What is psoriasis?
Psoriasis is one of the most common inflammatory diseases of the skin. It usually progresses in episodes. Typical signs are reddened, scaly patches that are sharply demarcated from healthy skin and are often very itchy. They occur mainly on certain parts of the body such as the elbows, knees or the hairy area of the head. Sometimes the spots can also spread or merge. In some patients, nails, lymph nodes or joints are also affected by psoriasis.
Psoriasis is caused by an autoimmune reaction of the skin. Scientists have not yet been able to fully clarify the exact trigger for this misdirected immune response. In addition to a hereditary predisposition, infections, stress, geography or other factors also play a role in the onset of psoriasis. The disease is not contagious. There are also other factors that can trigger psoriasis: Obesity, smoking, medication, irritation of the skin.
Psoriasis – frequency and age
In Switzerland, around one to two percent of the population suffer from psoriasis. In most cases, it is a so-called common psoriasis (psoriasis vulgaris). Medical experts distinguish between the early type (type 1) and the late type (type 2). Type 1 psoriasis mainly affects younger people under the age of 40. Type 2 usually only becomes apparent after the age of 40.
Psoriasis: causes and risk factors
The cause of the typical skin reactions in psoriasis is a disturbed immune response in the body. The keratinocytes, the skin cells that form the cornea, are particularly affected. They are constantly formed in the lower layers of the skin, migrate from there to the epidermis and are then shed. This whole process usually takes up to a month. In psoriasis, the misdirected immune response leads to an inflammatory reaction and the keratinocytes multiply much faster than normal. This leads to an excessive formation of skin cells. The affected areas become thick and flaky.
Hereditary predisposition plays a major role in the development of psoriasis. Children whose parents suffer from the skin disease fall ill much more frequently than children of healthy parents. But not everyone who has a family history of psoriasis automatically develops it. In most cases, other factors are necessary that can contribute to the onset of the disease or promote a flare-up. These include, for example:
