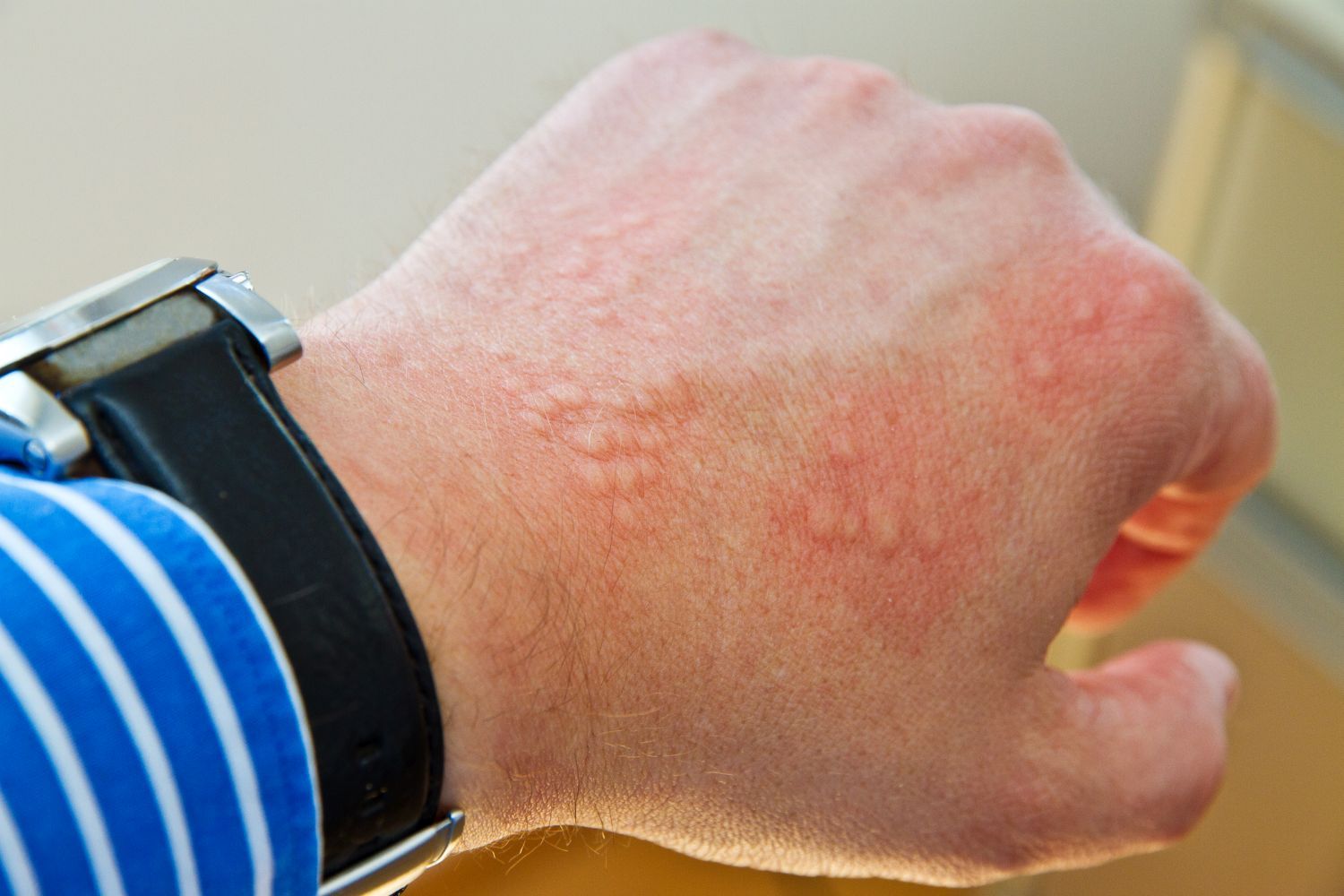
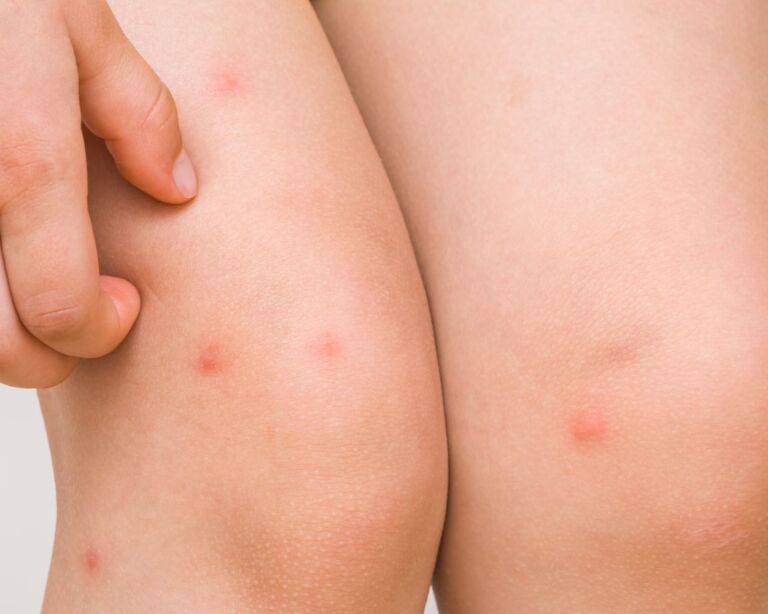
What is hives
Hives is the generic term for certain skin conditions. Typically, you get a rash that appears in the form of itchy wheals. It can be localized or extend over larger areas or the whole body. Their skin changes are reminiscent of symptoms that appear after contact with a stinging nettle (Latin: urtica = nettle). In some cases, so-called angioedema, extensive swelling of the subcutaneous tissue and certain areas of the mucous membrane, also develops. It is estimated that about one in four people will temporarily develop hives once in their lifetime. The rash is not contagious and is not life-threatening, but it can significantly impair your quality of life – on the one hand due to the visible skin changes and on the other hand due to the severe itching usually associated with it. This sometimes causes other people to keep their distance. All these factors can also affect your psyche.
A variety of factors can influence or trigger urticaria, which is why the search for the cause is often challenging. In the more common chronic spontaneous form, however, there is usually no clear trigger.
Acute and chronic hives – characteristics & duration
Generally, we distinguish between two courses of hives based on duration:
- Acute: If the disease lasts up to six weeks, we speak of acute hives.
- Chronic: Chronic hives persist for more than six weeks. If the urticaria is chronic, we distinguish between different forms of progression:
- In chronic continuous urticaria , they experience daily flare-ups with wheals and itching.
- In chronic recurrent urticaria , episodes of the disease alternate with symptom-free phases. Both the relapses and the symptom-free phases can last for weeks or months.
In the majority of chronic courses, chronic spontaneous urticaria is present without a detectable trigger; chronic inducible forms with clear triggers (e.g. cold or pressure) are less common.
Causes of nettle rash
Research into the causes of hives (urticaria) is very complex. In many cases, no specific trigger can be identified.
