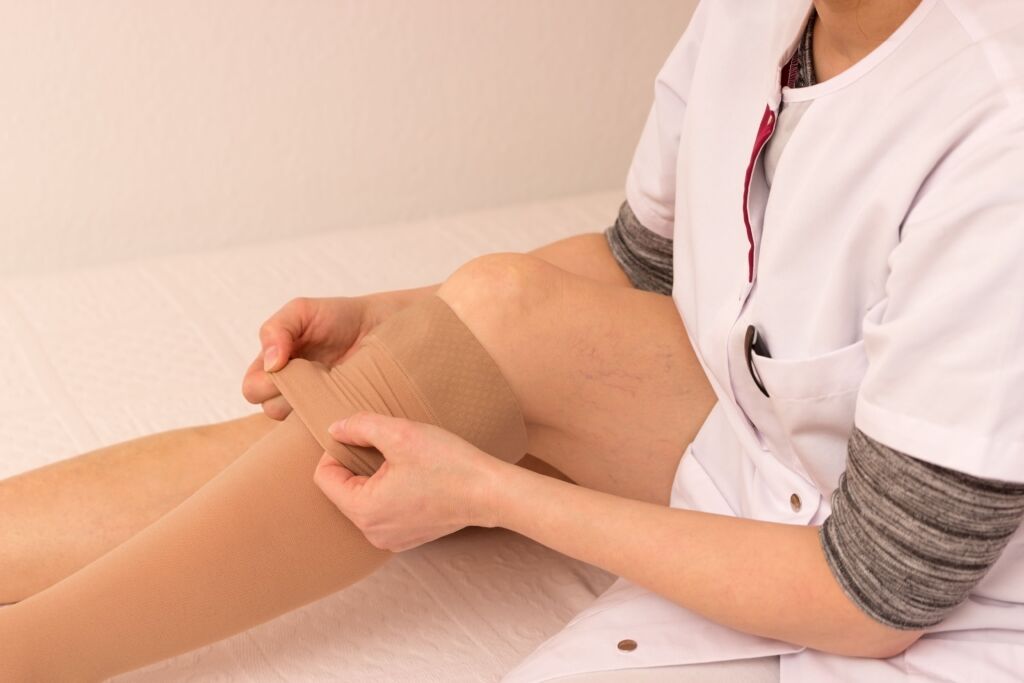
The causes of lymphedema are either congenital or acquired. cordingly, one speaks of primary or secondary lymphedema.
Primary lymphedema
Primary lymphedema, which accounts for only one to two percent of all cases, is typically associated with a malformation of the lymphatic system. In this case, there is usually a reduction in the number of lymphatic vessels or a narrowing of these, which in turn is associated with an impairment of the transport capacity of the lymph. In childhood or puberty, lymphedema is manifested by unilateral or bilateral swelling of the legs or arms.
If primary lymphedema manifests itself from birth, it is called congenital lymphedema. If primary lymphedema begins between the first and 35th year of life, it is called lymphedema praecox (premature, early lymphedema). f it does not appear until after the age of 35, we refer to it as lymphedema tardum (late lymphedema).
The distinction between the praecox and tardum forms is particularly important because differential diagnosis, especially at an older age, must take into account the blockage of lymphatic drainage by a malignant disease (cancer).
Why can consequences of a congenital anomaly perhaps only appear in old age?
It may very well be that the transport capacity and thus the function of the lymphatic vessels is restricted as a result of a malformation. However, the lymphatic vessels are still able to perform their tasks adequately in the sense of transporting the lymph away from the body. Lymphedema only develops when the transport capacity of the lymph vessels is no longer sufficient.
Secondary lymphedema
Secondary lymphedema is acquired in the course of life. The following causes are possible:
- Injuries, sprains or scars
- Surgery and radiation as part of cancer treatment
- Tumors, especially malignant lymph node diseases, such as Hodgkin’s disease or leukemia
- Inflammations of the lymph nodes
- Inflammations with parasites, bacteria, fungi or viruses