This applies in particular if:
- larger areas of skin are affected
- face, hands, feet or the genital area are injured
- the person concerned is unconscious or has difficulty breathing
- there is a suspicion that hot smoke or steam has been inhaled
- the combustion was caused by electricity or chemical substances
In these situations, medical help should be sought immediately.
Diagnosis of burns
In the case of a burn or scald, we will first assess the burn wound to gauge the extent and severity of the injury.
To find out what type of burn you have, we will ask you about how the injury occurred. Important clues for the diagnosis are provided by your condition as well as your level of consciousness, breathing and cardiovascular function.
Assess the burnt body surface: Rule of nine
We estimate the extent of the burn based on the size of the affected area. This value is expressed as a percentage of the total body surface area. For a quick estimation of the extent of combustion, the so-called rule of nine has proven its worth. Here, the body is divided into areas, each of which accounts for about nine percent (or a multiple thereof) of the total body surface.
- Head and neck: 9 %
- Arm: 9 %
- Leg: 18 %
- Chest and abdomen: 18 %
- Back: 18 %
- Genital region: 1 %
We estimate a burn in children using a different formula. In them, the head is larger in relation to the body than in adults, but the arms and legs are relatively short.
Imaging techniques for inhalation trauma
Depending on the nature of the burn or scald, further investigation may be required. If it is suspected that the affected person has inhaled hot steam or smoke, a laboratory test and, if necessary, an endoscopy of the upper respiratory tract will be carried out to determine what is known as inhalation trauma. We use an endoscope to examine the patient’s airways for possible damage. In the case of facial burns, an ophthalmologist or an ear, nose and throat specialist is often consulted.
Burns: Prevention, early detection, prognosis
You can avoid burns or scalds in many cases by being prudent and proactive.
Be attentive with young children. This is especially true when they are learning to walk and are holding onto other things or exploring things out of curiosity. In doing so, the child can easily knock over hot drinks or knock down cooking pots. Also beware of hot oven doors. You can reduce the risk of scalds and burns by eliminating possible sources of danger or shielding them with protective grids.
Among adolescents and adults, burns from barbecue accidents are common, in addition to scalds from hot liquids or burns from cooking or baking in the oven. Therefore, make sure to handle grills properly and avoid liquid fire accelerants such as methylated spirits.
Older people, on the other hand, are more likely to suffer burns in home fires. Therefore, be careful with possible sources of fire such as candles or cigarettes. An underestimated source of danger for scalding is too hot water in the bathtub, if you cannot get out of the tub quickly enough. Therefore, before taking a bath, you should always check the temperature.
Course and healing time of burns
The course of a burn or scald depends on how badly the tissue is damaged and how much skin is affected. The age and any previous illnesses of the person concerned also play a role. For example, diabetes mellitus can make wound healing more difficult.
The prognosis for small burns and superficial injuries is generally good. These often heal without complications and without permanent damage. In contrast, a severe burn can severely affect the quality of life. This is especially true if visible scars develop, mobility is limited, or there is permanent pain. In the case of severe burns, not only medical treatment of the burns and possibly physiotherapy are important for the prognosis, but also psychological support.
Treatment of the burn depending on the extent and severity
The treatment of a burn or scald depends on whether it has just happened or happened some time ago. Thus, in the case of an acute burn or scald, fast and proper first aid is important.
Secondly, the extent and severity of the burn play an important role. More severe burns may require hospitalization and prolonged follow-up.
Details of the treatments
Frequently asked questions about burns & burn injuries
In the case of a second-degree burn, you should immediately cool the wound with lukewarm water (if the area is small, otherwise there is a risk of the body cooling down too much) and cover it with a sterile dressing. Do not open blisters yourself. As deeper layers of the skin are affected and there is a risk of infection, a medical examination should be carried out.
The most effective immediate measure is to cool the affected skin with lukewarm water for 10 to 20 minutes. This dissipates the heat from the tissue and limits the spread of the injury.
Home remedies such as oil, flour or toothpaste should not be used as they can further damage the wound.
The degree of severity can be recognized by typical characteristics:
- Grade 1: redness, pain, no blisters
- Grade 2: blistering, severe pain
- Grade 3: whitish or charred skin, often no pain
- Grade 4: deep destruction down to muscles or bones
A precise assessment should be carried out by medical professionals.
Seek medical help if:
- Bubbles develop
- large areas of skin are affected
- sensitive areas are affected (face, hands)
- Signs of infection occur
- the pain is severe or does not subside
Burns become dangerous when deeper layers of skin are affected, large areas of the body are burned or vital functions are impaired. Burns with inhalation trauma or infections are particularly dangerous.
Untreated burns can become infected, heal less well and cause permanent scars. In severe cases, life-threatening complications such as blood poisoning or circulatory failure can occur.
Yes. As the skin’s protective barrier is damaged, bacteria can enter the body and cause an infection. In severe cases, this can develop into blood poisoning (sepsis), which requires immediate medical treatment.
The risk of life-threatening complications depends not only on the amount of burnt skin, but also on the age of the person affected, the severity of the burn and possible accompanying injuries.
In adults, burns of around 20 percent of the body surface are considered potentially life-threatening. For children, older people or people with pre-existing conditions, even a lower proportion can be critical.
In addition to the affected area, the depth of the burn and possible damage to the airways are also decisive.
Severe burns can impair several vital functions of the body. One of the main causes is the loss of the skin as a natural protective barrier. This can lead to a considerable loss of fluids and infections.
In addition, burns can trigger inflammatory reactions throughout the body that impair circulation and organ function. If hot smoke or steam is inhaled, the airways can also be damaged, which impairs the body’s oxygen supply.
Thanks to modern medical care, even severe burns can often be treated successfully today, especially if specialized therapy is provided at an early stage.