Even if the development of hives is very complex, all forms have one thing in common: certain immune cells (so-called mast cells) release inflammation-promoting messenger substances, including mainly histamine and other mediators such as leukotrienes and prostaglandins. The messenger substances stimulate immune cells in your skin and cells responsible for sensory perception. Typically, they become active when attackers such as parasites or hostile bacteria besiege the body. Histamine and other signaling substances give the starting signal for a localized or widespread inflammation of your skin. It swells, reddens, itches and forms wheals. For example, an allergic reaction, such as to pollen or food, can activate mast cells. However, there are many other factors that can stimulate mast cells. In the majority of cases, the cause remains unclear and is then referred to as idiopathic urticaria.
Hives forms
Various factors can cause hives to break out and the typical rash to develop. The three main forms include:
- Spontaneous urticaria: Symptoms appear spontaneously, with no apparent external trigger.
- Physical urticaria: External stimuli such as cold, heat or pressure trigger the skin changes.
- Other forms of urticaria: Factors such as exertion, contact with water, or allergies provoke the hives.
Spontaneous urticaria
In spontaneous urticaria, wheals or angioedema form spontaneously, “out of the blue”.
We distinguish two forms here:
Spontaneous acute urticaria, the symptoms of which subside after six weeks at the latest. Triggers include infections, sometimes in combination with painkillers. Genuine immediate allergic reactions, for example to insect stings from bees or wasps, food or medication, can also occur with acute urticaria and may then be associated with dangerous symptoms such as asthma or circulatory collapse; these symptoms then manifest themselves quickly, practically always within the first hour after contact with the allergy. If acute urticaria manifests itself for the first time and proceeds without accompanying symptoms, further clarification is not absolutely necessary.
