Overview: What are hemorrhoids?
Hemorrhoids are vascular cushions located at the exit of the rectum near the anus. These erectile tissues are very well supplied with blood because they are supplied by a dense network of arteries and veins. Everyone has hemorrhoids, but they only become noticeable when they are pathologically enlarged. Doctors call this clinical picture hemorrhoidal disease or symptomatic hemorrhoids. In this case, the blood accumulates in the vascular cushions and can no longer flow away unhindered. This causes various symptoms, for example itching, burning, bleeding or oozing.
Hemorrhoids have an important function in the body: together with the internal and external sphincter muscles, they seal the bowel and ensure that bowel movements can be easily controlled at all times. Sometimes these closure mechanisms also have to withstand greater stress, for example when great pressure is exerted on them when coughing, sneezing or lifting heavy loads.
Severity of enlarged hemorrhoids
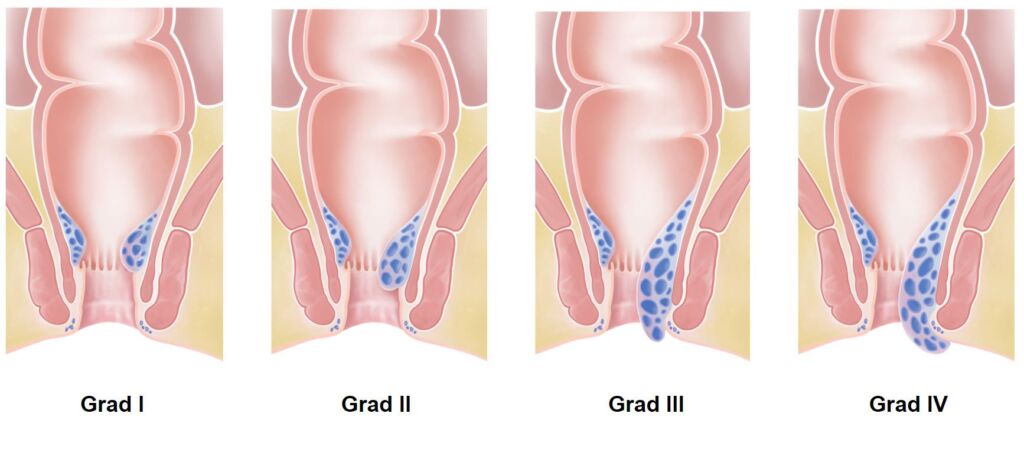
Depending on the size and severity of hemorrhoids, we divide them into different degrees of severity. There are grades one through four – from mild to severe hemorrhoidal disease.
- Grade 1: The hemorrhoids are enlarged but not visible from the outside. They usually do not yet cause any problems.
- Grade 2: The hemorrhoids are more enlarged. They may come out of the anus during bowel movements or sometimes during physical activity. However, they retreat back inside on their own.
- Grade 3: The hemorrhoids are enlarged to the point that they protrude from the anus during bowel movements and physical exertion. They will not slide back on their own, but you can push the erectile tissue back into place with the help of your fingers.
- Grade 4: The hemorrhoids are very enlarged. They emerge permanently from the anus and cannot be pushed back manually. So they are constantly visible from the outside. In most cases, a piece of the anal mucosa is also revealed. Doctors refer to this as anal prolapse.
Hemorrhoids – frequency and age
In industrialized nations, hemorrhoidal disease is one of the most common conditions. However, it is difficult to estimate exactly how many people suffer from this. This is because many people do not see a doctor for this reason, and the number of unreported cases is probably high. Medical professionals suspect that more than half of all adults over the age of 30 will develop problems with hemorrhoids during their lifetime.
Hemorrhoidal disease is most common between the ages of 45 and 65. Some studies conclude that men and women are affected about equally often. Other studies found that men are ahead in hemorrhoidal disease. During pregnancy there is often a temporary hemorrhoidal condition due to the hormone-induced weakness of the connective tissue.
Hemorrhoids: Causes and risk factors
Hemorrhoids can enlarge when there is increased pressure in the anal canal. The anal canal corresponds to the last part of the rectum, it opens into the anus. There are some risk factors that are believed to promote the development of hemorrhoids:
- Chronic constipation constipationoften due to a low-fiber diet and insufficient fluid intake
- Frequent diarrhea
- Lack of exercise and a predominantly sedentary way of working and living – bowel activity is “lamed”, which in turn promotes constipation
- Frequent lifting of heavy loads – the pressure on the abdomen increases
- Pregnancy: The unborn child presses on the abdomen and intestines, and the connective tissue also loosens due to the hormonal changes.
- Congenital connective tissue weakness
Symptoms of hemorrhoids: hemorrhoids often cause itching and burning sensation
In the beginning, hemorrhoids cause little or no discomfort. In addition, the symptoms are often very non-specific and can also occur in the context of other diseases. Even if you are uncomfortable with an ailment in this area of your body – don’t be afraid to see a doctor and get your symptoms checked out. This is especially true if there is blood in the stool.
The following signs may indicate enlarged hemorrhoids:
- Bright red blood on stool or toilet paper (grade 1) when the swollen vascular pads have been injured by hard stool and are bleeding. However, the bleeding does not cause pain. In grade 2, bleeding from the anus may increase and blood drips out.
- Itching, burning and leaking at the anus
- Foreign body or pressure sensation in the anal region – sitting becomes increasingly uncomfortable
- Feeling that the bowel is not completely emptied despite going to the toilet
- Discharge of mucus or stool in flatulence
- Severe pain in advanced hemorrhoidal disease
The symptoms usually intensify as the hemorrhoidal condition progresses. By the way, hemorrhoids should not be confused with the so-called marisci. Behind this are harmless folds of skin on the anus, which occur in many people. These can also sometimes cause symptoms, for example, when they become inflamed.