- psychological stress (for example due to the death of a loved one, divorce, unemployment or similar),
- Medication (such as non-steroidal anti-inflammatory drugs, beta blockers, antimalarials, glucocorticoids, antibiotics, etc.),
- Nicotine and alcohol,
- Infections (especially with streptococci) and
- Irritation of the skin (e.g. due to sunburn, injuries, etc.).
Symptoms: How you can recognize psoriasis
There are several signs that indicate psoriasis. Most of them relate to the skin. However, there are less frequent changes to the nails and joints.
Typical skin changes in psoriasis
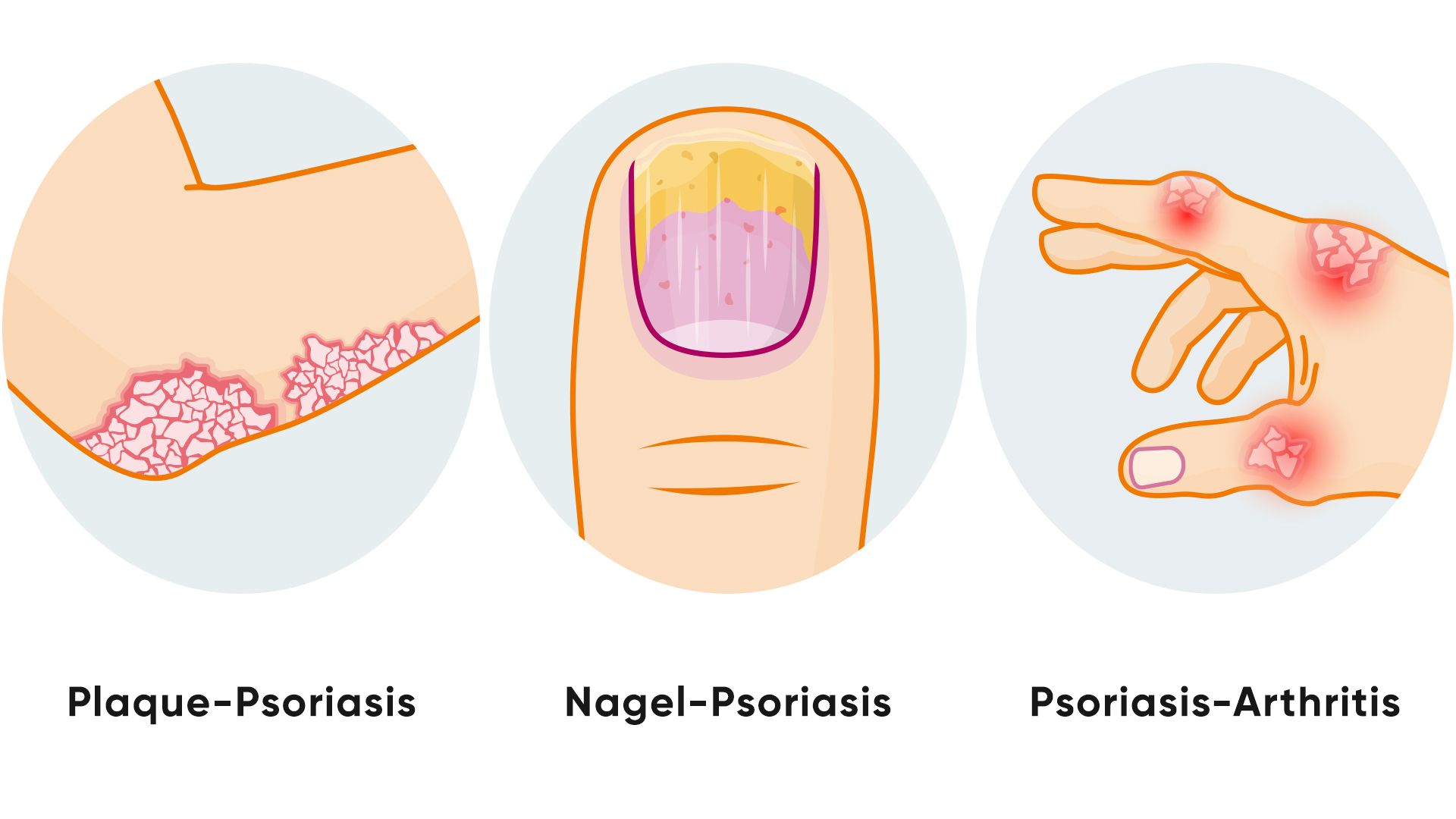
Most of those affected (80 to 90 percent) suffer from so-called psoriasis vulgaris or plaque psoriasis. Typical signs are usually sharply defined, reddened and slightly raised patches, so-called plaques. They are usually covered with silvery-white scales. If you rub off the scales and the so-called last cuticle underneath, a punctiform hemorrhage occurs. The plaques can vary in size and can be very itchy. They mainly appear on heavily stressed areas of the skin (such as elbows, knees, sacrum, hairy head).
However, the skin changes typical of psoriasis can also occur in other areas of the body, such as in the folds of the buttocks, in the armpit or on the hands and feet. Sometimes the plaques spread over the entire body. In this case it is a so-called psoriatic erythroderma.
Very rarely, blisters filled with pus may form on the reddened areas of skin. In severe cases, the whole body is affected. Pustular psoriasis develops mainly after an infection with bacteria.
Nail changes in psoriasis
Psoriasis can also cause changes to the nails (nail psoriasis). Typical are, for example, dents that are about the size of a pinhead (so-called spotted nails). However, yellowish discoloration or fine, brownish longitudinal stripes are also possible. The nail can also peel off or crumble (crumbling nail).
Joint problems with psoriasis
In around 20 percent of sufferers, psoriasis also manifests itself in the joints. Medical professionals then speak of psoriatic arthritis. In most cases, the finger or toe joints become inflamed, swollen, stiff and painful (peripheral type). Sometimes the joints between the sacrum and ilium (sacroiliac joints) or the spine (axial type) are also affected. The underlying inflammation can lead to permanent damage to the joints involved.