Spontaneous chronic urticaria with symptoms lasting longer than six weeks. In the majority of cases, the cause remains unclear or is autoimmune mediated. Genuine food or additive triggers are rare.
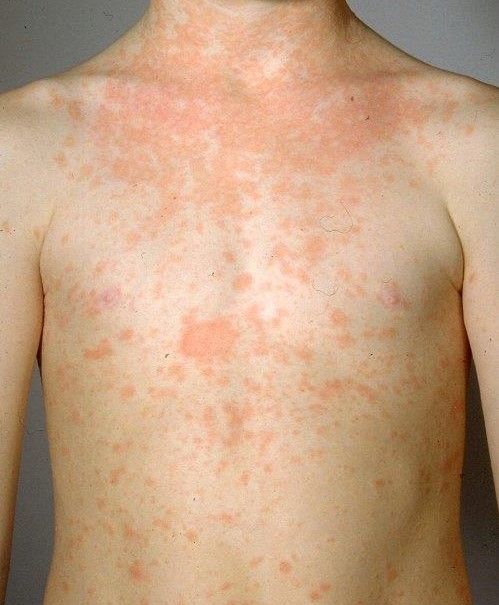
Physical urticaria
Pressure, temperature or other physical stimuli trigger physical urticaria. Their symptoms are usually confined to the area where the stimulus occurred. Sometimes, however, it spreads over a larger area.
There are several triggers of physical hives. These include:
Mechanical stimuli: urticaria factitia, pressure urticaria, vibration urticaria
When mechanical stimuli act on your skin, hives may also break out.
The most common form is urticaria factitia, or skin pruritus. The rash is caused by shear forces, such as when fabric scratches, rubs or rubs. Then, within minutes, the typical wheals form and the skin itches. The rash persists between two and eight hours. In the case of the special form Urticaria factitia tarda, the characteristic rash appears with a delay of at least 30 minutes to a maximum of four hours after the irritation. Pressure urticaria, in which prolonged pressure acts on the skin (e.g. tight belts, rucksack straps or heavy carrying), also occurs with a time delay of four to eight hours. If hives develop as a result of vibration, for example when you work with a percussion drill, it is vibratory urticaria.
Why the mast cells in your skin release an increased amount of the messenger substance histamine has not yet been conclusively clarified. The mechanical stimulus is the trigger, but the actual causes usually remain obscure. In most cases, no additional underlying disease can be detected. Other causes are only discussed in individual cases.
Temperature stimuli: cold urticaria, heat urticaria, light urticaria
Cold urticaria occurs when you have contact with cold water, ice, or cold metals. The symptoms can be localized or widespread.
This form of hives resulting from exposure to cold, such as after jumping into ice-cold water, can be life-threatening. In rare cases of cold urticaria, rapid exposure to cold can trigger a generalized reaction up to anaphylaxis (anaphylactic shock), i.e. an excessive reaction of the immune system.
In most cases, cold urticaria has no underlying other disease. In individual cases, for example, infections or chronic inflammations are identified as triggers; however, this is rather the exception.
Heat urticaria, in turn, is the result of exposure to heat. There is also light urticaria. Both natural daylight and UVA radiation, for example in a solarium or from a halogen lamp, can trigger light urticaria.
Other forms of urticaria
The following factors can also trigger hives:
- Cholinergic urticaria: This is also known as sweat urticaria because it occurs when, for example, a hot bath, sport, excitement or hot spices increase the body’s core temperature. It appears as an extensive skin rash with a large number of small, separate wheals.
- Aquagene Urtikaria: Maximal 30 Minuten nach längerem Kontakt mit Wasser bilden sich stecknadelkopfgrosse gerötete Quaddeln, vor allem am Oberkörper, seltener an den Beinen und im Gesicht.
- Contact urticaria: The typical wheals develop after contact with certain substances, for example formaldehyde, natural latex, spurge.
- Exercise-induced urticaria: It occurs after physical exertion.
Medical checkup – more information
Send a photo of the affected skin area and fill out the short questionnaire. Within 24 hours on weekdays, you will receive a reliable diagnosis from our experts. Your data will be transmitted to us encrypted and treated confidentially.
Hives symptoms
You can recognize hives by the following typical symptoms:
- Urticaria begins with severe itching of the skin, rarely it also burns. Usually, you are more likely to feel the need to rub or squeeze the affected skin area. With other itchy skin conditions, such as eczema, sufferers are more likely to want to scratch.
