J Natl Cancer Inst.
Breuer E, Hebeisen M, Schneider MA, Roth L, Pauli C, Frischer-Ordu K, Eden J, Pache B, Steffen T, Hübner M, Villeneuve L, Kepenekian V, Passot G, Gertsch P, Gupta A, Glehen O, Lehmann K. *CCCZ Members in bold
Abstract
Background: Multimodal treatment, including systemic treatment and surgery, improved the prognosis of peritoneal metastasis (PM). Despite all efforts, recurrence rates remain high, and little data are available about clinical behavior or molecular patterns of PM in comparison to hematogenous metastasis. Here, we aimed to analyze recurrence patterns after multimodal treatment for PM from colorectal cancer.
Methods: Patients with colorectal PM undergoing multimodal treatment including systemic chemotherapy and cytoreductive surgery plus hyperthermic intraperitoneal chemotherapy (CRS/HIPEC) between 2005 and 2017 at 4 centers were analyzed retrospectively.
Results: A total of 505 patients undergoing CRS/HIPEC were analyzed. Of the patients, 82.1% received preoperative chemotherapy. Median peritoneal cancer index was 6 (interquartile range = 3-11). Median disease-free and overall survival was 12 (95% confidence interval [CI] = 11 to 14) months and 51 (95% CI = 43 to 62) months, respectively. Disease recurred in 361 (71.5%) patients, presenting as isolated peritoneal recurrence in 24.6%, isolated hematogenous recurrence in 28.3%, and mixed recurrence in 13.9% of patients. Recurrence to the peritoneum was associated with an impaired time from recurrence to death of 21 (95% CI = 18 to 31) months for isolated peritoneal and 22 (95% CI = 16 to 30) months for mixed recurrence, compared with 43 (95% CI = 31 to >121) months for hematogenous recurrence (hazard ratio [HR] = 1.79, 95% CI = 1.27 to 2.53; P = .001; and HR = 2.44, 95% CI = 1.61 to 3.79; P < .001). On multiple logistic regression analysis, RAS mutational status (odds ratio [OR] = 2.42, 95% CI = 1.11 to 5.47; P = .03) and positive nodal stage of the primary (OR = 3.88, 95% CI = 1.40 to 11.86; P = .01) were identified as predictive factors for peritoneal recurrence.
Conclusions: This study highlights the heterogeneity of peritoneal metastasis in patients with colorectal cancer. Recurrent peritoneal metastasis after radical treatment represents a more aggressive subset of metastatic colorectal cancer.
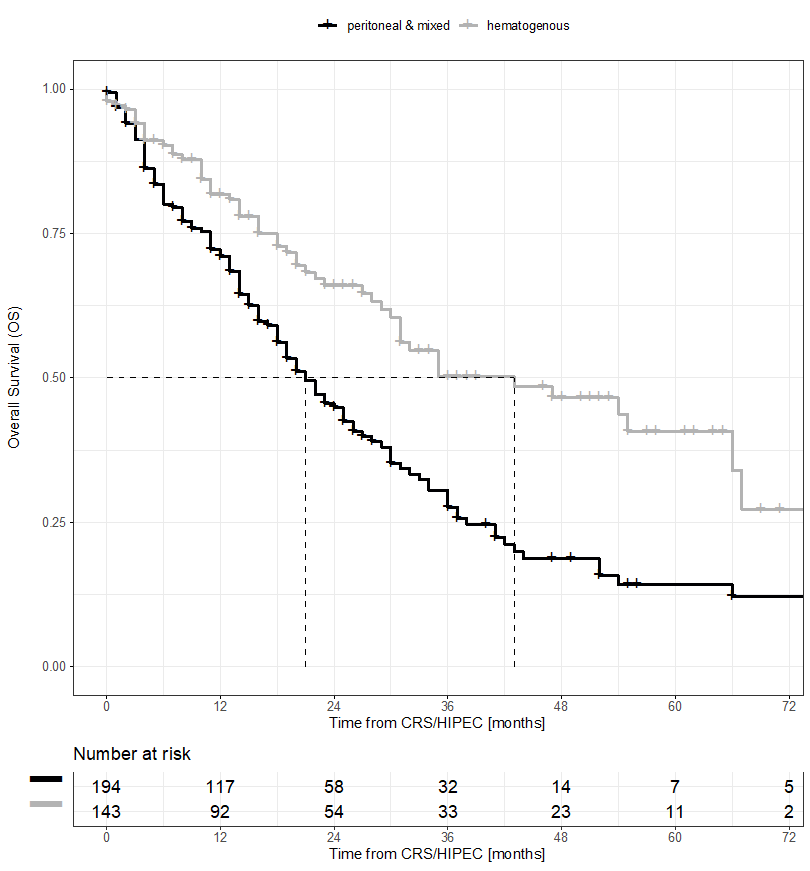
Patients with hematogenous recurrence have a better survival compared to patients with peritoneal metastasis (43 vs. 35 month). Risk factors for peritoneal metastasis were RAS mutational status (OR 2.42, p=0.03) and a positive nodal stage of the primary (OR 3.88, p=0.01)
J Natl Cancer Inst. 2021 Aug 2;113(8):1027-1035.
doi: 10.1093/jnci/djab001

