Various heart diseases can lead to heart failure. In addition to treating the underlying heart disease, there are now very good treatment options for heart failure itself. In addition to a well-coordinated combination drug therapy, these also include so-called device-based therapies. Selected patients benefit from specialized pacemakers (cardiac resynchronization) with or without defibrillator function to protect against sudden cardiac death. In the final stages of the disease, there is also the possibility of so-called mechanical circulatory support, either as a short-term bridging measure until recovery or as a permanent therapy with a good quality of life, possibly until a heart transplant. The decisive factor is that comprehensive care with individually tailored therapy can significantly improve the quality of life and prognosis of heart failure.
Heart failure
Heart failure
Heart failure (cardiac insufficiency) is a serious condition. As the disease progresses, the supply of blood and oxygen to the body may be reduced. This can lead to various symptoms that can affect the quality of life. In the last 20 years, treatment options have developed rapidly which can significantly improve quality of life and life expectancy.
Overview: What is heart failure?
Various heart diseases can lead to heart failure. With increasing heart failure, the heart muscle can become so weakened that it can no longer pump enough blood through the body to meet the needs of the organs. As a result, organs, muscles and tissues no longer receive enough oxygen and nutrients. In addition, water accumulates in the legs, abdomen and lungs. Around 210,000 Swiss people currently suffer from heart failure (as of 2020), and older people are particularly frequently affected. The most common symptoms are shortness of breath, swollen legs, increasing fatigue and performance intolerance. However, various other symptoms such as palpitations, nausea, loss of appetite and digestive problems can also occur.
Heart failure: causes and risk factors
Since a wide variety of heart diseases can lead to heart failure, the causes are manifold. However, heart failure is often the result of a long-standing condition, such as high blood pressure or so-called
coronary heart disease
(narrowing of the coronary arteries). The narrowing of the coronary arteries that often occurs in old age leads to reduced blood flow to the heart and thus to an undersupply of oxygen to the heart. If the heart no longer receives enough oxygen and nutrients, its pumping capacity decreases and heart failure develops. In addition to these diseases, however, there are also numerous other causes of heart failure, some of which can be remedied or improved, which is why careful diagnostics form the basis of any good therapy.
High blood pressure, which is very common and unfortunately often inadequately treated, should also be emphasized. The heart has to “overcome” arterial blood pressure in order to pump blood into our body. If the heart has to pump against high blood pressure for years, this often leads to a thickening and stiffening of the left ventricle. The reason: it has to constantly work against high resistance in order to distribute the blood throughout the body despite high blood pressure. The thickening makes the left ventricle less flexible, so that its absorption capacity is restricted. If less blood can flow into the left ventricle, it accumulates in the atrium and lungs. This is also a common form of heart failure. Over a long period of time, this imbalance weakens the heart, which can ultimately lead to pronounced cardiac insufficiency with dilation of the heart chambers.
In addition to high blood pressure and coronary heart disease, there are other heart conditions that can lead to heart failure. These include:
- Myocarditis
- So-called storage diseases
- Heart valve defects
- Congenital heart defects
- Genetic diseases affecting the heart
- Cardiac arrhythmias
- Diseases of the lungs: pulmonary hypertension
Unhealthy lifestyle
Heart disease is often caused by an unhealthy lifestyle. Many of those affected are overweight, smoke, drink too much alcohol or have too much cholesterol in their blood. However, heart disease can also be the result of another disease such as diabetes mellitus. This so-called diabetes is often also associated with an unhealthy lifestyle. The risk of a diabetic developing coronary heart disease is more than twice as high compared to non-diabetics, regardless of age, gender, blood pressure, cholesterol levels or obesity. For this reason, all diabetics should undergo a thorough assessment of their cardiovascular risk and additional cardiac risk factors should be controlled as closely as possible.
Symptoms of heart failure
Initially, there are usually hardly any symptoms. This is mainly due to the fact that the body takes measures to normalize blood circulation:
- The heart beats faster,
- the blood vessels become narrower,
- the body produces more blood and
- the heart muscle increases in volume to compensate for the reduced pumping capacity.
In this way, the body tries to maintain circulation and supply all organs with sufficient oxygen and nutrients. This works for a few months, but sooner or later these compensation mechanisms reach their limits. Typical symptoms of heart failure therefore develop over time.
Typical signs of heart failure
If the left ventricle is weak, those affected usually breathe quickly and shallowly and have the feeling that they are not getting enough air. Shortness of breath (dyspnoea) is a possible sign of left heart failure. Attacks of breathlessness often occur at night in particular, as lying flat has an unfavorable effect on the pressure conditions in the heart and lungs and, in addition, water that has leaked into the tissue during the day sometimes passes back into the vascular system during the night. A general undersupply of oxygen-rich blood leads to increasing performance intolerance and fatigue. Memory performance can also decrease over time. Sometimes a blue discoloration of the lips can also occur, and in advanced stages patients often suffer from cold hands and feet.