- Then you get a skin rash in the form of small wheals, reminiscent of the skin change after contact with a nettle. The rash is clearly distinguishable from unaffected areas of the skin. It can appear limited, but can also extend over larger areas. The wheals often regress after minutes, or a few hours, usually after 24 hours at the most. However, they often form again afterwards and reappear at new locations at best.
- Sometimes the so-called angioedema occurs in the context of acute hives. This is a cushion-like, elastic swelling of the tissues under the skin or mucous membranes because aqueous fluid accumulates there. Angioedema often develops on the face, hands, feet and genitals. In the area of the mucous membranes, the larynx or tongue may swell. It can become life-threatening if swelling obstructs breathing. Sometimes pain or itching accompanies the swelling, which usually lasts up to 72 hours. Angioedema indicates a hypersensitivity reaction of the body.
- In rare cases, angioedema also occurs without accompanying urticaria; in these cases, hypersensitivity to certain drugs (especially blood pressure drugs, so-called ACE inhibitors) or rare inherited disorders of the coagulation system(hereditary angioedema, HAE) must also be considered.
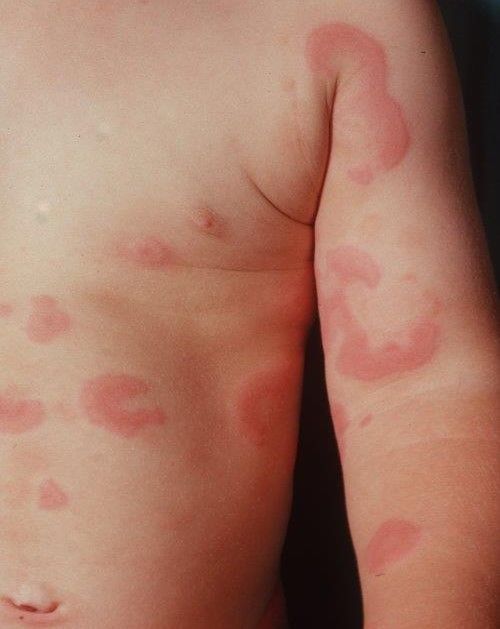
Hives: Emergency anaphylactic shock
If you suffer from an allergy and suddenly develop symptoms of hives, in rare cases this can lead to anaphylaxis. If you are allergic to bee venom, for example, you may experience symptoms of urticaria after a sting, with itching, wheals and swelling, and even allergic shock.
The following symptoms characterize anaphylaxis:
- Your blood pressure drops, you suffer circulatory weakness and even unconsciousness.
- You feel unwell, vomit, get diarrhea.
- You get anxious.
- Your bronchial muscles tense up, which is why you experience shortness of breath.
- Your heart races.
If left untreated, the combination of symptoms can lead to cardiovascular and respiratory arrest.
Emergency anaphylactic shock
In the event of an allergic shock (anaphylaxis), you must act immediately: Call the emergency services(144). If available, administer the emergency medication (adrenaline auto-injector) into the outer thigh.
Hives diagnosis
Because of the typical rash, the diagnosis of hives is usually not difficult for us. It is more complex to track down the actual cause of urticaria.
First, we will ask about the patient’s medical history (anamnesis). For example, we will ask you:
- How long have you been suffering from hives?
- How long and how often has the rash occurred so far?
- Did he change during the day?
- Have you ever been treated for urticaria before?
- Has tissue swelling (angioedema) occurred, for example on the face, hands and feet or in the genital area?
- Is there an intolerance to certain foods or medications?
- Could certain physical stimuli have triggered the rash, e.g. cold, heat or pressure?
Acute urticaria does not usually require extensive diagnostics, as the symptoms usually subside on their own. In the case of chronic hives, on the other hand, a targeted search for the causes should be carried out, whereby a basic diagnosis consisting of blood count, CRP/BSG and thyroid values is useful. Despite these investigations, in most cases no specific trigger is found for the more common chronic spontaneous urticaria.
Finding the cause of chronic hives
It can be helpful for people with chronic urticaria to keep an urticaria diary. In it, you record when the symptoms appear, what you ate, drank, what medications you took, and how you acted.
Possible laboratory tests for chronic hives include:
- a blood test to determine possible inflammation levels and to get an indication of possible infections,
- In selected cases, further examinations if the medical history provides concrete indications of additional illnesses.