Correct clarification and therapy
Hemorrhoids affect a large part of the population during your lifetime. Often, even small measures can lead to a significant improvement in symptoms and quality of life. It is therefore worthwhile to consult a specialist in gastroenterology or proctosurgery in case of typical complaints in order to obtain a correct clarification and therapy.
Hemorrhoids: Diagnosis at the USZ
In a consultation, we always first ask about your medical history (anamnesis). For example, it is important to know exactly what symptoms you have, how long the complaints have lasted and how pronounced they are. Your lifestyle, body weight or any pregnancies also play a role. Your answers already provide us with initial clues as to whether enlarged hemorrhoids may be present.
To narrow down the cause of the complaints more precisely, we perform the following examinations:
- Digital rectal examination (DRU): This is a palpation examination with a finger – the doctor carefully palpates the rectum and detects any enlarged hemorrhoids.
- Anal canal endoscopy (proctoscopy): For this examination, we use a so-called proctoscope – a short tube with an integrated light source and lens. In this way, it is easy to see whether and how much the hemorrhoids are enlarged.
- Sometimes colonoscopy (colonoscopy) to rule out colon cancer in the rectum or colon. If there is blood in the stool, we usually also perform a complete colonoscopy to gain certainty.
Whether treatment of hemorrhoids is necessary and which therapy can be considered depends on the extent of the hemorrhoidal condition.
Hemorrhoids: Prevention, early detection, prognosis
The fact that hemorrhoids enlarge in the course of life or in special situations, such as pregnancy, can usually not be prevented. So, you cannot prevent hemorrhoidal disease one hundred percent. Nevertheless, there are some risk factors that promote enlarged vascular cushions. And you have a partial influence on these yourself, because they are rooted in lifestyle.
Prevention tips
Diet: Consume enough fiber, which is good for digestion and prevents constipation. Whole grain products, fruit, vegetables or legumes (peas, lentils, beans) are particularly rich in fiber.
Hydration: Drink at least 1.5 to 2 liters a day, more on hot days. Low-calorie drinks such as water, unsweetened tea or fruit juice are recommended. In this way, you also ensure a soft bowel movement.
Regular bowel movements: don’t delay having a bowel movement when you need to go to the bathroom, go right away. Not everyone has a bowel movement every day. Lower frequencies of two to three times a week are also normal and are not considered constipation. And, don’t push too hard during bowel movements.
Exercise and sport: Move as much as possible in your daily life and avoid sitting for long periods. Go for a walk, climb stairs or ride your bike to the grocery store. Every kind of movement counts. Regular exercise also gets your bowels moving and aids digestion. Good are hiking, swimming or cycling. But pelvic floor exercises can also prevent enlarged hemorrhoids.
Healthy Weight: Try to maintain or achieve a normal weight. Overweight and obesity are detrimental to health and can also promote enlarged hemorrhoids. If you are overweight: Try to lose a few kilos, preferably through a healthy, balanced diet and exercise.
Course and prognosis of enlarged hemorrhoids
Once enlarged, hemorrhoids do not shrink again on their own. Nevertheless, the course of hemorrhoidal disease cannot be generally predicted. In some, the process stops, but sometimes the hemorrhoids enlarge and the symptoms increase. This can lead to other consequences – from skin irritation to anal eczema.
The prognosis for hemorrhoids is usually good if we treat them adequately. This is best done when the condition is not too far advanced. Sometimes, however, hemorrhoidal disease flares up again and the symptoms return.
Complications with hemorrhoids – these are possible
With advanced hemorrhoids, the possibility of complications increases. The following complications are possible with hemorrhoidal disease:
- Anal eczema: oozing skin lesions and ulcers form.
- Anal fissure: An anal fissure can occur when hemorrhoids become sore from using toilet paper. Then cracks form in the anal mucosa, which is also very painful.
- Anal abscesses: In addition, the wounds can become infected with bacteria from the stool – suppurating abscesses can be the result.
- Anal fistulas: They can arise from an anal fissure. Fistulas are unnatural connections that extend from the bowel to the surface of the skin and do not belong there.
- Anal vein thrombosis: The erectile tissue becomes trapped and blood clots may form. These are recognizable as a blue-black, bulging lump next to the anus. Such a blood clot is also called anal thrombosis or perianal thrombosis. Many also refer to them as “external hemorrhoids,” which is not entirely accurate. Thrombosis in this sensitive area causes significant pain, often making sitting impossible. Anal venous thrombosis usually heals on its own, in the early stages excision (= cutting out) under local anesthesia can promptly help and accelerate healing You can relieve the pain with sitz baths or painkillers.
- Anemia, when hemorrhoids bleed constantly and profusely.
Although these complications are not life-threatening, they are extremely unpleasant and often associated with great pain. They can often be avoided if you have enlarged hemorrhoids treated in time, before they reach stage 4.
Hemorrhoids: Self-treatment and therapy
Hemorrhoids that are not yet so pronounced, you may be able to treat yourself at first. However, the enlarged vascular cushions cannot be “shrunk” again in this way. In the case of advanced stage hemorrhoidal disease, a visit to the doctor’s office is always advisable. This is especially true if you discover blood in your stool. A possible contact person is the family doctor or a specialist for the rectum, a proctologist. Treatment depends on the extent of hemorrhoidal disease and symptoms.