Other possible symptoms are
- Restlessness
- Pulmonary edema (water in the lungs)
- Cough
If the right ventricle is mainly affected, this is referred to as right heart failure. Many sufferers keep waking up at night because they have to go to the toilet. This is due to the fact that during flat lying, accumulated fluid from the tissue passes back into the blood and is then increasingly excreted via the kidneys. If the right heart failure progresses further, the water retention can increase. The legs are usually affected first, followed later by the side of the abdomen or the buttocks. Another typical and often clearly visible sign of right heart failure is congested neck veins.
This type of congestion often affects other organs as well. If the stomach is affected, there is sometimes a feeling of fullness and loss of appetite. If blood accumulates in the liver, its volume increases considerably, and over a longer period of time this can even lead to remodeling processes and a certain loss of liver function. If water retention is pronounced, those affected may gain more than two kilograms in weight within a few days.
If both heart chambers are affected, those affected suffer from so-called global heart failure. In this case, the typical symptoms of both right and left heart failure occur.
Heart failure – symptoms often unspecific
However, not every sick person always has all these symptoms. It is often difficult for a layperson to correctly classify the symptoms of heart failure. If you suffer from shortness of breath, become exhausted quickly or notice water retention, you should therefore have yourself checked. In this way, if the worst comes to the worst, you will receive an early diagnosis and can avoid or delay serious complications.
Possible complications of heart failure
Severe heart failure can lead to pulmonary edema, i.e. accumulation of water in the lungs, which can have fatal consequences. If vital organs are undersupplied, a so-called cardiogenic shock can also occur, a condition that is acutely life-threatening and requires immediate intensive medical measures. Such complications require immediate hospitalization. In the intensive care unit, the heart can be relieved both medically and mechanically with so-called cardiac support systems . In addition, a quick diagnosis can be made in order to treat any remediable causes.
A heart attack, i.e. an acute circulatory disorder of the heart itself, is also a possible consequence of advanced cardiac insufficiency. It can also lead to the formation of blood clots in the heart, which can trigger a pulmonary embolism or a cerebral infarction(stroke).
Diagnosis of heart failure
First of all, we will ask you whether you have any pre-existing medical conditions and whether you are taking any medication (medical history). This is how we find out whether you suffer from an underlying disease such as diabetes, which is associated with an increased risk of heart failure. As the extent of alcohol consumption also influences the likelihood of heart failure, we also ask about your alcohol consumption.
After the interview, we will examine you:
- We listen to your heart and lungs to identify possible signs of heart failure, such as a third or fourth heart sound or water in the lungs.
- We also measure your heart rate and blood pressure.
- We will also look for water retention in the legs and check the superficial veins in the neck to see if there is any evidence of blood backing up in front of the heart
- We also take blood samples to look for certain indications of heart failure as well as to check for a number of causes and risk factors.
Further diagnostic procedures are:
- Urine test: If heart failure is present, a urine test can help to identify certain causes of heart failure. In addition, a urine test allows conclusions to be drawn about kidney function in the event of pre-existing kidney function impairment, a common side effect of heart failure.
- X-ray. In addition to the clinical examination, we use an X-ray of the chest to detect water retention in the lungs. In addition to water retention, the size and shape of the heart silhouette can also provide indications of the presence and type of heart failure. This is an important indicator of heart failure, as heart failure often leads to an enlargement of the heart.
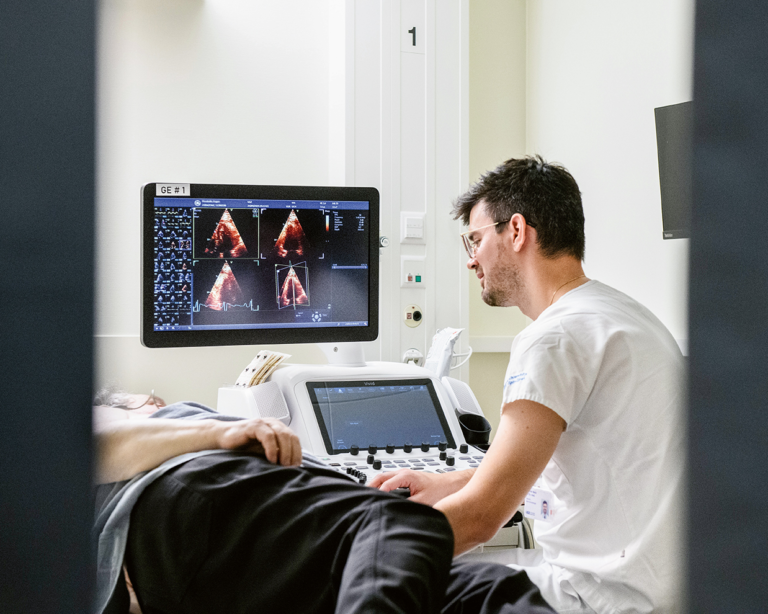
- However, the most important diagnostic procedure is echocardiography, an ultrasound examination of the heart. During this examination, the size and function of the heart chambers in particular, but also valve function and other structural abnormalities can be assessed.