If there is a suspicion that you are developing the symptomatology of hives due to physical stimuli such as heat, cold or pressure, we can specifically expose you to these stimuli in tests.
Often, several factors are responsible for the onset of hives. In most cases, the cause cannot be identified despite extensive testing. Especially in the chronic spontaneous form, it must be accepted that a specific trigger can often not be found.
Hives (Urticaria): Prevention, Early Detection, Prognosis
You can not prevent the skin disease. Since the symptoms usually occur abruptly, early detection is not possible. The symptoms of acute urticaria usually only last a few days, at most a few weeks. If you are lucky, they will never occur again.
Chronic hives persist for years, sometimes decades, in rare cases. Then the usual symptoms occur daily, weekly or less frequently. In many patients, however, the disease improves over time, even if no trigger is found.
Hives treatment
The treatment of hives depends on the cause and the course of the disease. Acute hives usually subside on their own within a short time. If necessary, antihistamines can inhibit the release of histamine and thus quickly relieve itching and wheals.
There are two types of chronic urticaria. In the more common form, so-called chronic spontaneous urticaria, no clear trigger can be identified. It occurs “out of the blue”, so to speak, and in many cases is due to a malfunction of the body’s immune response. The focus here is on drug therapy, usually initially with modern antihistamines. If these are not sufficient in normal dosage, the dose can be significantly increased. If symptoms persist, very effective modern therapies such as omalizumab are now available; in rare, persistent cases, other medications may be considered. Cortisone preparations are only used for a short time and in special situations.
The second form is chronic inducible urticaria. There is a clear trigger here, for example pressure on the skin, cold or heat, physical strain, water or sunlight. In this case, it is important to avoid or adapt these triggers as far as possible. Antihistamines can also be used here, and in certain subtypes the disease also responds well to modern therapies such as omalizumab.
As hives can take very different courses, their treatment often requires patience and good cooperation between the patient and the medical team. At the USZ, we look after you with specially trained specialists in dermatology and allergology and tailor the treatment to your personal situation.
FAQ on the topic of hives
Hives can be triggered by many factors. In the majority of cases, however, no trigger can be identified, especially in the chronic spontaneous form. Common triggers of acute hives are infections, rarely also allergic reactions to food, medication or insect bites. In certain chronic inducible forms, cold, heat or pressure play a role as triggers, but these are rarer than chronic spontaneous urticaria without a recognizable trigger.
Acute hives can occur as part of or after infections, for example due to cold viruses, Epstein-Barr virus, hepatitis viruses or bacterial infections of the respiratory tract. This is particularly common in children. The skin reaction is caused by an excess immune response, not by the virus itself.
Sudden hives occur when mast cells in the skin release histamine – for example after contact with an allergen, an infection or a physical stimulus. Stress or certain medications can also trigger this process. The exact cause often remains unclear, especially in the chronic spontaneous form.
Yes, psychological or physical stress can promote the release of histamine and increase symptoms. Stress management can therefore help.
Acute hives usually only last a few hours to days, sometimes up to six weeks. If the wheals do not subside afterwards, this is referred to as chronic hives. This can last for months or years and requires targeted clarification and treatment.
A direct deficiency as a cause is rare. Studies show that a lack of vitamin D or iron can influence the course of chronic hives without being the sole cause. However, a balanced diet supports the immune system and can have a positive influence on the course of the disease. A typical “hives deficiency”, which would regularly be found as a cause, is not known.
Hives mainly affect the skin, more specifically the mast cells in the upper and middle layer of the skin. These cells release histamine, which causes wheals, redness and itching. Internal organs are not usually affected – except in the case of severe allergic reactions with angioedema.
Trigger avoidance is particularly important for chronically inducible forms. In the more common chronic spontaneous urticaria, on the other hand, the focus is on consistent drug treatment, as a trigger cannot usually be identified with certainty.
In children, urticaria is usually acute and harmless. Cooling compresses, antipruritic lotions or antihistamines can alleviate the symptoms. If shortness of breath, swelling of the face or circulatory problems occur, immediate medical attention is required as this may indicate an allergic reaction.
The treatment depends on the cause. Antihistamines are usually used to relieve itching and wheals. For chronic hives, additional medication such as omalizumab (anti-IgE antibodies) may be necessary. It is important to identify and reduce possible triggers in chronically inducible forms. In most cases of chronic spontaneous urticaria, on the other hand, the focus is on individually tailored drug therapy, even if no trigger is found.