Psoriasis: Diagnosis by the doctor
The typical skin symptoms are usually a clear indication that you are suffering from psoriasis. To confirm the suspicion, we can carefully remove the scales from one of the affected skin areas. The thin, shiny skin underneath can also be easily removed. This usually results in small, pinpoint hemorrhages, known in technical jargon as the “spotting phenomenon”.
In addition to the skin, we will also examine your nails for characteristic features such as discoloration or brittleness. To rule out other diseases such as nail fungus, we can take a sample of the nail and examine it more closely. You will also be asked various questions during the examination. For example:
- How long have the symptoms been present?
- Do you have a family history of psoriasis?
- Do you have additional complaints such as joint problems?
Medical checkup – more information
Send a photo of the affected skin area and fill out the short questionnaire. Within 24 hours on weekdays, you will receive a reliable diagnosis from our experts. Your data will be transmitted to us encrypted and treated confidentially.
Diagnosing psoriasis - what doctors do next
Sometimes the symptoms of psoriasis are only very mild. This can make a clear diagnosis difficult. If the diagnosis is unclear, we will perform a so-called biopsy. A small skin sample is taken from the affected area, which is then examined under a microscope. This allows other diseases (such as fungal infections, eczema, lichen or syphilis) that cause similar symptoms on the skin to be ruled out.
Once the diagnosis of psoriasis has been confirmed, an attempt is made to assess the severity of the disease. This is important in order to choose the right therapy afterwards. Various factors play a role in the severity of psoriasis, such as where the skin changes occur, how large the affected area of skin is, whether there are other symptoms or how much the psoriasis affects the sufferer’s everyday life.
Psoriasis: prevention, early detection, prognosis
What actually triggers psoriasis is still not fully understood. In addition to a hereditary predisposition, various other risk factors can also play a role. There are therefore no measures you can take to directly prevent psoriasis. However, if there are already cases of psoriasis in your family, you can try to avoid risk factors such as stress, alcohol or nicotine. As there are no methods for the early detection of psoriasis, you should also have any skin problems that arise clarified as quickly as possible – especially if one of your family members already suffers from psoriasis.
Progression and prognosis of psoriasis
Psoriasis is a chronic disease and usually progresses in relapses. This means that phases in which the symptoms are more severe alternate with phases in which the symptoms are less severe or sometimes do not occur at all. It is also typical that the disease develops differently in each affected person. The course of the disease is therefore difficult to predict. This is a problem for many sufferers. In addition, many sufferers are ashamed to show their skin changes. Some therefore withdraw and avoid contact with other people. Psoriasis can therefore also lead to psychological problems such as depression. In addition, people with psoriasis are often very overweight and also suffer from high blood pressure, cardiovascular disease or diabetes.
Psoriasis – what you can do yourself
Even though psoriasis is currently incurable, you can usually get the disease under control with the right therapy. This is especially true if the joints are affected by the inflammation. The earlier the treatment takes place, the better you protect your joints from possible permanent damage.
You can also take various measures yourself to prevent or delay the onset of flare-ups:
- Find out what makes your symptoms worse. A diary can help with this.
- Make sure you take good care of your skin.
- Make sure you lead a healthy lifestyle. This means: little alcohol, no cigarettes, sufficient exercise and a healthy diet.
- If you are overweight, try to lose the extra pounds. This can keep possible concomitant diseases such as diabetes or high blood pressure in check.
- Stress can promote the occurrence of relapses. So make sure you relax sufficiently.
- Do not shy away from seeking psychological support. This can not only improve your quality of life, but also have a positive influence on the course of the disease.
Psoriasis: treatment in several steps
Various options are available for the treatment of psoriasis. Depending on the severity of your illness, we will decide which measures are appropriate. Even though the disease is not yet curable, it can be controlled well in most cases with the right treatment.