- In addition, the electrocardiogram (ECG, cardiac current curve) provides important information that can contribute to the diagnosis of heart failure. In addition to rhythm disturbances or disturbances in the propagation of the excitation, indications of an increase in the muscle mass of the heart or a decrease in cardiac output can be derived.
Heart failure: prevention and prognosis
There are four stages of symptoms caused by heart failure:
- In the first stage, the heart is already weakened, but there are no noticeable symptoms yet.
- In the second stage, those affected notice shortness of breath during everyday activities such as climbing stairs.
- In the third stage, even light exertion is enough to cause shortness of breath and exhaustion.
- In the fourth and final stage, those affected also complain of symptoms such as shortness of breath or coughing at rest.
So if you notice that you are becoming less and less resilient, consult your doctor as soon as possible. In this way, you can improve your prognosis and increase your quality of life.
Progression and prognosis of heart failure
Cardiovascular diseases, which often lead to heart failure, are among the most common causes of death in Switzerland. The life expectancy of those affected depends on their general health, age and lifestyle. On average, however, the probability of survival is often shorter than for most cancers, with the result that around a third of patients die within the first year of being diagnosed with heart failure. If the heart failure is recognized in the early stages and the patient is still young, the prognosis is better. However, prognosis and well-being depend heavily on good therapy and the control of other risk factors such as high blood pressure, cholesterol levels, diabetes and inhaled cigarette smoking. If you maintain a healthy lifestyle and seek medical treatment, you can have the best possible positive influence on your prognosis.
So if you have been diagnosed with heart failure, it is important to adjust your lifestyle. If you are a smoker, it is best to stop using nicotine completely as soon as possible. This measure alone can increase your life expectancy. If you suffer from other illnesses, have them treated.
You will also improve your prognosis if you treat other diseases well. This includes in particular
Mental illness also has an impact on your life expectancy. You should therefore also seek psychotherapeutic support if necessary.
Heart failure: how to prevent it
You may be able to prevent heart failure by treating existing conditions properly and maintaining a healthy lifestyle. High blood pressure and coronary heart disease are very common causes of heart failure – diseases that are both positively influenced by a healthy lifestyle. You can protect yourself,
- by getting enough exercise,
- Become or stay a non-smoker,
- Reduce excess weight and
- ensure moderate alcohol consumption.
If we have already diagnosed you with high blood pressure, take your medication regularly. If you notice any unpleasant side effects, do not simply stop taking the preparations, but talk to your doctor.
Heart failure treatment
In order to increase quality of life and life expectancy, it is necessary to treat the underlying disease. This is usually due to high blood pressure or coronary heart disease.
In addition to the elimination of possible constrictions in your coronary arteries, if you suffer from coronary heart disease, drug therapy with so-called beta blockers, ACE or ARN inhibitors and possibly mineralocorticoid antagonists is essential. With the help of water tablets, so-called diuretics, the water balance can be regulated so that you suffer as little as possible from breathlessness, which significantly improves your quality of life.
In addition to drug therapy, some patients also benefit from specialized pacemakers or implantable defibrillators, which protect against sudden cardiac death. Some patients are even eligible for a heart transplant and/or implantable mechanical ventricular assist device. Although heart failure cannot be cured, thanks to good treatment and a healthy lifestyle, you can gain time with a good quality of life.
Frequently asked questions about heart failure
The signs of heart failure are shortness of breath on exertion or when lying down, tiredness and rapid exhaustion, water retention in the legs or abdomen, sudden weight gain, the urge to urinate at night, coughing as well as palpitations or an irregular pulse, dizziness and problems concentrating. If these symptoms occur, a doctor should be consulted immediately.
Heart failure cannot usually be cured, but it can be treated well. In some cases, cardiac function can improve, for example in the case of treatable causes. Medication, lifestyle changes and medical measures can slow down progression and improve quality of life.
The following should be avoided if you have heart failure:
- Too much salt – promotes water retention and puts a strain on the heart
- Excessive fluid intake – Can lead to edema and shortness of breath (follow medical advice)
- Alcohol and nicotine – damage the heart
- Excessive physical exertion – exertion should be adjusted individually
- Overweight – Increases heart strain, healthy diet is important
- Stress and lack of sleep – can have a negative impact on blood pressure and heart rate
- Certain medications – painkillers such as ibuprofen or diclofenac can be harmful (seek medical advice)
A heart-healthy lifestyle can help to stabilize the disease and improve quality of life.
Life expectancy in heart failure depends on the severity, cause, treatment and individual lifestyle. With early diagnosis, modern treatment and healthy habits, many sufferers can live for many years or even decades with a good quality of life.